Hemophilia: Causes, symptoms & treatment
Reference article: Facts about hemophilia.
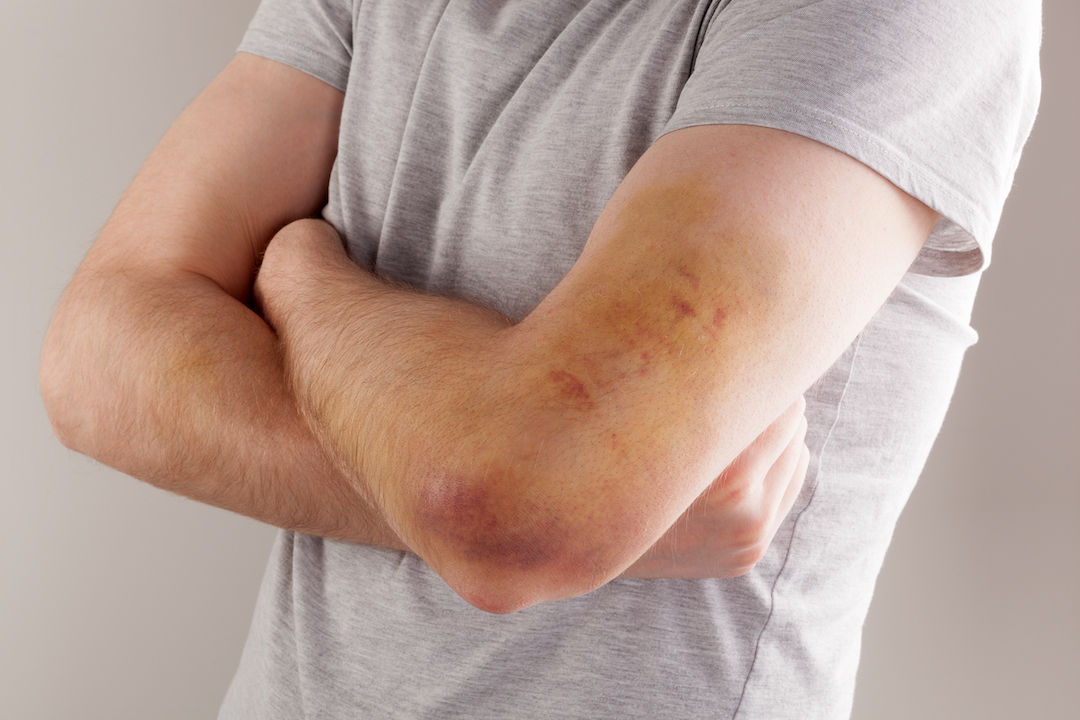
Hemophilia is a rare bleeding disorder that prevents the blood from clotting properly. People with hemophilia either lack or have very low amounts of a specific clotting factor: a protein that promotes blood clotting and controls bleeding.
As a result, the blood can't clot as efficiently, and a person may bleed for a longer period of time after a relatively small trigger, such as bumping an elbow, said Dr. Stacy Croteau, medical director of the Boston Hemophilia Center at Dana-Farber/Boston Children's Cancer and Blood Disorders Center.
Hemophilia is a relatively rare condition affecting an estimated 20,000 people in the United States, according to the Centers for Disease Control and Prevention (CDC). The blood disorder is a sex-linked disease that primarily affects males. The CDC estimates that hemophilia occurs in about 1 out of every 5,000 male births.
How hemophilia is inherited
Hemophilia is caused by a mutation in one of the genes that make a specific clotting factor protein needed to form a blood clot. There are three types of hemophilia.
Hemophilia A is the most common type, and it occurs when clotting factor VIII is low or missing in the blood. The second most common type is hemophilia B, also known as Christmas disease, named for Stephen Christmas, who at 5 years old was the first patient diagnosed with the disease, according to the National Organization of Rare Disorders (NORD). Hemophilia B is caused by the absence or low levels of clotting factor IX. Hemophilia C, which is even rarer, is caused by missing clotting factor XI. This type affects males and females equally because it is not sex-linked, but both parents must carry the mutated gene for a child to be affected by the disorder.
Related: Mom with rare blood disorder adopts 3 kids with same condition
There are over a dozen different clotting factors in the blood, according to the Merck Manual. In general, the term hemophilia refers only to deficiencies in one of the three clotting factors mentioned above. Deficiencies in one or more of the remaining clotting factors are even rarer and are typically referred to as factor deficiencies.
Get the world’s most fascinating discoveries delivered straight to your inbox.
Hemophilia is usually inherited, but in about 30% of cases, there is no family history of hemophilia. In those cases, the disorder might be caused by a new or previously unnoticed genetic mutation.
The faulty genes for hemophilia A and B are found on the X chromosome, according to the Indiana Hemophilia and Thrombosis Center. Females who are carriers of hemophilia have one X chromosome with the altered gene that causes hemophilia and one X chromosome with a properly functioning gene.
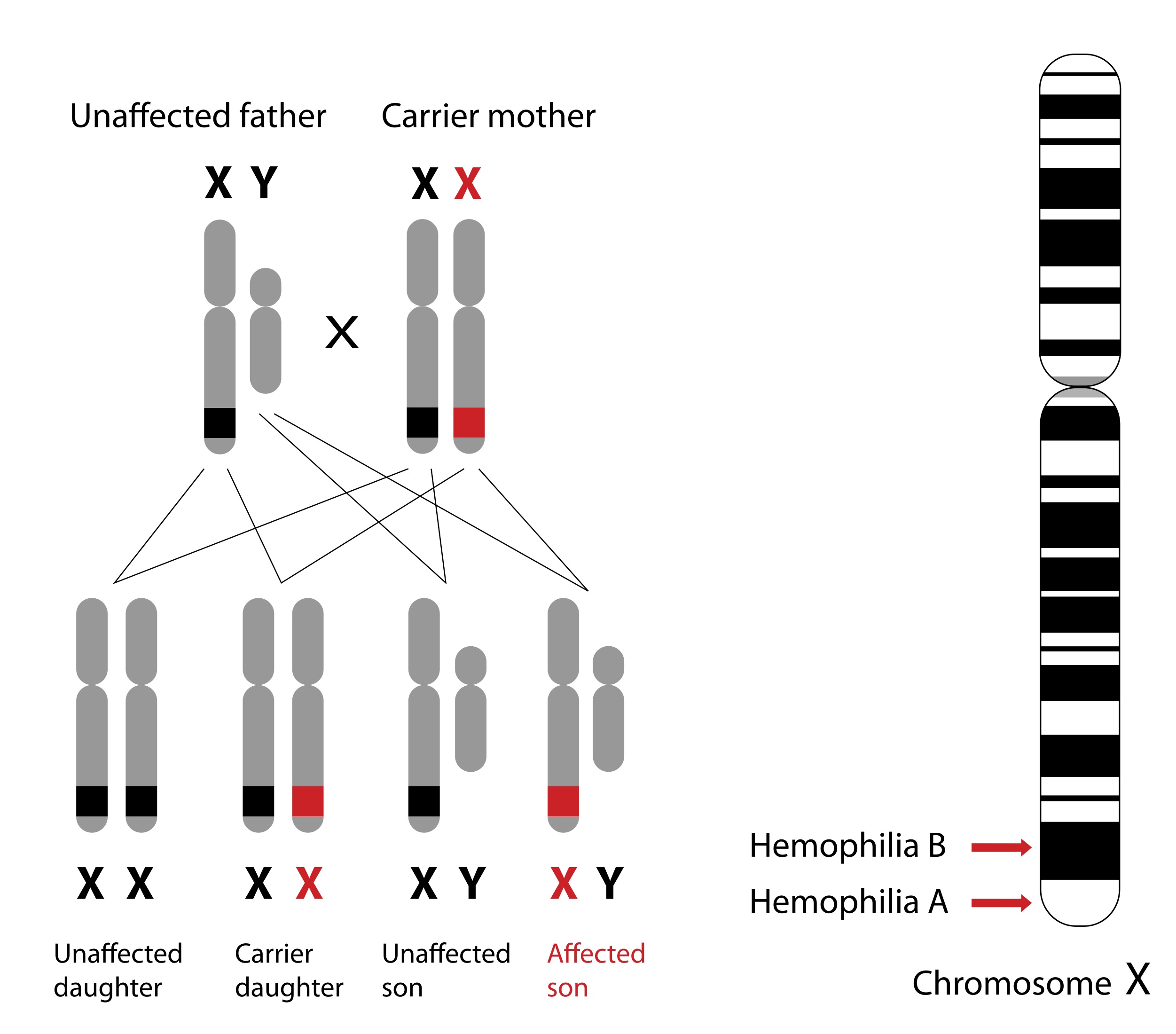
Diagram of the genetics behind hemophilia A and B inheritance.
Males have only one X chromosome and one Y chromosome, so if they inherit a copy of the faulty X chromosome that carries hemophilia from their mother, they will develop the disorder. Males who inherit their mother's properly functioning X chromosome will not have hemophilia.
Females have two X chromosomes, so if a daughter inherits one X chromosome containing the faulty hemophilia gene from her mother and one normal X chromosome without the faulty gene from her father, she will become a carrier of hemophilia and may pass on the faulty gene to her own children some day.
A father who has hemophilia can only pass on his altered hemophilia gene to his daughter because only a daughter will inherit his altered X chromosome. (His son will inherit his unaffected Y chromosome.)
Hemophilia predominantly affects males because they inherit only one X chromosome, and therefore, have only one gene responsible for coding the necessary clotting factors. Daughters inherit two X chromosomes, so if they have one X chromosome with the faulty hemophilia gene and one without the faulty gene, the normal gene can compensate for the defective one, which usually prevents females from getting the bleeding disorder, according to the CDC.
Most women who are carriers of hemophilia don't experience any signs or symptoms of the blood disorder, according to the Mayo Clinic. And women who do experience symptoms tend to have mild hemophilia. In this case, both X chromosomes have the faulty gene or one X chromosome has the hemophilia gene and the other gene is missing or can't produce enough clotting factor. These women may experience symptoms such as heavy periods, prolonged bleeding after dental procedures or heavy bleeding after childbirth.

Frequent nosebleeds is a common symptom of hemophilia.
Hemophilia symptoms
"One of the misperceptions about hemophilia is that a person with the disorder will have a big pool of blood with a small cut or minor injury," Croteau told Live Science. But a bigger health concern, especially for people with moderate to severe types of hemophilia, is internal bleeding into muscles, joints and soft tissue, she said.
If someone with hemophilia fell down and got a cut, that person may require more medication or more applied pressure to stop the external bleeding, she said.
But the signs of internal bleeding may be harder to spot, especially when it comes to babies and kids who don't have the words yet to describe their discomfort, Croteau said. In these situations, a parent might notice behavior changes, such as a child seeming fussier than usual, or a child showing pain by avoiding putting weight on a limb or not bending an elbow.
Another sign of internal bleeding is swelling or redness on the child's skin, and the area may feel warm, Croteau said. As children get older and can express pain, they may say they feel a "bubbling" or "popping" sensation in their joints before they can actually notice any redness or discomfort in these areas, she said.
The concern with repeated episodes of deep internal bleeding is that it can seriously damage a person's joints, muscles, brain or other internal organs, and may be life-threatening, according to the National Institutes of Health.
Adults with hemophilia experience the same symptoms as children with the blood disorder. According to the CDC, some common signs and symptoms of hemophilia A and B may include:
- Bleeding into the skin, forming large bruises caused by a buildup of blood under the skin.
- Bleeding into muscles and joints. Internal bleeding may result in swelling, pain or tightness in the knees, elbows and ankles that can lead to arthritis and limited movement.
- Excessive bleeding of the mouth and gums after removing a tooth or dental surgery.
- Excessive bleeding after circumcision. Hemophilia may be detected early in life if bleeding goes on for a long time after male babies have their foreskin removed.
- Excessive bleeding after having shots or vaccinations.
- Blood in the urine or stool.
- Frequent and hard-to-stop nosebleeds.
A person can have mild, moderate or severe hemophilia, based on how much clotting factor is in the blood. Someone with hemophilia typically stays at the same severity level throughout life, Croteau said.
About 60% of people with hemophilia A have severe hemophilia, about 15% have moderate hemophilia and about 25% have the mild form, according to the National Hemophilia Foundation.
The severity of hemophilia is described as follows, according to the World Federation of Hemophilia:
- Severe hemophilia: People usually bleed frequently, about once or twice a week, into their muscles or joints. Bleeding is often "spontaneous," meaning it happens suddenly, for no obvious reason.
- Moderate hemophilia: People bleed less frequently, about once a month, and rarely have spontaneous bleeding. They may bleed for a long time after surgery, a bad injury or dental procedure.
- Mild hemophilia:. People do not bleed often, but when they do, it's a result of surgery or major injury.
Regardless of severity, people with hemophilia can expect to have a normal life span with proper therapy, according to a report on hemophilia and aging from the National Hemophilia Foundation.
How hemophilia is diagnosed
"If there is a family history of hemophilia, an infant can be tested for it shortly after birth or during the first year of life," Croteau said. But since 1 in 3 people who have the disease have no family history, severe hemophilia is usually picked up during the first year or two of life, after a child has an episode of abnormal bleeding that a parent notices, she said.
A person with mild hemophilia who has no family history might not be diagnosed until school age, the teen years or even adulthood, Croteau said. Mild cases may turn up later because a person may not show signs of excessive bleeding until he or she has surgery or a significant injury, she explained.
Blood test results are used to diagnose hemophilia and determine its type and severity. Tests can measure how long it takes blood to clot and whether blood is clotting properly. Tests can also show whether levels of certain clotting factors are low or missing, which can determine the type and severity of the bleeding disorder. Genetic testing can indicate if particular genes may be causing hemophilia.
Hemophilia is usually diagnosed at a young age, once a child experiences an episode two of excessive bleeding.
How is hemophilia treated?
For people with severe and moderate hemophilia A or B, factor replacement therapy may be given intravenously to replace the missing clotting factor (VIII or IX) so blood can clot properly and to avoid joint damage from internal bleeding, Croteau said.
Replacement clotting factor can be given to control a bleeding episode in progress, and treatment can also be given on a regular schedule to help prevent bleeding episodes from occurring.
People with hemophilia A may need to replace clotting factor about two or three times a week, while those with hemophilia B may need treatment twice a week, once a week or every two weeks, Croteau said. Treatment often happens at home once patients or parents of patients are comfortable administering the therapy, she said.
Some people with severe hemophilia may experience a negative reaction to the replacement clotting factors used to treat the blood disorder. Their immune system develops inhibitors, which are proteins that inactivate the clotting factors and make treatment less effective. In these cases, other medications can be given to help blood clot.
People with severe and moderate hemophilia should avoid contact sports such as rugby, football, wrestling, ice hockey, boxing and lacrosse because of potential injuries and the risk of bleeding into the head, stomach and other tissues, Croteau said.
"It takes a lot of work to be healthy with hemophilia," and regularly replacing clotting factor can be a burden, Croteau said. But with regular therapy, people with hemophilia typically have a normal life expectancy, she said.
Additional resources:
- Find answers to frequently asked questions about hemophilia, from the World Federation of Hemophilia.
- Read more about how hemophilia is inherited, as explained by the CDC.
- Separate fact from fiction about hemophilia, from HemAware, the bleeding disorders magazine.
Cari Nierenberg has been writing about health and wellness topics for online news outlets and print publications for more than two decades. Her work has been published by Live Science, The Washington Post, WebMD, Scientific American, among others. She has a Bachelor of Science degree in nutrition from Cornell University and a Master of Science degree in Nutrition and Communication from Boston University.

 Live Science Plus
Live Science Plus




