How do fevers kill germs?
You may have heard that fevers help fight infections. But how, exactly, do they do it?


They're the hallmarks of cold and flu season: a sore throat, a blocked nose and, sometimes, a dreaded fever.
You may have heard that the warmth of a fever helps the body recover from illness. But how, exactly, do fevers help kill germs in the body?
Scientists know that elevated body temperatures play a role in helping the immune system fight infection: "The enhanced immune function during fever is at least partly caused directly by the fever because it can also be elicited by hyperthermia — that is, increased body temperature in the absence of an infection," Anders Blomqvist, a neuroscientist who studies fever at Linköping University in Sweden, told Live Science in an email.
But just cranking up the heat might not be enough to thwart an illness, so other immune factors must also be involved.
Fevers begin when immune cells at the site of an infection secrete pro-inflammatory cytokines — proteins that ramp up the immune response. To generate a fever, some cytokines travel to the brain and mess with the hypothalamus, which, among regulating other bodily functions, acts as the body's thermostat. There, the cytokines boost the production of enzymes that synthesize fever-triggering chemical signals called prostaglandins.
In fact, fever-suppressing drugs such as acetaminophen (Tylenol) and ibuprofen (Advil) are thought to work by blocking these enzymes from making prostaglandins.
Get the world’s most fascinating discoveries delivered straight to your inbox.
Prostaglandins initiate several changes in the body that trigger a fever, which is often defined as a body temperature of at least 100.4 degrees Fahrenheit (38 degrees Celsius). Acting through the chemical messengers of the nervous system, they boost heat generation within brown fat reserves, which burn sugar. They also induce muscle shivering to build heat, and they limit heat loss by constricting blood vessels, especially near the extremities, like the hands and feet.
But how does turning up the heat affect the scuffle between pathogens and the immune system?
"Febrile temperatures have been shown to increase the immune response by stimulating both the innate and adaptive compartments of the immune system," Blomqvist said. The former controls generalized immune reactions, while the latter "learns" to fight new pathogens as they enter the body. "But the underlying mechanisms are not fully understood," he noted.
However, there are specific elements of the immune system that fevers are thought to boost. First-responder immune cells called neutrophils are recruited to the front lines at an infected site; these cells die shortly after service, so fevers may encourage a larger number to be drafted to the battlefield.
There's also evidence that, during a fever, so-called dendritic cells develop a stronger tendency to engulf harmful microbes. By gobbling up germs, the cells can then present fragments of the microbes to adaptive immune cells, giving them intel on how to mount an attack tailored toward the invader.
Related: Can you catch a cold and the flu at the same time?
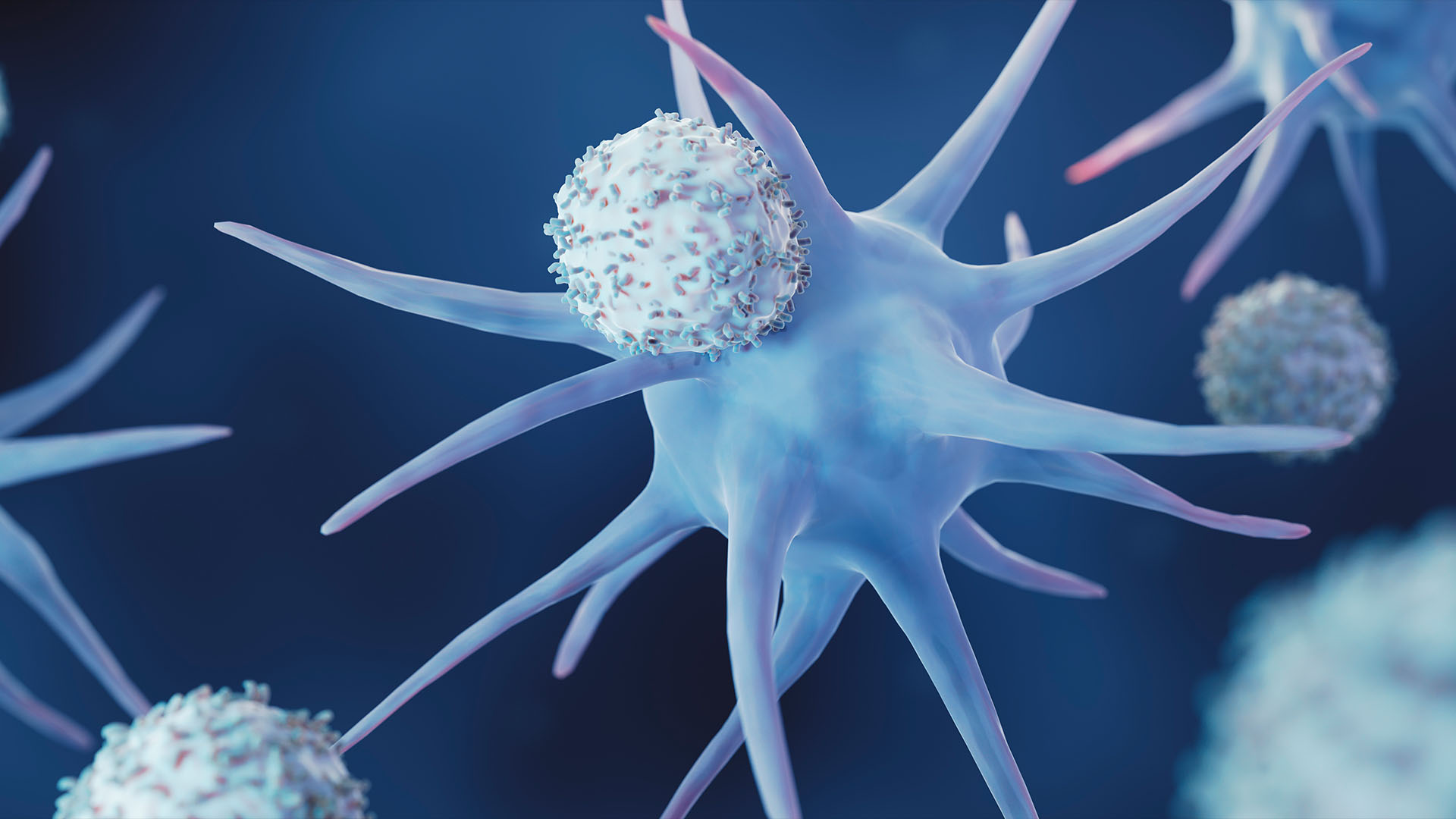
Dendritic cells (large cells) activate cells of the adaptive immune system (small cells) to fight specific germs.
Researchers have also proposed that fevers might hamper a pathogen's chances of winning the battle by putting it in the hot seat. If a foreign invader evolves to infect the body at normal temperatures, its performance may dwindle when overheated as its enzymes might start to "cook," losing shape and functionality. But, if the pathogen evolves to withstand fevers, it might then become less adept at infecting people at normal body temperatures. In essence, the pathogen might find itself in a catch-22 scenario.
Scientists face a major challenge in figuring out how fevers fight infection: The cytokines that trigger fevers also enhance other immune functions, so it's difficult to tease apart the effect of the fever from these other immune boosts. For example, pro-inflammatory cytokines promote the migration of immune cells around the body. This ushers them to the infected site as well as immune tissues, like lymph nodes, where adaptive immune cells are trained to fight an infection.
Although the cytokines also play their part, Blomqvist argued that fevers play an important role in fighting foreign invaders.
Studies show that intensive-care patients are more likely to recover from an infection if they develop a fever. The effect of fever-suppressing drugs is also telling: Doctors may feel it's necessary to administer them if they're worried a patient's fever will rise to dangerous temperatures, but in less severe cases, using these drugs might disarm the body's defenses.
RELATED STORIES
"The most robust evidence for the beneficial effects of fever comes from preclinical and clinical studies showing increased mortality to infections when antipyretics [fever reducers] are given," Blomqvist noted. Critically ill patients were more likely to survive if they only received fever-reducing acetaminophen at the last minute, before their fever crossed the danger threshold.
This article is for informational purposes only and is not meant to offer medical advice.
Ever wonder why some people build muscle more easily than others or why freckles come out in the sun? Send us your questions about how the human body works to community@livescience.com with the subject line "Health Desk Q," and you may see your question answered on the website!

Kamal Nahas is a freelance contributor based in Oxford, U.K. His work has appeared in New Scientist, Science and The Scientist, among other outlets, and he mainly covers research on evolution, health and technology. He holds a PhD in pathology from the University of Cambridge and a master's degree in immunology from the University of Oxford. He currently works as a microscopist at the Diamond Light Source, the U.K.'s synchrotron. When he's not writing, you can find him hunting for fossils on the Jurassic Coast.

 Live Science Plus
Live Science Plus




