Type 1 diabetes: Symptoms, causes and treatment
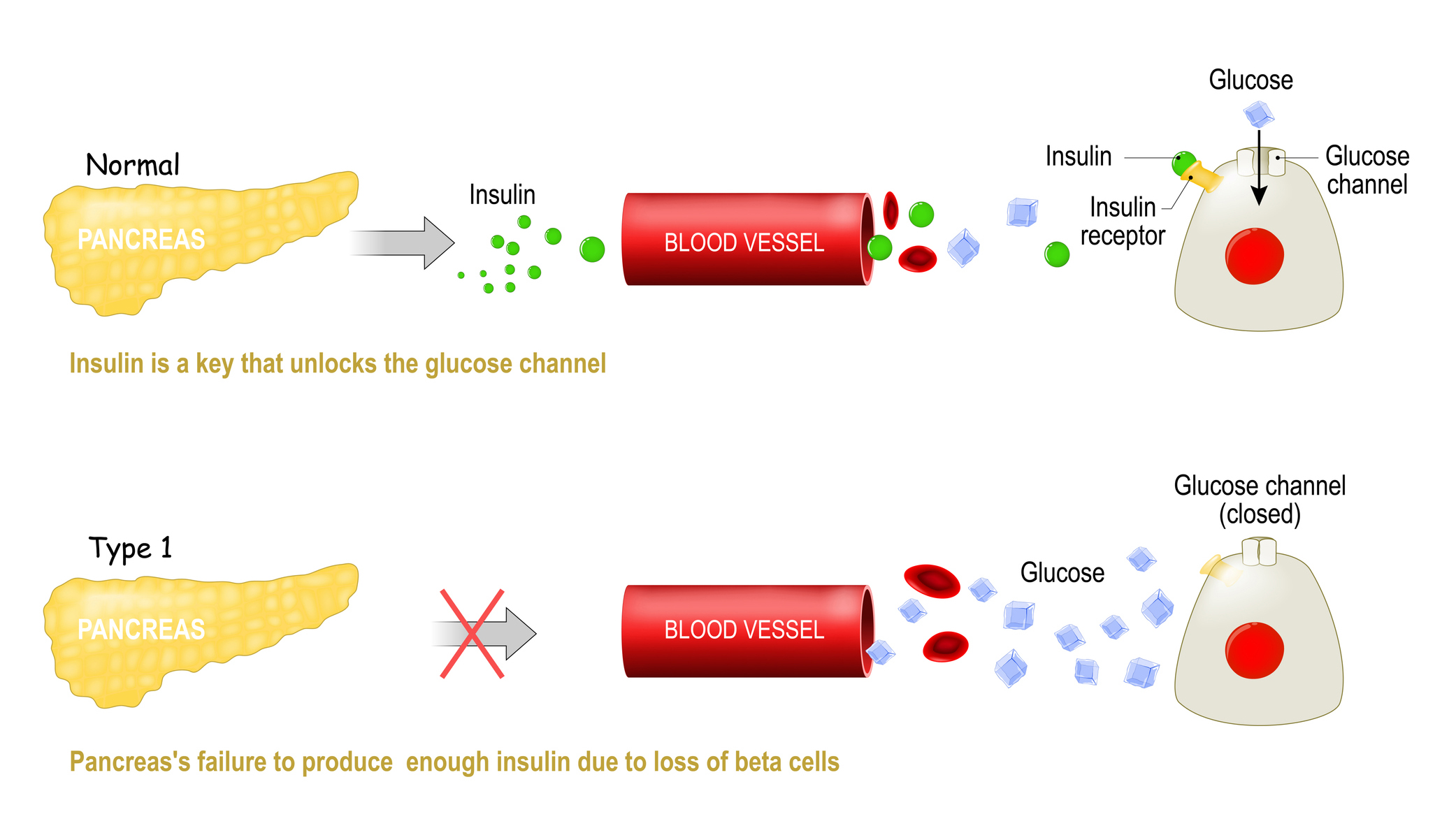
Type I diabetes is a disease where the pancreas stops producing insulin, a hormone that lets the body's cells absorb glucose from the bloodstream.
Get the world’s most fascinating discoveries delivered straight to your inbox.
You are now subscribed
Your newsletter sign-up was successful
Want to add more newsletters?
Join the club
Get full access to premium articles, exclusive features and a growing list of member rewards.
Type 1 diabetes, once referred to as juvenile diabetes or insulin-dependent diabetes, is a chronic condition characterized by high blood sugar, or glucose.
It occurs when the immune system mistakenly attacks the cells in the pancreas that make the hormone insulin, resulting in the inability of the body to produce enough insulin to keep blood sugars in check. Insulin is crucial for glucose metabolism; it helps shepherd sugar from the bloodstream into the body's cells for energy. Without insulin, glucose builds up in the blood, which, over time, can trigger life-threatening complications. (In people with type 2 diabetes, the body doesn't produce enough insulin, or does not use the insulin efficiently.)
Type 1 diabetes is frequently diagnosed in children, adolescents or young adults, but it can develop at any age. People with this form of diabetes need to take insulin every day to stay alive.
Article continues belowIn 2019, 37.3 million Americans had diabetes (diagnosed and undiagnosed), of which 1.9 million had type 1 diabetes, according to the American Diabetes Association (ADA).
Causes & risk factors
The exact cause of type 1 diabetes is unclear, according to the National Library of Medicine (NLM). However, scientists think genetics and environmental factors, such as exposure to a virus, can cause the body to mistakenly attack key cells in the pancreas that make insulin.
Some known risk factors for this form of diabetes include a family history of type 1 diabetes, the presence of certain genes and geography; turns out, the incidence of the disease is higher the farther away one is from the equator, possibly due to UV radiation and vitamin D deficiency, according to several scientific reports, such as a study published in 2017 in the journal Photochemical & Photobiological Sciences. And although the disease can develop at any age, it seems to often strike during two periods: in children between 4 and 7 years old, and in children between 10 and 14 years old, according to the Mayo Clinic.
Symptoms & complications
The inability to produce insulin can result in a constellation of symptoms, which usually appear very quickly over a few days and weeks, according to the National Institute of Diabetes and Digestive and Kidney Diseases. These symptoms may include increased thirst, hunger and urination; blurred vision; fatigue; and unexplained weight loss.
Get the world’s most fascinating discoveries delivered straight to your inbox.
"What we see in children is that they start being hungry and thirsty, and they're urinating a lot," Dr. Spyros Mezitis, an endocrinologist at Northwell Health in New York told Live Science. "They're feeling weak; they're losing weight."
Sometimes, the first sign of type 1 diabetes is a life-threatening condition called diabetic ketoacidosis (DKA), which occurs as a result of drastically low levels of insulin in the body, according to the NLM. Symptoms of DKA may include breath that smells fruity, dry or flushed skin, nausea or vomiting, stomach pain, breathing difficulties, confusion and inability to concentrate. DKA occurs when the body can't use sugar for energy, so it turns to fat instead. As a result of this process, compounds called ketones are released, causing the blood to become acidic and, in turn, toxic. If left untreated, DKA can be deadly.
Over time, uncontrolled blood sugar levels in people with diabetes can lead to a host of complications affecting major organs, triggering serious problems such as heart attack, stroke, blindness and kidney failure.
Diagnosis
If a doctor suspects diabetes, they will use a range of blood and other tests to make a diagnosis. For type 1 diabetes, in particular, the favored test is a random blood sugar test. The random blood sugar test measures blood sugar at the time of testing, and fasting is not required. A blood sugar level of 200 milligrams per deciliter (11.1 millimolar/liter) or higher indicates diabetes. But this measure and other blood tests don't discern whether the individual has type 1 or type 2 diabetes.
Knowing the type of diabetes is crucial because it determines the treatment regimen, according to the Centers for Disease Control and Prevention (CDC). If type 1 diabetes is suspected, doctors may test for certain autoantibodies that attack the body' beta cells. Particular autoantibodies are common in type 1 diabetes, but not in type 2, and include: islet cell antibodies (ICA, against cytoplasmic proteins in the beta cell), antibodies to glutamic acid decarboxylase (GAD-65), insulin autoantibodies (IAA), and IA-2A, to protein tyrosine phosphatase, according to Johns Hopkins Medicine.)
Other tests that help a doctor to diagnose diabetes, before determining the type, include:
- A fasting plasma glucose test reveals how effectively the body metabolizes glucose and requires the patient to fast for eight hours before taking the test. Normal blood sugar levels vary from person to person, but a normal range for fasting blood sugar is between 70 and 100 mg/dL (3.9 and 5.6 mmol/L), according to the World Health Organization. And a result of more than 126 mg/dL (7.0 mmol/L) of glucose in the blood signals diabetes.
- The oral glucose tolerance test requires the patient to consume an extra-sugary drink. Two hours later, the person undergoes a blood test. A result of 200 mg/dL or greater of glucose in the blood is considered a sign of diabetes.
- The A1C blood test shows average blood glucose over the preceding three months. The test measures glucose attached to hemoglobin, the oxygen-carrying protein in blood. The red blood cells that carry this protein live for about three months, so measuring them at a single time point provides a snapshot of the general level of glucose in the blood. An A1C result of less than 5.7% is normal; between 5.7% and 6.4% suggests prediabetes; and 6.5% or greater indicates diabetes.
Prevention & treatment
Scientists have not yet found a way to prevent type 1 diabetes, but researchers are currently working on ways to cease the destruction of insulin-producing cells in the pancreas in people who are newly diagnosed, the Mayo Clinic says. TrialNet — an international network of institutions and doctors working on type 1 diabetes research — has several clinical trials in the works for preventive measures. For instance, this network is testing whether a drug called Abatacept could delay or prevent the progression of the disease according to TrialNet. Another drug, called teplizumab, was found to delay the progression of type 1 diabetes for a median of two years, according to TrialNet.
Those who develop kidney failure and receive a kidney transplant, will sometimes also receive a transplant of pancreatic islet cells from an organ donor at the same time. Islet transplants may free them from the need to use insulin, potentially for many years, but requires taking lifelong immunosuppressive drugs according to the National Institute of Diabetes and Digestive and Kidney Disorders.
But the vast majority of people with type 1 diabetes require lifelong insulin therapy and will need to monitor their blood sugar levels frequently.
People with type 1 diabetes need to take insulin both to cover basic metabolic functions (called basal insulin) and to regulate the blood sugar produced by eating (called bolus insulin). To handle the blood sugar spikes caused by food, insulin shots are typically timed with meals and, once a routine is established, are done several times per day. Other options for administering insulin include a "pen," which allows for smaller doses (or boluses) of insulin to be injected, and a pump, which is attached to the body and delivers insulin throughout the day through a tiny tube that is inserted just beneath the skin surface, according to the ADA.
Insulin can cause low blood sugar, or hypoglycemia, which may cause feelings of weakness, hunger and headaches. Prolonged and severe low blood sugar can cause seizures, coma and death.
There are several different types of insulin: Some last from about 18 hours to an entire day (called intermediate and long-acting, respectively); others, called rapid-acting insulin, enter the bloodstream in a few minutes and works most powerfully for an hour or twos; and regular- or short-acting insulin enters the bloodstream in about 30 minutes and is active for 3 to 6 hours, according to WebMD. People with type 1 diabetes may take long-acting insulin, which the body absorbs slowly, to provide the body’s basal metabolic need for insulin, while the rapid-acting insulin is used for meals.
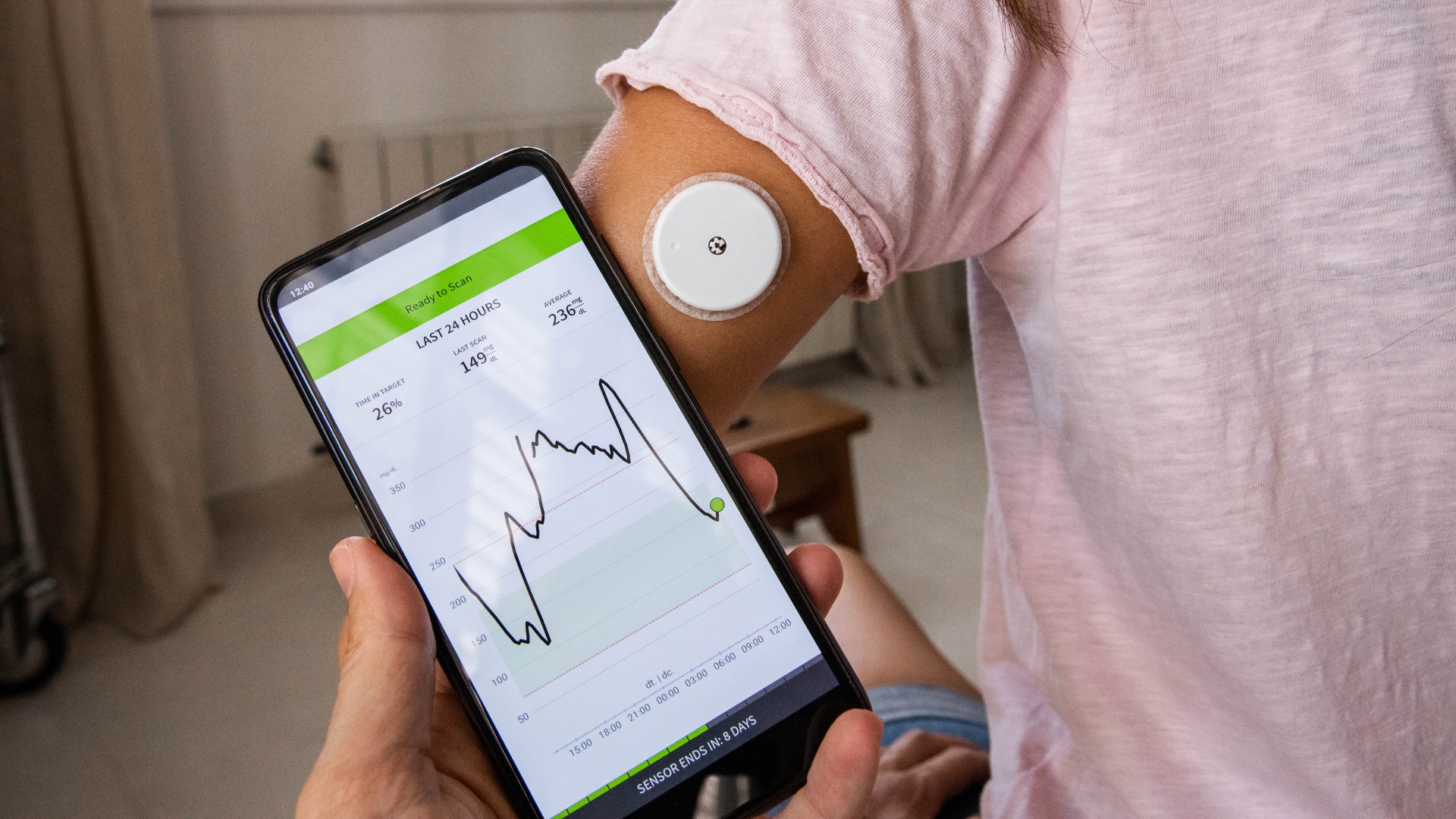
In 2016, the U.S. Food and Drug Administration approved the use of a so-called "artificial pancreas" — essentially a pump that uses a continuous glucose monitor to detect blood glucose levels and then automatically adjusts insulin dosing in response to those numbers, Live Science previously reported.
At the moment, there is no cure for type 1 diabetes, but research is ongoing. In order to rid someone of type 1 diabetes, the cure would need to both stop the immune system from destroying the body's beta cells and replace the already-lost beta cells successfully, according to the Juvenile Diabetes Research Foundation (JDRF). In 2021, the company Vertex announced a patient with type 1 diabetes was the recipient of a stem-cell therapy to replace their beta cells; and 90 days after the infusion, the person was using 91% less insulin, though the person also needs to continue immunosuppressive therapy to keep the body from killing off those replacement cells.
This article is for informational purposes only and is not meant to offer medical advice.
This article was updated on April 11, 2022, by Live Science contributor Natalie Grover, with additional reporting by Joseph Brownstein, MyHealthNewsDaily contributor.
Additional resources
- Learn more about the latest research on the hunt for a type 1 diabetes cure in this report by The New York Times.
- Read about how the prevalence of type 1 diabetes in American youth is on the rise in this report by the CDC.
- Check out the children's book "Year One with Type One: A True Story of a Boy with Type 1 Diabetes" (Owl Eye Books, 2018), by Mike Suarez, inspired by his son's journey with the disease.
Bibliography
"Statistics About Diabetes," American Diabetes Association
https://www.diabetes.org/resources/statistics/statistics-about-diabetes
"Type 1 diabetes," The Mayo Clinic
https://www.mayoclinic.org/diseases-conditions/type-1-diabetes/diagnosis-treatment/drc-20353017
"Type 1 Diabetes," National Institute of Diabetes and Digestive and Kidney Diseases
https://www.niddk.nih.gov/health-information/diabetes/overview/what-is-diabetes/type-1-diabetes
"Type 1 Diabetes," National Library of Medicine
https://medlineplus.gov/genetics/condition/type-1-diabetes/
"What Is Type 1 Diabetes?" Centers for Disease Control and Prevention
https://www.cdc.gov/diabetes/basics/what-is-type-1-diabetes.html
"Diabetic ketoacidosis," National Library of Medicine
https://medlineplus.gov/ency/article/000320.htm
"Diabetes Tests," Centers for Disease Control and Prevention
https://www.cdc.gov/diabetes/basics/getting-tested.html

Laura is the managing editor at Live Science. She also runs the archaeology section and the Life's Little Mysteries series. Her work has appeared in The New York Times, Scholastic, Popular Science and Spectrum, a site on autism research. She has won multiple awards from the Society of Professional Journalists and the Washington Newspaper Publishers Association for her reporting at a weekly newspaper near Seattle. Laura holds a bachelor's degree in English literature and psychology from Washington University in St. Louis and a master's degree in science writing from NYU.
 Live Science Plus
Live Science Plus