Cheap, decades-old transplant drug delays full onset of type 1 diabetes
A transplant drug that has been used for decades can preserve the function of insulin-producing cells in young children who are newly diagnosed with type 1 diabetes.


An inexpensive drug that's been used for decades in transplant surgeries can delay the progression of type 1 diabetes in those newly diagnosed, new research suggests.
In previous studies, a high dose of the immune-suppressing drug polyclonal antithymocyte globulin (ATG) reduced the loss of insulin-making cells in the pancreas, called beta cells. The new study shows that a much smaller dose is almost as effective at slowing disease progression in type 1 — but with fewer side effects.
In type 1 diabetes (T1D), the immune system destroys the body's beta cells, which produce insulin, the hormone that allows glucose from the blood to enter cells, where it is used as fuel. Without enough insulin, glucose piles up in the bloodstream.
But there's a window of time soon after diagnosis, called the "honeymoon phase," in which beta cells still produce some insulin; this provides an opportunity to keep those remaining beta cells alive longer. A longer honeymoon phase and more residual beta cell function are tied to reduced risk of diabetes complications, such as heart and kidney disease, down the line.
It's this honeymoon phase that the new study was targeting. The study included 117 participants, who were between the ages of 5 and 25 and had been diagnosed with type 1 diabetes within nine weeks of starting the trial. The participants received either a high, intermediate or low dose of ATG: the high dose was equivalent to 2.5 milligrams of ATG per kilogram of body weight; the intermediate dose was 1.5 mg/kg; and the low dose was 0.5 mg/kg of body weight.
The researchers found that the lowest dose preserved beta cell functioning for a year, according to the paper published Sept. 27 in the journal The Lancet.
The trial was designed to help researchers analyze the lowest effective dose in children as young as 5 years old, lead study author Dr. Chantal Mathieu, endocrinologist at the University Hospital Gasthuisberg Leuven in Belgium, told Live Science. That's because the drug's side effects — such as harmful immune reactions — can be especially hard on them, she said.
Get the world’s most fascinating discoveries delivered straight to your inbox.
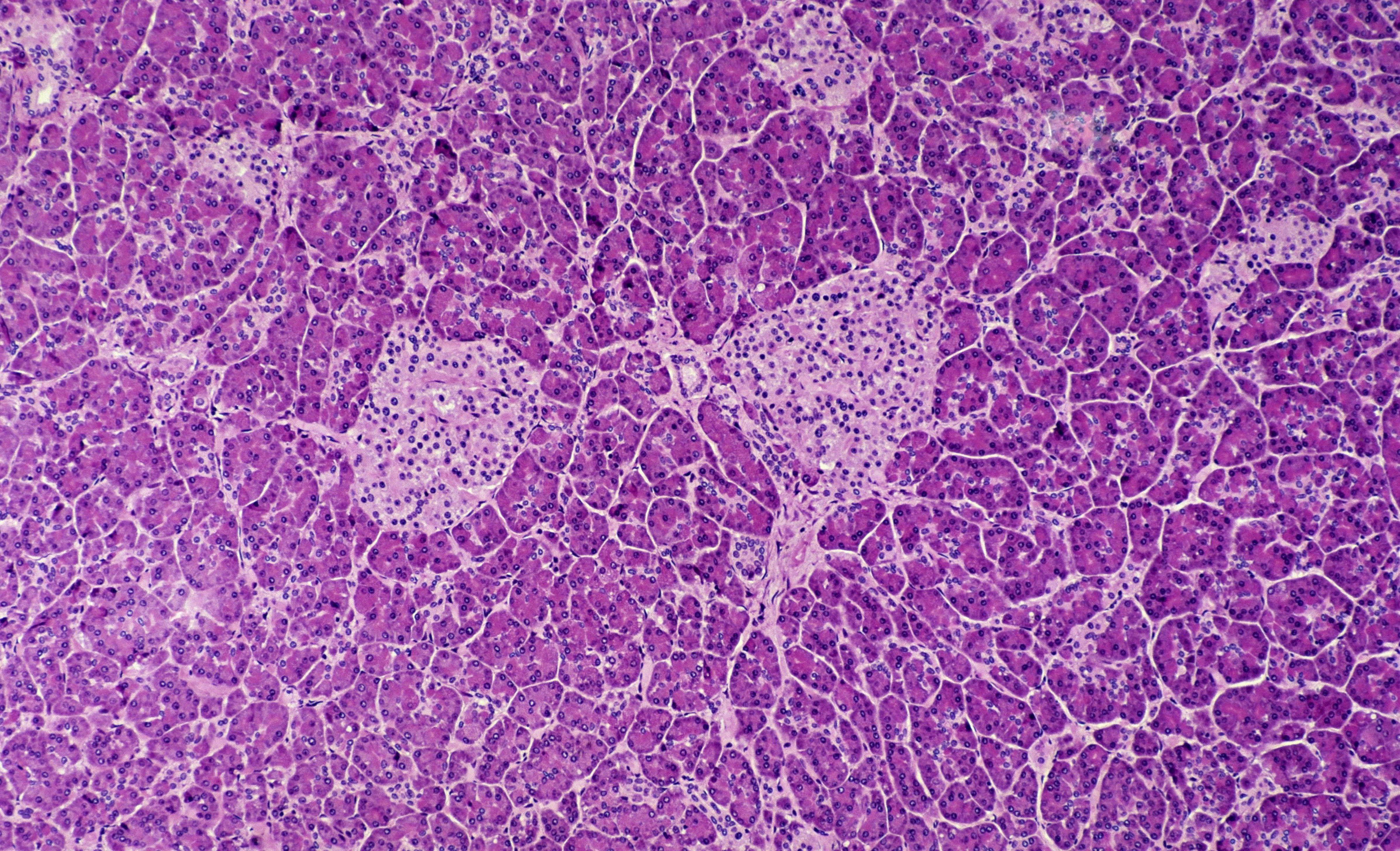
In type 1 diabetes, the immune system destroys beta cells located found in the islets of Langerhans in the pancreas (shown here).
"The ATG worked wonderfully," she said. The beneficial effect "was the biggest in the smallest children."
This was the third study to confirm the effectiveness of ATG to delay beta cell loss, Mathieu added.
Notably, when researchers reviewed the data, they found a similar level of side effects in the intermediate- and high-dose groups, so they dropped the intermediate dose from further study. The biggest difference between the remaining high- and low-dose groups was the incidence of side effects. One of the most common ATG side effects is serum sickness, an immune reaction to foreign proteins that can be triggered by drugs made in the cells of other animals. (ATG is produced in the cells of rabbits and horses.) In the new study, serum sickness impacted 82% of the participants in the high-dose group and just 32% in the low-dose group.
Meanwhile, in the low-dose group, 24% had cytokine release syndrome, a runaway inflammatory response that can include fever, nausea, fatigue, headache, and muscle and joint pain. About 33% of the participants who received the higher dose developed the syndrome.
"I think the reason this is somewhat promising is that it's now one of a handful of drugs that show you can delay type 1 diabetes somewhat," Mathieu said. Another benefit of ATG, Mathieu said, is that it's inexpensive and widely available.
Other medications that have been found to delay diabetes are teplizumab-mzwv (brand name Tzield) and baricitinib (Olumiant). Tzield is given as a 14-day infusion, but it's only approved for use in "stage 2" diabetes — at which point the body has been making antibodies to insulin and has some abnormal blood sugar responses, but most of its insulin-making cells are still working. Few people are diagnosed with diabetes in this early stage, which limits the drug's reach.
Meanwhile, baricitinib — a rheumatoid arthritis drug that hasn't yet been tested in children with diabetes — must be taken continuously to prevent disease progression.
Good news for young children
Dr. Jennifer Sherr, an endocrinologist and professor of pediatrics at Yale School of Medicine, who was not involved in the study, said the results were encouraging, especially for families who would find it extremely challenging to take off from work for their child to receive two days of infusions. In the study, those in the low-dose group received an infusion on the first day and a placebo on the second day, but the placebo day wouldn't be necessary if the drug were given outside a clinical trial, she noted.
Sherr also liked that the study included 5- to 11-year-olds. "Those are the kids who lose their beta cells so fast" after diagnosis, Sherr told Live Science. "Their insulin needs go up incredibly."
Sherr hopes that this less-expensive medication could ultimately be approved for use in diabetes to help give "kids a smoother ride," she said.
As for whether ATG is better than other alternatives demonstrated to delay progression, "many people think it's going to take a multi-agent approach," she said. In other words, to really stop T1D in its tracks, people would likely need to get multiple drugs, Sherr said.
It's premature to say one treatment is better than another. "I think what gives us hope for the future is [that] there are lots of things we can consider," Sherr said.
And in a clinical trial set to begin late this year or early next year, researchers will test a next-generation version of ATG made in genetically modified cows in people newly diagnosed with type 1 diabetes.
RELATED STORIES
The new drug, made by SAB BIO and called SAB-142, is grown in a cow that has been gene edited to produce human antibodies, said lead researcher Dr. Michael Haller, chief of pediatric endocrinology at the University of Florida's Diabetes Institute and advisory board member for SAB BIO. . "The cow can then donate blood," from which the human antibodies are harvested, Haller told Live Science in an email.
The hope is that, because the antibodies are made using human genes, they will no longer trigger serum sickness in patients. The human antibodies are also less likely to cause the immune system to produce antibodies that block the drug's action, so in theory, Haller said, "the new drug may be safer and even more effective in type 1 diabetes."
Editor's note: Haller holds stock options in SAB BIO, in addition to being an advisory board member.
This article is for informational purposes only and is not meant to offer medical advice.

Theresa Sullivan Barger is an award-winning freelance journalist who covers health, science, and the environment. Her stories have appeared in The New York Times, The Boston Globe, Los Angeles Times, AARP, CURE, Discover, Family Circle, Health Central, Next Avenue, IEEE Spectrum, Connecticut Magazine, CT Health Investigative Team, and more. Based in central Connecticut, she is an advanced master gardener who is passionate about gardening for wildlife, especially pollinators and songbirds.
You must confirm your public display name before commenting
Please logout and then login again, you will then be prompted to enter your display name.

 Live Science Plus
Live Science Plus




