How does the COVID-19 pandemic compare to the last pandemic?
There are some key differences between the 2009 swine flu and COVID-19, and the response to each of them.

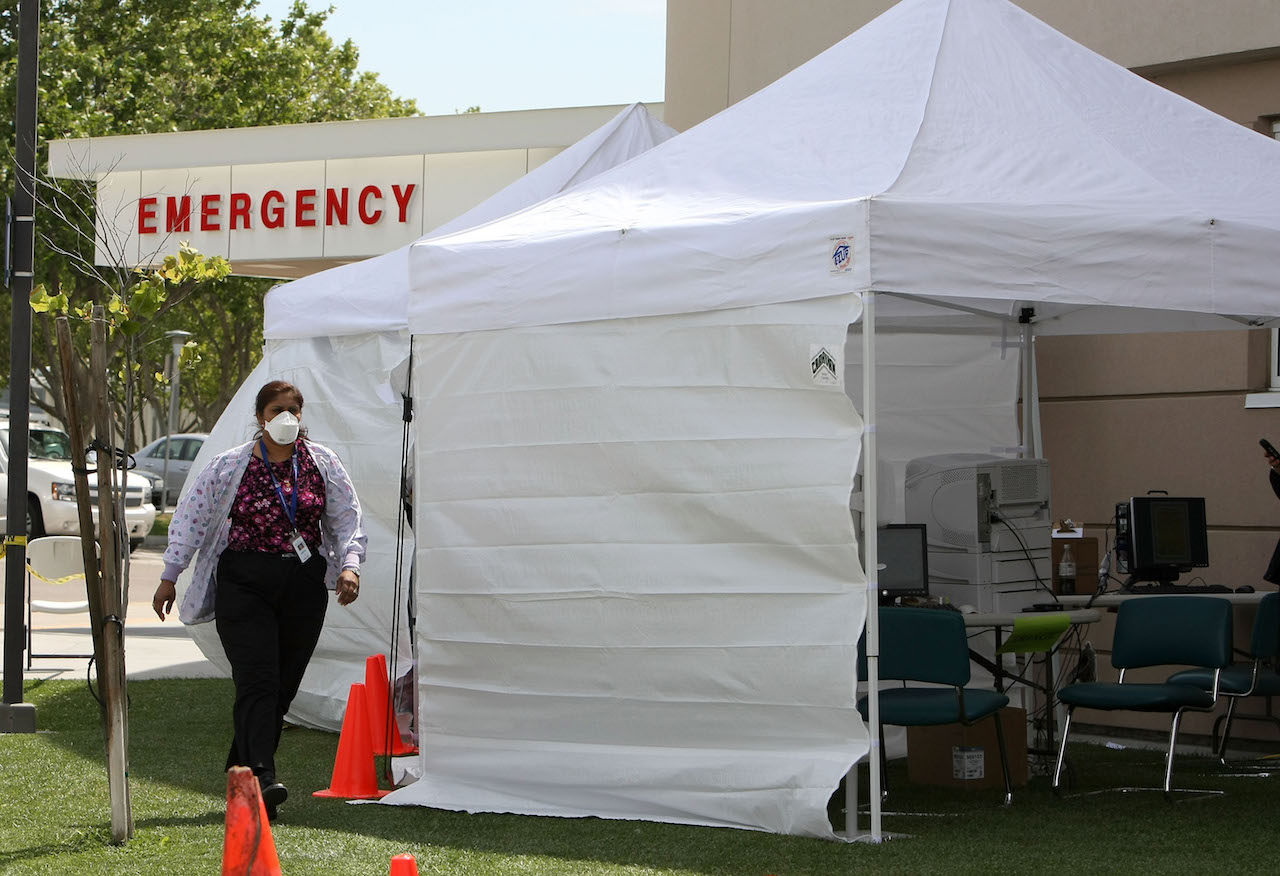
It's been a little over a decade since the world experienced its last pandemic, the 2009 H1N1 swine flu. Between the spring of 2009 and the spring of 2010, the virus infected as many as 1.4 billion people across the globe and killed between 151,700 and 575,400 people, according to the Centers for Disease Protection and Control. Now, the world is in the midst of the COVID-19 pandemic, caused by a novel coronavirus called SARS-CoV-2.
Having been through a pandemic in recent history, it seems reasonable to expect that government agencies in the U.S. would be prepared for the next one. But there are some key differences between the 2009 swine flu and COVID-19, and the response to each of them.
"The 2009 H1N1 pandemic should have been a warning sign," said Steffanie Strathdee, the Associate Dean of Global Health Sciences at the University of California San Diego's Department of Medicine. "It didn't end up being a pandemic that killed millions of people as we feared it would, but it should have been a wake-up call. By all serious estimates, COVID-19 is going to be a major killer."
Strathdee is also the author of "The Perfect Predator" (Hachette Books, 2019), a memoir of her personal experience fighting a deadly microbial pathogen, a superbug called Acinetobacter baumannii, and witnessing her husband almost die from it. Her husband fully recovered, but is at high risk of developing serious complications if the COVID-19 pandemic reaches him.
How are the illnesses different?
The 2009 flu pandemic was the second H1N1 pandemic the world had seen — the first being the 1918 Spanish flu, still the most deadly pandemic in history. The 2009 pandemic was caused by a new strain of H1N1 that originated in Mexico in the spring of 2009 before spreading to the rest of the world. By June of that year, there were enough cases that the World Health Organization declared the swine flu outbreak a pandemic.
In the U.S., between April 2009 and April 2010, the CDC estimates there were 60.8 million cases of swine flu, with over 274,000 hospitalizations and nearly 12,500 deaths — that's a mortality rate of about 0.02%.
Related: Path of a pandemic: Map shows how H1N1 swine flu spread
Get the world’s most fascinating discoveries delivered straight to your inbox.
Coronavirus science
The mortality rate for the novel coronavirus is much higher so far, around 2% (although the number will likely change as more people are tested). That may not sound like a big difference, "but when extrapolated, can mean millions more deaths," Strathdee said.
The 2009 flu pandemic primarily affected children and young adults, and 80% of the deaths were in people younger than 65, the CDC reported. That was unusual, considering that most strains of flu viruses, including those that cause seasonal flu, cause the highest percentage of deaths in people ages 65 and older. But in the case of the swine flu, older people seemed to have already built up enough immunity to the group of viruses that H1N1 belongs to, so weren't affected as much.
There is typically some herd immunity to seasonal flu, Strathdee said. This means that so many people are immune to the infection, because of vaccines or because their immune system has already fought the infection, that the few people who aren't immune are somewhat protected. There might be some groups of people who have immunity to the 2019-CoV-2 virus, too, but that's an area that's still being researched. So far, COVID-19 is most deadly for people over 60 who have underlying health conditions.
Another difference is that flu viruses are spread in respiratory droplets and airborne particles, while 2019-CoV-2 is primarily spread through respiratory droplets, and in some instances may be shed in feces, Strathdee said. "We don't yet know how important the oral-fecal route of infection is, but it's another reason to wash your hands regularly with soap and water," she said.
The symptoms of the swine flu were similar to those caused by other flu viruses, primarily: fever, cough, headache, body aches, sore throat, chills, fatigue and runny nose. Those symptoms show up between one and four days after contracting the virus.
Doctors are still determining the full breadth of symptoms of COVID-19. So far, the clearest signs of the disease appear to be fever, dry cough and shortness of breath, according to the CDC. Other symptoms, including headache, sore throat, abdominal pain and diarrhea, have been reported, but are less common. And just like the flu, COVID-19 can cause respiratory issues that lead to serious problems, such as pneumonia.
But some people with COVID-19 have mild symptoms, or they may not experience symptoms at all, according to the CDC. The virus appears to have an incubation period of between four and 14 days, which means an individual could be carrying (and spreading) the virus for up to two weeks before experiencing any illness.
The H1N1 flu was also less contagious than the novel coronavirus. The basic reproduction number, also called the R-nought value, is the expected number of individuals who can catch the virus from a single infected person. For the 2009 H1N1 virus, the mean R-nought value was 1.46, according to a review published in the journal BMC Infectious Diseases. For the novel coronavirus, the R-nought value is estimated to be between 2 and 2.5, at the moment.
How has the response been different?
There have been a few differences in the way the U.S. responded to the 2009 H1N1 pandemic compared with the nation's response to COVID-19 pandemic.
"A major difference in response is that we were better prepared for a pandemic (at least in the U.S.) years ago," Strathdee said.
At the beginning of both pandemics, the genetic sequences of the virus were released to the public with remarkable speed, so that countries could create diagnostic tests as soon as possible. On April 24, 2009, just nine days after initial detection of H1N1, the CDC uploaded genetic sequences of the virus to a public database and had already begun development of a vaccine. Similarly, on Jan. 12, 2020, five days after the novel coronavirus was isolated, Chinese scientists published the virus' genetic sequence.
The first case of COVID-19 in the U.S was identified on Jan. 20, and the country's Department of Health and Human Services declared COVID-19 a public health emergency 11 days later, on Jan. 31. Similarly, the U.S. declared the swine flu a public health emergency 11 days after the first confirmed U.S. case in 2009.
But that's about where the similarities stop. Things haven't happened quite as fast or as smoothly with COVID-19 as they did with H1N1.
Within four weeks of detecting H1N1 in 2009, the CDC had begun releasing health supplies from their stockpile that could prevent and treat influenza, and most states in the U.S. had labs capable of diagnosing H1N1 without verification by a CDC test.
But diagnostic testing ran into significant hiccups when it came to COVID-19. On Feb. 5, the CDC began sending diagnostic kits for 2019-CoV-2 to about 100 public-health laboratories across the country. Most of the labs received faulty kits, which caused a major delay in combating the virus. Testing had to continue exclusively at the CDC headquarters until the agency could develop and send out replacement kits. This meant that COVID-19 continued to spread, undetected for weeks.
The FDA commissioner announced on Feb. 29 that the agency would allow labs across the country to begin testing for the novel coronavirus with their own lab-developed tests without prior approval, as long as the labs took basic steps to validate the tests and submitted an "emergency use authorization" (EUA) application within 15 days of the notice.
Related: Confusion and chaos surround coronavirus testing in the US
By March 10, seven weeks after the first confirmed case in the U.S., the CDC announced that 79 state and local health labs in the United States could test people for COVID-19. But some of those labs are already running out of supplies to run the tests.
"Another difference is that this is the first pandemic in the era of social media," Strathdee said. The wealth of misinformation about the disease has spread faster than the virus, she said, as has blame for the virus. "We need to stop thinking like this. We need to unite against the virus."
However, the plus side of living in this advanced technological age is the speed at which research and vaccine development can occur. A potential treatment and the first trial of a candidate vaccine are already underway, which is amazing and encouraging, Strathdee said. "It will take time for a vaccine and treatments to be studied and scaled up," she said. "So in the meantime, we all need to do our part and stay home."
- Going viral: 6 new findings about viruses
- Top 10 mysterious diseases
- The 12 deadliest viruses on Earth
Editor's note: This article was updated on March 25, 2020 to reflect a correction. The U.S. declared the swine flu a public health emergency 11 days after the first confirmed U.S. case in 2009, not two days.
Originally published on Live Science.
OFFER: Save at least 53% with our latest magazine deal!
With impressive cutaway illustrations that show how things function, and mindblowing photography of the world’s most inspiring spectacles, How It Works represents the pinnacle of engaging, factual fun for a mainstream audience keen to keep up with the latest tech and the most impressive phenomena on the planet and beyond. Written and presented in a style that makes even the most complex subjects interesting and easy to understand, How It Works is enjoyed by readers of all ages.

Kimberly has a bachelor's degree in marine biology from Texas A&M University, a master's degree in biology from Southeastern Louisiana University and a graduate certificate in science communication from the University of California, Santa Cruz. She is a former reference editor for Live Science and Space.com. Her work has appeared in Inside Science, News from Science, the San Jose Mercury and others. Her favorite stories include those about animals and obscurities. A Texas native, Kim now lives in a California redwood forest.

 Live Science Plus
Live Science Plus





