Does gut health affect skin?
Here's what we know so far about the link between gut health and skin health.


At a glance, our skin and our digestive system may seem like two separate entities. However, the evidence is growing that there's a connection between the two, often referred to as the "gut-skin axis." In fact, some scientists suggest that an imbalanced gut microbiome, or community of microbes in the digestive tract, could be linked to skin disorders such as psoriasis and eczema.
"We are really entering a new era in medicine as we begin to decipher the relationship between gut health and disease," said Dr. Brooke Jeffy, a fellow of the American Academy of Dermatology. "In dermatology, it has become more and more clear that there is a relationship between certain conditions and foods. But this is a fairly new idea. Just 10 years ago, we were taught that any relationship between food and dermatologic conditions was minimal at best. I believe we will see a shift in the approach to treating chronic inflammatory skin conditions, with a focus on gut health over the next few years."
So how exactly does gut health affect the skin? Here's what science tells us so far about the so-called gut-skin axis.
Article continues belowWhat is the gut-skin connection?
According to a 2021 review published in the journal Clinics in Dermatology, the gut-skin axis refers to the constant exchange of signals between the skin and the gut. It is often viewed as an integral part of a much bigger network, known as the gut-brain-skin axis, which is regulated by a host of signaling molecules and the activity of our gut microbes.
"When your gut microbiome is out of balance, the cells of the gut do not work properly which allows pro-inflammatory molecules to escape and enter the bloodstream," Jeffy told Live Science. "These molecules get to the skin where they trigger inflammation that causes accelerated aging or flares of rosacea, acne, eczema and psoriasis."

Jeffy received her undergraduate degree in biology from the University of Kentucky in Lexington, Kentucky, and her medical degree from the University of Louisville in Louisville, Kentucky. She completed her residency training at the University of Louisville. There, she completed two years of training in pathology and a preliminary year in internal medicine before starting her training in dermatology. Jeffy is board certified by the American Board of Dermatology and a fellow of the American Academy of Dermatology.
Dysbiosis, or "gut imbalance" is when your gut doesn't have enough "good" bacteria to thrive, and instead has higher levels of "bad" bacteria that can trigger things like inflammation. All humans have a unique microbiome, so this imbalance can look different for each of us.
According to Dr. Patricia Farris, dermatologist and clinical assistant professor at Tulane University School of Medicine, Louisiana, other mechanisms may also be at play.
Get the world’s most fascinating discoveries delivered straight to your inbox.
"When there is a bacterial imbalance in the gut, certain immune cells are activated, setting up a pattern of chronic systemic inflammation that can affect all organs, including the skin," she said. "There is an endocrine component in the gut-skin axis. Certain gut bacteria can produce neurotransmitters" — or chemical messengers — "that can trigger an itch-scratch cycle seen in some skin disorders."

Farris is a clinical assistant professor at Tulane University School of Medicine and in private practice in Metairie, Louisiana. In addition to being a fellow of the American Academy of Dermatology, she is also a member of the American Society of Dermatologic Surgery, American Society for Laser Medicine and Surgery, Women’s Dermatologic Society, International Society for Cosmetic Dermatology and the American Dermatologic Association.
Some studies also indicate that the gut-skin axis may be a casual factor in food allergies, allergic rhinitis and asthma, as described in a 2021 review in the journal Current Opinion in Gastroenterology. And in a 2022 review published in the International Journal of Molecular Sciences, researchers note that skin bacteria is important for helping wounds to heal fully, as well as preventing diabetic foot ulcers.
Gut health and skin disorders
Psoriasis
Psoriasis is an autoimmune disorder that causes people to develop patches of itchy, inflamed skin primarily on the knees and elbows, although it can also affect other areas of the body. This condition is not fully understood, but it is believed to be caused by a combination of an overactive immune system, genetic predispositions and environmental factors.
It also appears to be linked to gut health. According to a 2021 review in the International Journal of Molecular Sciences, changes in the gut microbiome in psoriasis are similar to those observed in patients with inflammatory bowel disease. In both of these conditions, there tends to be a significant increase in harmful bacteria strains like Salmonella and Campylobacter, while the "good" strains are in decline compared with people without the diseases.
"Patients with psoriasis lack certain bacteria that produce short chain fatty acids, resulting in immune imbalance and inflammation," Farris told Live Science. Short chain fatty acids are produced by the "'good"' bacteria in your gut, and are thought to play a role in health and disease.
The gut-brain-skin axis may also help to explain why psoriasis flare-ups tend to be strongly linked to stress and depression. A 2021 review published in the journal Biomedicine & Pharmacotherapy suggests that negative emotional states may lead to changes in gut microbiota, which in turn can trigger skin inflammation. The specific mechanism of this interaction is still unclear, but since psoriasis itself can be distressing, this could further exacerbate symptoms, the authors suggested.
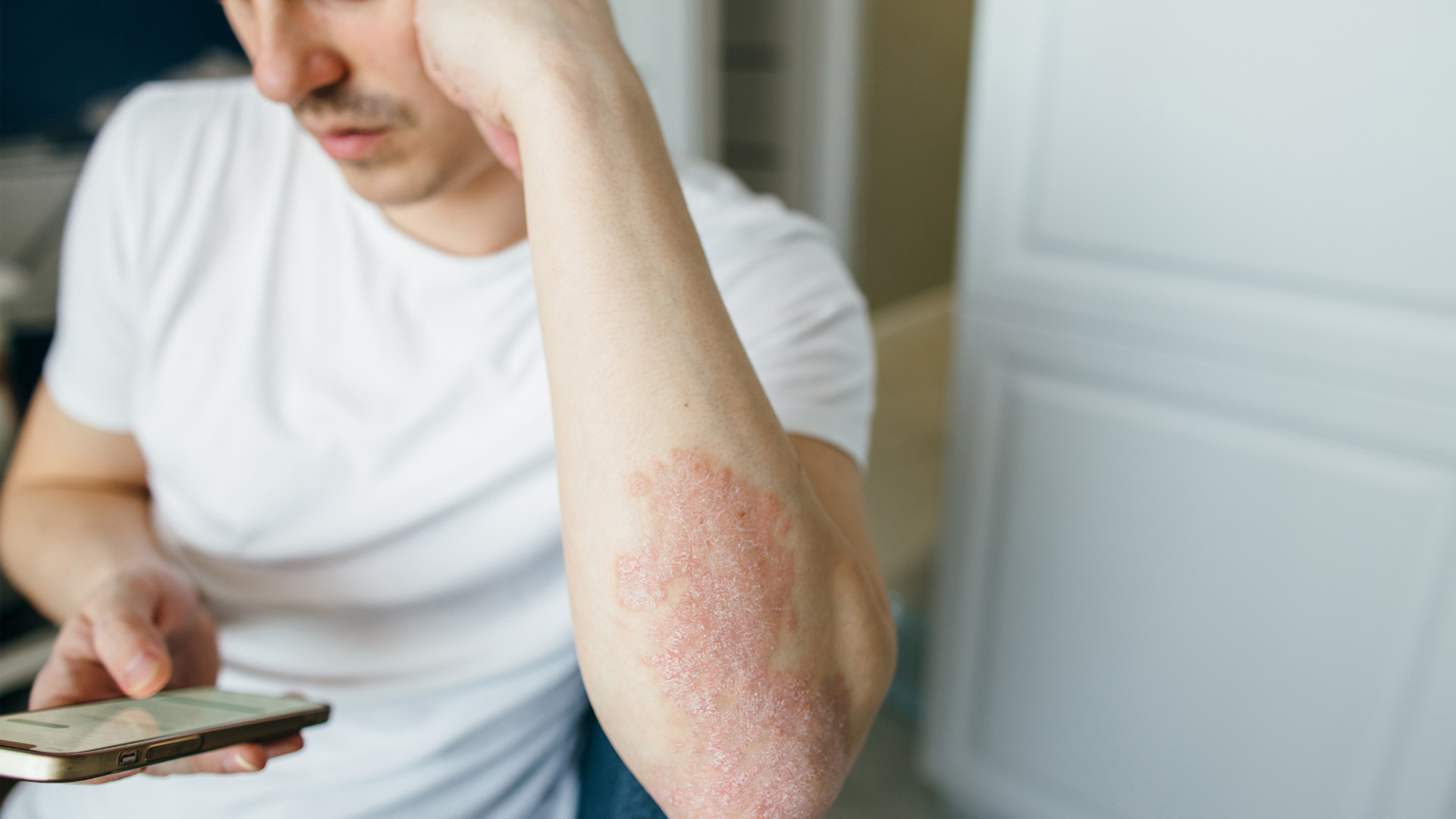
Eczema
Atopic dermatitis, also known as eczema, is an inflammatory condition that causes reddening, swelling, thickening and scaling of the skin. Its exact cause isn't known, but researchers believe it might be triggered by a host of environmental, genetic and psychological factors. Gut health also appears to be linked to the condition.
"It appears that patients with atopic dermatitis have a decreased gut bacterial diversity and lack certain bacteria found in healthy individuals," said Farris.
Indeed, a 2016 review published in the International Journal of Molecular Sciences identified particular environmental factors that may influence the composition of gut bacteria, and therefore the host's susceptibility to infections and allergies such as eczema. Those with altered gut microbiome compositions included infants born prematurely or via Cesarean section, those that had been breastfed for under six months, and those without older siblings. According to the authors, reduced contact with the maternal vaginal, perineal and fecal flora due to birth via C-section could result in lower counts of certain bacteria in these individuals. In the instance of breast feeding, the authors noted that breastfeeding with a duration of six months or longer increased the prevalence of colonization by lactobacilli and bifidobacteria.
However, the authors also noted that it is impossible to ascertain the cause and effect relationships of these factors, nor the strength of the association.

Rosacea
Rosacea is a chronic condition characterized by recurrent periods of redness and pimples around the face. Many different environmental and genetic factors trigger flare-ups of this disease, with gut health appearing to have a particularly significant role.
According to a 2021 review in the Advances in Therapy journal, rosacea has been linked to a number of gastrointestinal conditions, including inflammatory bowel disease, celiac disease and irritable bowel syndrome.
"Patients with rosacea have a greater chance of having something called small intestinal bowel overgrowth," said Farris. "In this condition there is an overgrowth of certain bacteria known as Helicobacter pylori that can contribute to the symptoms of rosacea including flushing and inflammation."
According to a 2018 study in the journal BMC Infectious Diseases, this specific bacteria can stimulate the immune system to produce a large number of inflammatory mediators, leading to the occurrence and aggravation of rosacea inflammation.
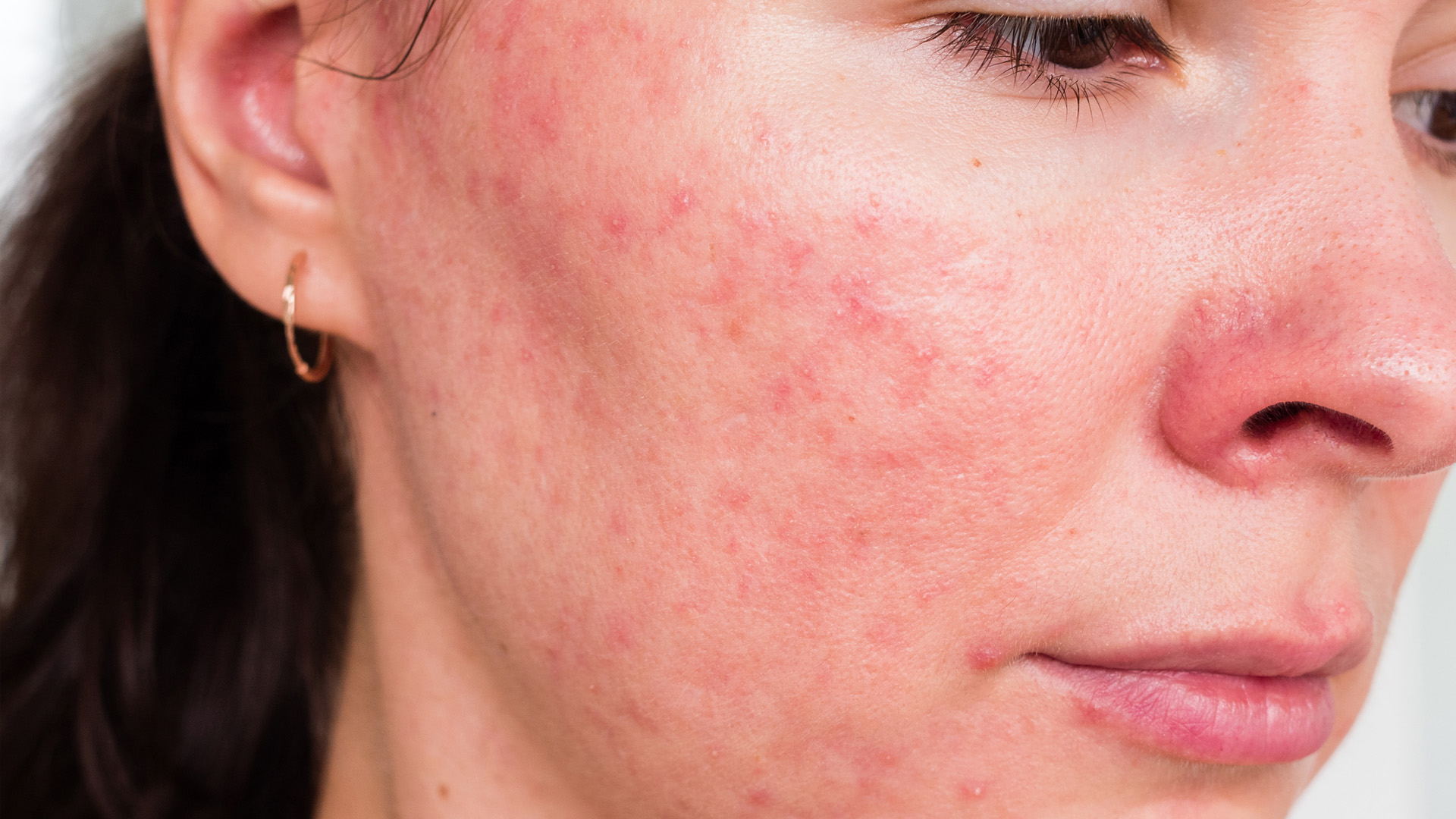
Acne
Acne is a common skin condition that manifests itself as blackheads, whiteheads, red bumps and cysts, mostly around the face. Genetic predispositions, hormonal imbalances and metabolic problems are considered to be common triggers. Recently, the evidence is growing that gut health may also be a significant factor.
"In acne, we know that a Western diet contributes to the pathogenesis of acne and causes gut dysbiosis," said Farris. A "Western diet" is categorized as being high in refined carbohydrates, saturated fats and added sugar.
A 2022 review in the journal Microorganisms also suggests that gut microbes may aggravate symptoms of acne by modifying skin immune responses to bacteria like Cutibacterium acnes and Propionibacterium acnes. However, more research is needed to understand this relationship.
This article is for informational purposes only and is not meant to offer medical advice.

Anna Gora is a health writer at Live Science, having previously worked across Coach, Fit&Well, T3, TechRadar and Tom's Guide. She is a certified personal trainer, nutritionist and health coach with nearly 10 years of professional experience. Anna holds a Bachelor's degree in Nutrition from the Warsaw University of Life Sciences, a Master’s degree in Nutrition, Physical Activity & Public Health from the University of Bristol, as well as various health coaching certificates. She is passionate about empowering people to live a healthy lifestyle and promoting the benefits of a plant-based diet.