Childhood obesity should be treated early and aggressively, new guidelines say. Is that safe?
The American Academy of Pediatrics released new guidelines for treating kids and teens with obesity.

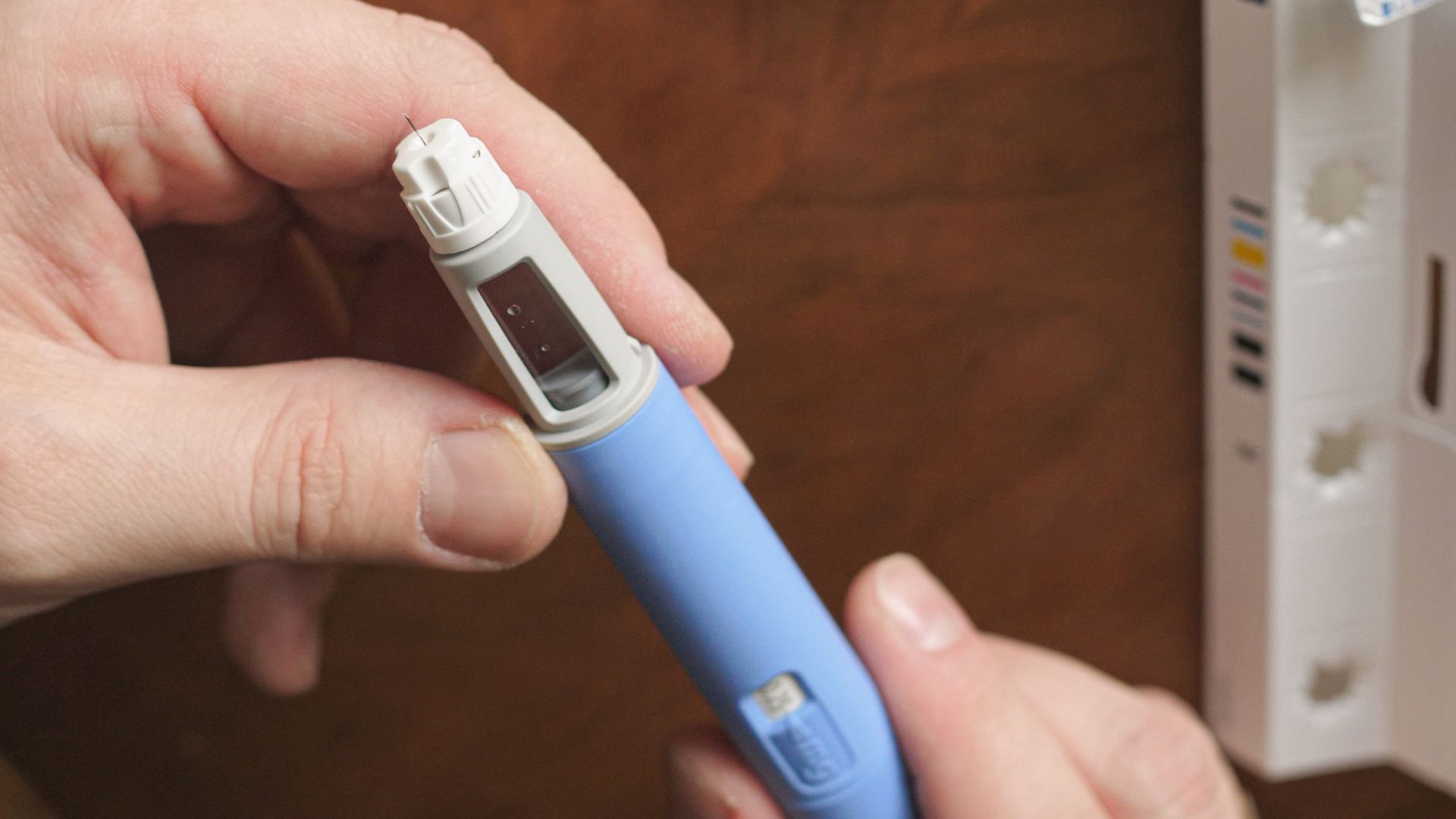
The American Academy of Pediatrics (AAP) released new guidelines for treating children and teens with obesity.
The 73-page guidelines outline a proactive approach, where children and their families receive counseling about weight-loss treatments sooner, rather than later. Treatments include time-intensive programs that address children's nutrition and physical activity, as well as weight-loss drugs for children as young as age 12 and metabolic and bariatric surgeries for teens 13 and older.
The guidelines aim to curb the negative health outcomes linked to untreated childhood obesity. In both the short-term and long-term, kids and teens with obesity face an elevated risk of heart disease, high blood pressure, insulin resistance, prediabetes and type 2 diabetes. Studies suggest that a child's weight is highly predictive of weight in adolescence and adulthood, and the links between obesity and increased health risks in adults are established, the report states. So by having doctors treat obesity early, the AAP is aiming to head off a lifetime of health problems, the authors wrote.
The new guidance received a mixed response, with some experts hailing it as an "overdue and crucial" shift in how American doctors approach childhood obesity. Others argued that it perpetuates anti-fat bias and may prompt physicians to reach for the aggressive interventions as first-line treatments, rather than last resorts.
Live Science asked experts what they think of the guidelines, and they generally agreed that the AAP presented an evidence-based review of childhood obesity and the best available treatments. However, for now, most children likely won't receive the gold standard of care recommended by the guidelines. Thus, there's a risk that harried pediatricians will recommend that children lose weight but lack the time to guide them safely through the process, potentially leaving kids vulnerable to disordered eating, one expert suggested. In addition, scientists are still learning about the long-term consequences of weight-loss drugs, they added.
Related: How body fat is calculated
"I think the challenge is that many patients do not have access, resources, or time to participate in structured and professionally run pediatric obesity treatment," Dr. Jason Nagata, a pediatrician and adolescent eating disorder specialist at the University of California, San Francisco, told Live Science in an email. Outside of these programs, kids recommended weight loss treatment may not be adequately monitored, Nagata said.
Get the world’s most fascinating discoveries delivered straight to your inbox.
"As an eating disorder specialist, I have received many referrals for teens who were previously told they were obese and needed to lose weight, and they took the weight loss to the extreme," he said. Research led by Nagata suggests that, compared with their leaner peers, older teens and young adults with overweight or obesity are more likely to engage in disordered eating behaviors, like fasting, but less likely to be diagnosed with eating disorders than underweight peers. That's dangerous because teens with disorders like anorexia can still be dangerously ill, even if they are not underweight.
Doctors should discourage patients from using dangerous weight control strategies, explain the risks, and monitor the rate and degree of patients' weight loss, Nagata said, and AAP gives similar, if brief, guidance in its report. But many doctors have limited training in eating disorders and limited time to interact with their patients, Nagata said, so ensuring that kids receive this type of care could be tough.
The AAP also provides examples of neutral language to use in conversations about a child's weight, and broadly, the guidelines frame obesity as a complex, chronic disease influenced by myriad factors, from genetics to socioeconomics, rather than a "reversible consequence of personal choices," as it's been considered in the past, the guidelines authors wrote.
The guidelines emphasize "treating the whole child," rather than fixating on a number on a scale, Dr. Sheethal Reddy, a clinical psychologist who specializes in obesity medicine at the Emory Bariatric Center, told Live Science. "The goal here is not to get kids skinny — it's not to have them fit into a certain size pair of pants," said Reddy, who until recently worked with children and teens at a pediatric obesity clinic.
In practice, that means taking a child's and their family's medical history, vital signs and labs, nutrition and physical activity habits, mental health and social circumstances into account, rather than checking only their body mass index (BMI) — an estimate of body fat calculated using weight and height.
That said, BMI still factors into a child's evaluation, although the measure has been widely criticized as an imprecise measure of fat and poor indicator of overall health. More-precise methods of measuring body fat are more cost- and time-intensive, and thus not regularly used in clinics or in research.
"Even though it's flawed, it's still a useful tool," Reddy said. "I sort of think of BMI as kind of the yellow traffic light" — a signal to slow down and see what else is going on with a child's health.
"The higher the percentile, the more likely it is that a child is carrying excess adiposity," meaning fat, said Dr. Sarah Hampl, chair of the AAP's Clinical Practice Guideline Subcommittee on Obesity and a lead author of the guidelines. "Overweight" is defined as a BMI at or above the 85th percentile and below the 95th percentile for children of the same age and sex, and "obesity" is defined as a BMI at or above the 95th percentile. These categories are reflected in the Centers for Disease Control and Prevention's new extended BMI growth charts for kids and teens.
"And yet it's still only one of several measures we look at in terms of determining the child's health," and whether or not their weight is negatively affecting them, Hampl said.
Related: High-sugar diet disrupts the gut microbiome, leading to obesity (in mice)
If a child is recommended for weight-loss treatment, what are their options?
One is a motivational interviewing, a type of counseling where doctors help kids and their families work towards adjusting their nutrition and physical activity. A similar but more extensive intervention, called intensive health behavior and lifestyle treatment (IHBLT), focuses on introducing similar lifestyle changes and making them sustainable in the long-term.
RELATED STORIES
"IHBLT is most often effective when it occurs face-to-face, engages the whole family, and delivers at least 26 hours of nutrition, physical activity, and behavior change lessons over 3 to 12 months," the guidelines state. Although backed by research, these types of programs aren't readily accessible to many kids, as few institutes host them and they're rarely covered by insurance, Reddy said.
As an adjunct to IHBLT, doctors may offer children with obesity weight-loss drugs, provided they are age 12 and older. These treatments include Wegovy (generic name semaglutide), a once-weekly injection that affects how the brain and gut communicate and reduces the user's appetite.
Weight-loss drugs approved for children have been tested in roughly year-long trials, but we don't yet have data on what happens after five or 10 years of use, for example, Hampl said. And there aren't set recommendations as to how long children should use the medications.
Teens ages 13 and older with severe obesity — meaning their BMI is equal to or greater than 120% of the 95th percentile for age and sex — may also be referred to a specialist to be evaluated for metabolic and bariatric surgery.
Evidence suggests that these surgeries can reduce teens' weight and counter health conditions linked to obesity, such as diabetes and high blood pressure. However, eating disorder experts have raised concerns that the procedures alter how and what patients can eat, which can damage their relationship to food, NPR reported; other experts worry that doctors will turn to surgery too quickly, without exhausting other options, according to STAT.
Others argue that surgery is just another option for patients and should be considered, if needed.
"There is too much hype or over emphasis on the mention that [pharmacotherapy] and surgery 'MAY or CAN' be offered," said Dr. Stephen Cook, an internist and associate professor who researches childhood and adolescent obesity at the University of Rochester Medical Center, told Live Science in an email. "There are a number of steps before those could be considered, and they are only to be considered for those with more severe levels of obesity," he said.

Nicoletta Lanese is the health channel editor at Live Science and was previously a news editor and staff writer at the site. She is a recipient of the 2026 AHCJ International Health Study Fellowship, with a project focused on antibiotic stewardship practices in Japan and the U.S. They hold a graduate certificate in science communication from UC Santa Cruz and degrees in neuroscience and dance from the University of Florida. Beyond Live Science, Lanese's work has appeared in The Scientist, Science News, the Mercury News, Mongabay and Stanford Medicine Magazine, among other outlets. Based in NYC, she also remains involved in dance and performs in local choreographers' work.

 Live Science Plus
Live Science Plus




