Prostate cancer: Causes, symptoms & treatment
Reference article: Facts about prostate cancer.


Prostate cancer occurs when the cells in the prostate gland grow uncontrollably, which can spread or cause complications due to an abnormally enlarged prostate. This type of cancer is the second most common form of cancer in men globally, according to the World Health Organization (WHO).
The prostate gland is a small, walnut-shaped gland that sits below the bladder and surrounds the urethra, the tube that carries urine out of the body. The gland is responsible for producing the nutrient-rich seminal fluid that houses and carries sperm. Prostate cancer doesn't occur in women because females don't have a prostate gland.
The prevalence of prostate cancer seems to be the highest in Australia, New Zealand, North America and western and northern Europe, primarily because the practice of getting tested for prostate cancer is far more common in those parts of the world than it is elsewhere, according to the WHO.
Prostate cancer is the fifth leading cause of cancer death in men globally and the second leading cause of cancer death in American men (after lung cancer), according to the American Cancer Society (ACS). But most men with prostate cancer won't die from it. In the U.S., the five-year relative survival rate for all stages after the cancer is first diagnosed is 98%, according to the latest ACS data.
What causes prostate cancer?
In general, cancers occur when abnormal cells start replicating and growing out of control rather than dying and becoming replaced by healthy cells. This can happen because of DNA defects that were either inherited or caused by environmental factors, such as smoking tobacco or being exposed to radiation. Scientists aren't exactly sure what causes prostate cancer, but the disease is closely associated with several risk factors.
The first one is age: 90% of prostate cancer cases are diagnosed in men age 56 or older, according to the National Cancer Institute (NCI). And the probability of being diagnosed with prostate cancer increases with age, with the highest probability being 1 in 12 for men 70 years or older.
Having a family history of prostate cancer is another major risk factor. The inherited risk of prostate cancer may be as high as 60%, according to the NCI. The prevalence of prostate cancer suggests that the risk of developing the disease is highest for black men, lowest for native Japanese men and intermediate for white men, but researchers haven't come to a consensus as to why.
Get the world’s most fascinating discoveries delivered straight to your inbox.
Hormone production also may play a role, as studies have shown that deficient or abnormal patterns of testosterone production seem to lower the risk of developing prostate cancer, according to the NCI.
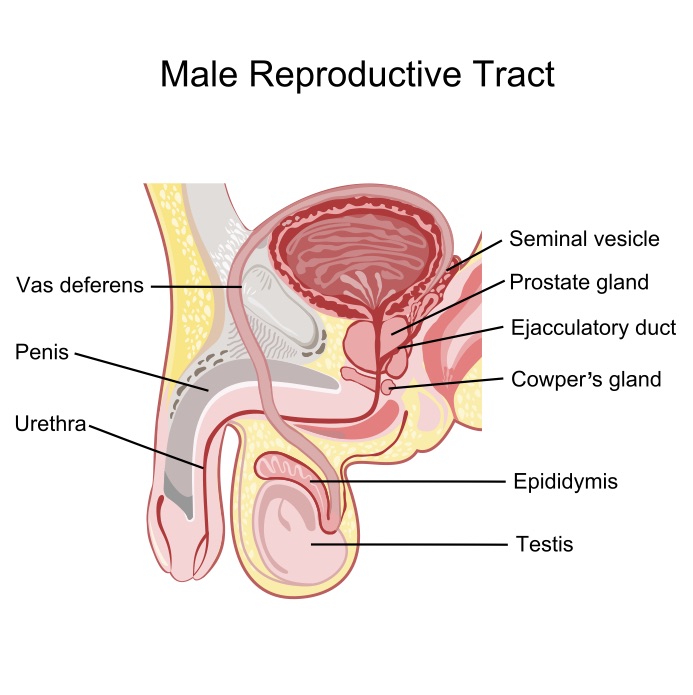
Diagram of the male reproductive system. The walnut-sized prostate gland sits right below the bladder and surrounds the urethra.
Symptoms and diagnosis
If prostate cancer is caught early enough, the patient may never experience symptoms. In more advanced stages, symptoms may include trouble urinating, blood in the urine or semen, erectile dysfunction or pain in the lower back, hips or thighs, according to the ACS. Those symptoms also may be caused by something other than prostate cancer, such as an enlarged-but-noncancerous prostate gland. Still, it's important to tell your doctor if you're experiencing any of those symptoms, as you may need to be screened for prostate cancer.
Most early cases of prostate cancer are caught after a prostate-specific antigen (PSA) blood test or a digital rectal exam, according to the ACS.
PSA is a protein produced by the prostate. Higher levels of PSA in the blood are correlated with an increased risk of prostate cancer, but there's no set cutoff that determines for sure whether a man has the disease.
The doctor also may perform a digital rectal exam, during which the doctor feels for any bumps or hard areas on the prostate that would indicate cancer growth. This can help the doctor figure out where the cancer is on the prostate and if it's likely to spread.
Depending on the results of these tests, your doctor may decide further testing (such as a biopsy or a CT scan) is warranted to confirm the presence of prostate cancer.
Age, overall health and family history are all important factors to consider when deciding whether to get screened for prostate cancer. The American Cancer Society recommends that men discuss the decision with their doctors to ensure they understand the uncertainties and potential risks involved.
Treatment
The treatment plan for prostate cancer depends on several factors and can vary widely, according to the Mayo Clinic.
For patients with low-risk, or slow-growing prostate cancer that's not causing symptoms, treatment may not be necessary; instead, the doctor may recommend regular testing to keep an eye on it. This may also be the treatment plan for very old patients or patients with other serious health conditions that could make cancer treatment difficult.
Surgical removal of the prostate gland is also an option, but this may cause urinary incontinence and erectile dysfunction. Radiation therapy to kill the cancer cells carries the same risks.
Related: Facts about prostate cancer (infographic)
Prostate cancer cells require testosterone to grow, so hormone therapy to stop the production of testosterone can help slow or eliminate cancer cell growth. The potential side effects of this treatment include erectile dysfunction, hot flashes, loss of bone mass, reduced sex drive and weight gain.
Chemotherapy, which uses drugs to rapidly kill cancer cells, may be an option for treating prostate cancers that don't respond to other forms of therapy.
Immunotherapy, or biological therapy, also may be used to treat difficult cases of prostate cancer. In this type of treatment, doctors extract the patient's immune system cells, modify them to specifically fight prostate cancer and then inject the modified cells back into the patient's body. According to the Mayo Clinic, immunotherapy is effective for some patients, but it's very expensive and requires multiple rounds.
Can you prevent prostate cancer?
There's no sure way to prevent prostate cancer, but as with most diseases, maintaining a healthy lifestyle is the best way to lower the risk of getting it, according to the ACS.
Certain drugs may lower a person's risk of developing prostate cancer. A class of drugs called 5-alpha reductase inhibitors prevent testosterone from turning into dihydrotestosterone, which is the main hormone that causes the prostate to grow. These drugs are prescribed to treat noncancerous prostate growth, but research suggests they also may lower prostate cancer risk. For example, one of these drugs, called finasteride, reduced the risk of prostate cancer by 25% in a large, long-term clinical trial published in The New England Journal of Medicine in 2019. These drugs aren't approved by the FDA specifically to prevent prostate cancer, but doctors can still prescribe them for this use.
There's a bit of evidence to suggest a daily dose of Aspirin might reduce prostate cancer risk, but the side effects of such a regimen likely outweigh the potential benefits, according to the Mayo Clinic.
Additional resources:
- Here are some good questions to ask your doctor about prostate cancer, from the American Cancer Society.
- Read more about drugs that may lower the risk of prostate cancer, from the National Cancer Institute.
- Learn more about the potential causes of prostate cancer, from the Prostate Cancer Foundation.

Kimberly has a bachelor's degree in marine biology from Texas A&M University, a master's degree in biology from Southeastern Louisiana University and a graduate certificate in science communication from the University of California, Santa Cruz. She is a former reference editor for Live Science and Space.com. Her work has appeared in Inside Science, News from Science, the San Jose Mercury and others. Her favorite stories include those about animals and obscurities. A Texas native, Kim now lives in a California redwood forest.

 Live Science Plus
Live Science Plus




