Vasectomy: Procedure, risks and reversal
Half a million men in the United States undergo a vasectomy every year. But how does this procedure work?

Joe Phelan

A vasectomy is a form of birth control for men. This minimally invasive surgical procedure prevents sperm from entering the semen and then being released during ejaculation.
According to the Centers for Disease Control and Prevention (CDC), a vasectomy is a minor surgery to cut or seal the vas deferens — the tube that connects the testes to the penis. Because sperm cells are produced in the testes, they can no longer be transported into the semen and therefore cannot cause pregnancy.
An estimated 500,000 men have a vasectomy every year in the United States, according to the Cleveland Clinic. Many men consider having a vasectomy when they are certain they do not want any more children or do not want children at all.
Dr. Hussain Alnajjar, a consultant urological surgeon at University College London Hospital in the U.K. and honorary associate professor at University College London, said that a vasectomy is the most reliable method for male sterilization. "It should also be regarded as irreversible," he told Live Science in an email. "Vasovasostomy procedure, often referred to as vasectomy reversal, is possible, but it may not always be successful."
How does a vasectomy work?
A vasectomy is a minimally invasive surgery performed by a urologist — a specialist who focuses on anything involving the urinary and reproductive tracts.
The procedure doesn't affect a man's ability to perform sexually or achieve orgasms and it doesn't visibly change semen, said Dr. Paurush Babbar, a urologist at The Urology Group in Cincinnati, Ohio, and a member of the American Urological Association.

Babbar completed both his undergraduate studies and medical school education at Wake Forest University in Winston-Salem, North Carolina, in 2013. He went on to the Cleveland Clinic in Cleveland, Ohio, for his urology residency, which he finished in 2019. Babbar is a member of the American Urological Association and board-certified with the American Board of Urology.
There are two common types of vasectomies: conventional and no-scalpel. During a conventional vasectomy, small cuts are made in the scrotum — the bag of skin that protects the testes — in order to reach the vas deferens tubes. In a no-scalpel vasectomy, no cuts are made during the process — instead the doctor makes a small puncture or incision to reach the vas deferens.
Get the world’s most fascinating discoveries delivered straight to your inbox.
A 2014 review in the Cochrane Database of Systematic Reviews found no difference in effectiveness between the two approaches. However, no-scalpel vasectomies may result in less bleeding, infection and pain, as well as a shorter operation time compared with the conventional technique.
During both types of procedure, the patient is put under local anesthetic. In a conventional vasectomy, a doctor then cuts the vas deferens, Babbar told Live Science in an email. The procedure takes about 30 minutes. Once the incision in the scrotum has been made, the doctor removes a small piece of the vas deferens tube. The ends are sutured, clipped and sealed by cauterization — a practice of burning a part of the body to remove or close it off. The patient also receives two or three stitches close to the incision, Babbar said.
In a no-scalpel vasectomy, a urologist feels for the vas deferens tube and then holds it in place with a clamp. A tiny hole is then made in the scrotum so the tube can be taken out and cut or tied. Afterwards, the vas deferens tube is put back in place.
While the testes continue to make sperm, they are simply reabsorbed back into the body, in exactly the same way as they would if the man did not have sex, said Adam Watkins, an associate professor in reproductive and developmental physiology at the University of Nottingham in the U.K.
It usually takes a few months before the patient is completely sterile, Babbar said. "A physician will confirm sterility with a semen sample two to three months after the vasectomy," he said.
Does a vasectomy work?
A vasectomy is a highly effective method of birth control, according to the Mayo Clinic, with more than a 99% success rate. However, there's always a small chance that pregnancy can occur, according to the CDC.
RELATED STORIES
Despite its effectiveness, a vasectomy does not work immediately and men should use other forms of contraception until post-vasectomy semen analysis, Alnajjar said. This is usually 12 weeks after the procedure or when 20 ejaculations have been deemed negative for sperm, he said.
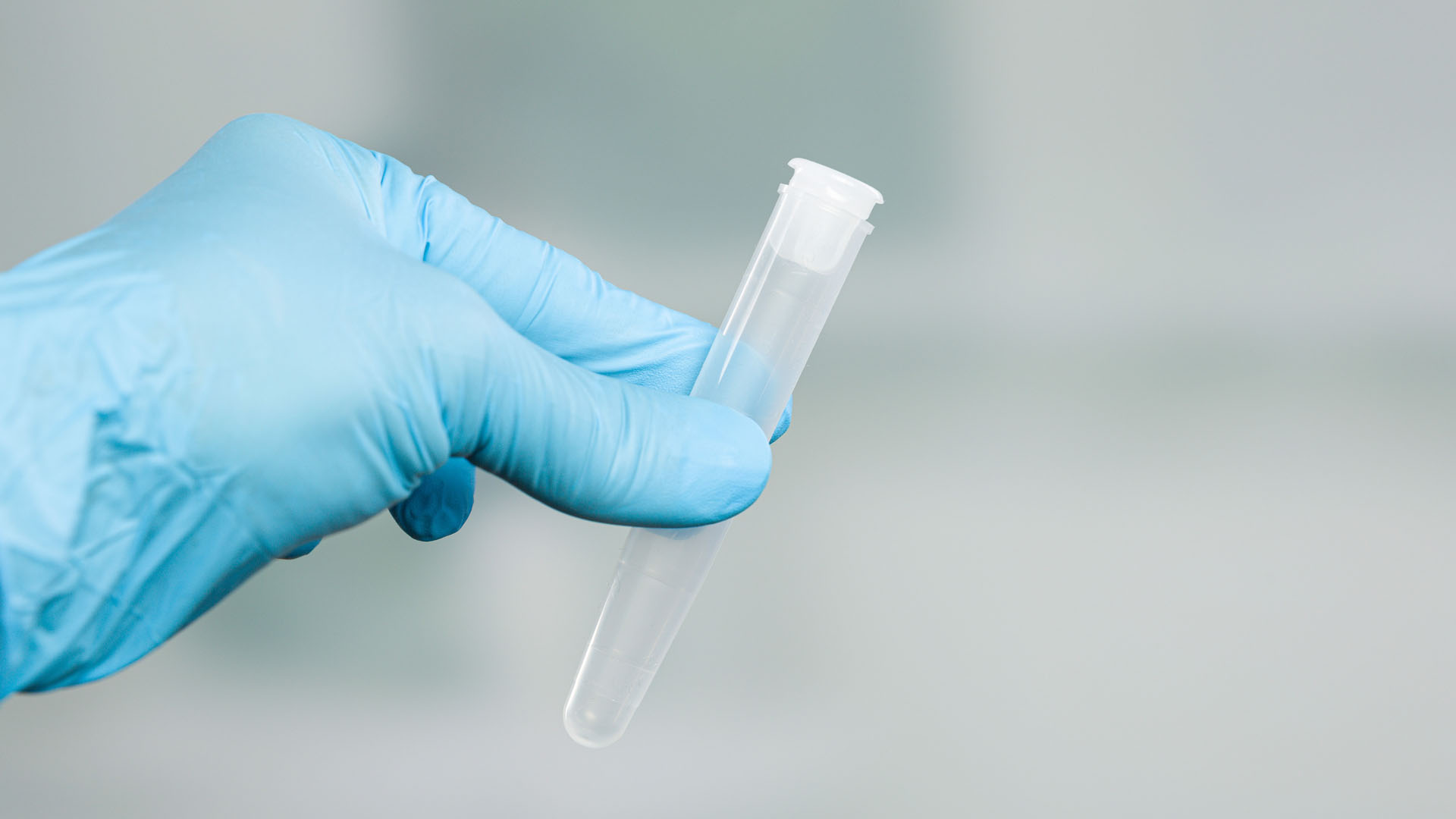
Post-vasectomy semen analysis is usually carried out 12 weeks after the procedure.
A vasectomy carries a small risk of short- and long-term complications, according to a 2021 review published in The World Journal of Men's Health. Most patients experience swelling, bruising and some discomfort for about two weeks after the procedure. These symptoms tend to go away on their own. However, there is a small risk that some patients may develop scrotum infection, hematoma (bleeding under the skin that looks like a bruise) and sperm granuloma (a lump in the scrotum caused by sperm that leaks out of the vas deferens tube into tissue).
Can a vasectomy be reversed?
Though a vasectomy is considered a permanent procedure, it can be reversed, Watkins told Live Science in an email. However, it is trickier to undo a vasectomy than to perform the initial surgery, he said.
"A vasectomy is a fairly routine and quick procedure. While a reversal procedure can be done, there is no guarantee that it will restore a man's fertility," Watkins said. "As such, a vasectomy should only be undertaken if the person is absolutely sure they do not want to have any, or any more, children."
Alnajjar said that vasectomy reversal is performed by re-joining the previously cut ends of the vas deferens using microscopic sutures.
The chance of success for vasectomy reversal is directly related to the time interval between the vasectomy and its reversal, and the age of the female partner, Alnajjar said. According to the Mayo Clinic, pregnancy success rates vary from about 30% to 90%, with the lowest rates applying to men who had a vasectomy over 10 years prior.
In addition, a vasectomy reversal procedure lasts longer (around 2 to 3 hours) and is more expensive than a vasectomy, Babbar said.
This article is for informational purposes only and is not meant to offer medical advice.

Anna Gora is a health writer at Live Science, having previously worked across Coach, Fit&Well, T3, TechRadar and Tom's Guide. She is a certified personal trainer, nutritionist and health coach with nearly 10 years of professional experience. Anna holds a Bachelor's degree in Nutrition from the Warsaw University of Life Sciences, a Master’s degree in Nutrition, Physical Activity & Public Health from the University of Bristol, as well as various health coaching certificates. She is passionate about empowering people to live a healthy lifestyle and promoting the benefits of a plant-based diet.
- Joe PhelanLive Science Contributor

 Live Science Plus
Live Science Plus





