Cavities (Tooth Decay): Causes, Symptoms & Treatment
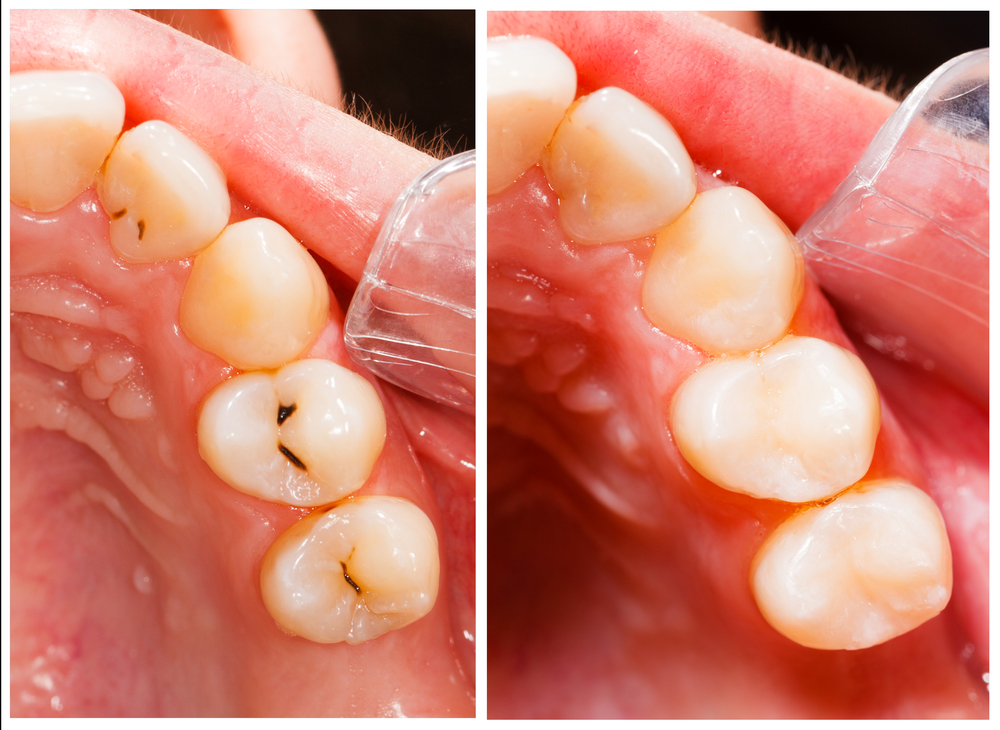
Cavities, also referred to as tooth decay or caries, are holes in the teeth. Cavities are the second-most common health disorder in the United States, according to the National Institutes of Health (the first is the common cold) and a very common disorder worldwide.
Cavities usually occur in the teeth of children and young adults, but they can happen at any age. Cavities are a common cause of tooth loss in young people. According to Dr. Margaret Culotta-Norton, a dentist in Washington, D.C., and former president of the D.C. Dental Society, cavities are the most chronic childhood disease in the United States.
Some groups have a higher risk for cavities, Culotta-Norton told Live Science, including:
- Lower-income families (children and adults).
- Senior citizens of all socio-economic status.
- People living in areas where the drinking water in not fluoridated.
- People with diseases and/or medication use that causes a decrease in salivary flow.
- People undergoing radiation therapy.
- People with diabetes.
- Tobacco users — both smoking and chewing.
- Alcohol and drug users.
- People who consume large amounts of carbonated and sugar drinks.
Causes
Cavities are the result of two primary factors: bacteria in the mouth and a high-sugar and starch diet. It is natural to have bacteria in the mouth but it becomes problematic in the case of poor oral hygiene.
According to the National Institutes of Health, the mouth's normal bacteria combine with food pieces and saliva to form plaque. Plaque is a sticky, invisible substance that accumulates quickly. Foods rich in sugar or starch make plaque stickier. If plaque stays on the teeth for more than a few days, it gets harder and becomes a substance called tartar.
Cavities form when bacteria in plaque and tartar convert sugar into acid. According to Culotta-Norton, Streptococcus mutans and Streptococcus sobrinus are bacteria especially likely to combine with fermentable carbohydrates like sucrose, fructose and glucose and produce acid. “The acid demineralizes the hard structure of the tooth, which over time creates a soft spot, or hole in the tooth called a cavity,” Culotta-Norton said.
The destruction doesn't stop there, reports the Mayo Clinic. After the enamel is worn away, the acid reaches the next layer of the teeth. This layer, called dentin, is softer and susceptible to acid. The bacteria and acid continue to work their way through the tooth, into the pulp, creating a bigger and bigger hole.
According to the NIH, cavities are most commonly found where plaque is highly prevalent, such as on the molars, between teeth, near the gum line, and at the edges of fillings.
Symptoms
There are often no symptoms of cavities, which is why Culotta-Norton stressed the importance of visiting a dentist and having “radiographs taken periodically so that cavities can be diagnosed and treated early before they get large enough to cause symptoms.” She reported that the most common early symptoms of cavities are a "chalky white or discolored spot on a tooth" and "sensitivity to cold."
"As the cavity progresses, the decay gets near the nerve (pulp) and can cause pain, which gets progressively worse especially with exposure to heat, cold, sweet foods or drinks," she continued. “If the decay gets large enough, part of the tooth may fracture off, leaving a large visible hole, and the tooth may be sensitive to biting pressure. Bad breath and or a bad taste in the mouth are also symptoms."
Cavities on the front teeth are the easiest to see and will look like a brown or black spot. Cavities in other parts of the mouth are often not visible without an X-ray.
Related: Tooth sensitivity: Causes and remedies
Prevention
Just as there are two factors that cause cavities, there are two main factors to preventing them: oral hygiene and diet change.
Good oral hygiene includes brushing your teeth at least twice a day, having a professional teeth-cleaning every six months, and having X-rays and a dental exam annually to detect cavity development. Flossing is also a typical recommendation, but in 2016 the Department of Health and Human Services dropped their recommendation to floss daily, or at all, from their Dietary Guidelines for Americans. Additionally, the benefits of flossing have not been proven, though many dentists still recommend the practice.
Reducing the amount of sugar — especially sugary drinks and juices — can help prevent cavities. You may consider brushing your teeth or rinsing your mouth after eating sticky foods. The NIH also suggests incorporating sugary, chewy foods such as dried fruit and candy into a meal rather than eating them as a snack. Minimizing snacking, avoiding constant sipping of sugary drinks, and not sucking on candy or mints can all help, too, because they produce a constant supply of acid in the mouth.
The Mayo Clinic suggests looking into dental sealants. Dental sealants may help prevent cavities and are most frequently applied to the teeth of children after their molars come in. Sealants are thin, plastic-like coatings on the surface of the molars that prevent the accumulation of plaque.
Fluoride is another cavity-prevention strategy encouraged by the Mayo Clinic. It can be consumed in drinking water or as a supplement. Topical fluoride is frequently applied as part of routine dentist visits. Your dentist may also recommend a fluoride toothpaste or mouthwash. When it comes to children, toothpastes containing fluoride should be closely monitored, though. Too much fluoride can cause deformed, yellowed teeth.
Get the world’s most fascinating discoveries delivered straight to your inbox.
Jessie Szalay is a contributing writer to FSR Magazine. Prior to writing for Live Science, she was an editor at Living Social. She holds an MFA in nonfiction writing from George Mason University and a bachelor's degree in sociology from Kenyon College.
