Battling Obesity ... with a Brain Implant?
Get the world’s most fascinating discoveries delivered straight to your inbox.
You are now subscribed
Your newsletter sign-up was successful
Want to add more newsletters?

Delivered Daily
Daily Newsletter
Sign up for the latest discoveries, groundbreaking research and fascinating breakthroughs that impact you and the wider world direct to your inbox.

Once a week
Life's Little Mysteries
Feed your curiosity with an exclusive mystery every week, solved with science and delivered direct to your inbox before it's seen anywhere else.

Once a week
How It Works
Sign up to our free science & technology newsletter for your weekly fix of fascinating articles, quick quizzes, amazing images, and more

Delivered daily
Space.com Newsletter
Breaking space news, the latest updates on rocket launches, skywatching events and more!

Once a month
Watch This Space
Sign up to our monthly entertainment newsletter to keep up with all our coverage of the latest sci-fi and space movies, tv shows, games and books.

Once a week
Night Sky This Week
Discover this week's must-see night sky events, moon phases, and stunning astrophotos. Sign up for our skywatching newsletter and explore the universe with us!
Join the club
Get full access to premium articles, exclusive features and a growing list of member rewards.
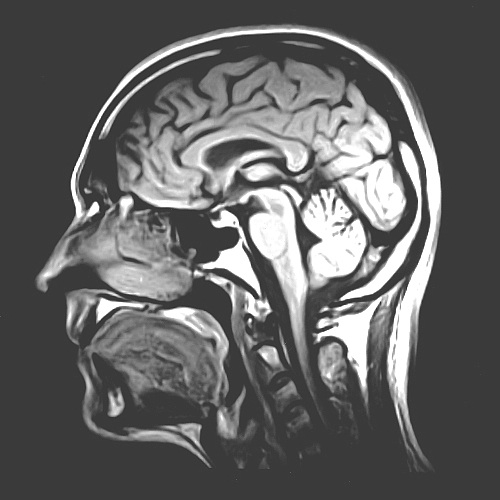
The brain may not seem like an obvious place to look for possible treatments for obesity, but researchers say implanting a device that stimulates a specific region of the brain may help curb the compulsion to overeat.
The new study on obese mice found that deep brain stimulation (DBS), which involves implanting a device that sends electrical impulses to precise targets in the brain, may reduce binge eating and other obesity-related behaviors.
"Once replicated in human clinical trials, DBS could rapidly become a treatment for people with obesity due to the extensive groundwork already established in other disease areas," lead author Casey Halpern, a resident in the department of neurosurgery at the University of Pennsylvania's Perelman School of Medicine, said in a statement. [8 Reasons Our Waistlines Are Expanding]
Farfetched idea?
At first, the idea of using brain implants to treat obesity seemed farfetched, said Tracy Bale, an associate professor of neuroscience at the University of Pennsylvania's School of Veterinary Medicine, and one of the senior authors of the study.
"We had a long discussion about it, and my initial thought was: who on Earth is going to get brain surgery for obesity?" Bale told LiveScience.
But, the researchers were interested in targeting a part of the brain called the nucleus accumbens, which is a small structure in the brain's reward center that is already known to play a part in addictive behaviors, such as binge eating.
Get the world’s most fascinating discoveries delivered straight to your inbox.
"The things that drive people to overeat are part of the reward system," Bale explained. "So, for example, if someone is under a lot of stress, or if they had a bad day, they might reward themselves with food. And bingeing is a component strongly linked with obesity."
Since binge eating and other obesity-related behaviors have been linked to deficits of a chemical called dopamine, the researchers used deep brain stimulation to activate the dopamine type-2 receptor in the nucleus accumbens of mice.
"Mice are just like humans — they love high-fat food," Bale said.
Binge-eating mice
In the experiment, mice were given unlimited access to low-calorie fare, but for one hour each day, they were offered food that was high in fat.
"Within two days, they learned that we take that food away, so they gorged themselves and ate as much as they could," Bale said.
After undergoing deep brain stimulation, however, the mice ate significantly less of the high-fat food, compared with mice that received no such treatment; the treated mice also didn't compensate for the loss of calories by eating more food.
After several days of constant stimulation, the devices were turned off, and the mice resumed their binge-eating behavior.
If deep brain stimulation is eventually used to treat people with obesity, the devices could be switched on constantly, and the strength of the electrical impulses could be adjusted, depending on the individual patient's needs, Bale said. This type of treatment may also be an alternative to risky bariatric surgery, and may be more effective than available pharmaceutical options, Bale said.
"It sounds intimidating, but for this type of surgery, the morbidity rate is much less," she said. "And this could be something for patients who don't respond to drugs. Many drug companies are trying to target obesity by getting people to not feel hungry, but that doesn't work. People aren't overeating because they're hungry. They're eating because it tastes good, or makes them feel better. This treatment taps directly into that reward system."
Deep brain stimulation is already used as a way to help reduce tremors in patients with Parkinson's disease, and scientists are investigating its therapeutic benefits for obsessive-compulsive disorder and depression.
Follow Denise Chow on Twitter @denisechow. Follow LiveScience @livescience, Facebook & Google+. Original article on LiveScience.com.

Denise Chow was the assistant managing editor at Live Science before moving to NBC News as a science reporter, where she focuses on general science and climate change. Before joining the Live Science team in 2013, she spent two years as a staff writer for Space.com, writing about rocket launches and covering NASA's final three space shuttle missions. A Canadian transplant, Denise has a bachelor's degree from the University of Toronto, and a master's degree in journalism from New York University.
 Live Science Plus
Live Science Plus










