10 Bizarre Diseases You Can Get Outdoors
Into the Woods ...

Frightening fungi, beastly bacteria and even deadly diseases — it's a wonder anyone heads outdoors anymore. With bugs, parasites and weird bacteria at every turn, what's to stop you from coming down with a rare disease?
But most of the time, people can enjoy the outdoors quite safely without too much fanfare, said Dr. Michelle Barron, an infectious disease specialist at the University of Colorado, Denver.
Knowledge and understanding of diseases can help alleviate people's fears, Barron told Live Science.
So, here's the lowdown on some of the strange diseases you could encounter on your next wilderness jaunt, and some tips on how to avoid them.
Giardia
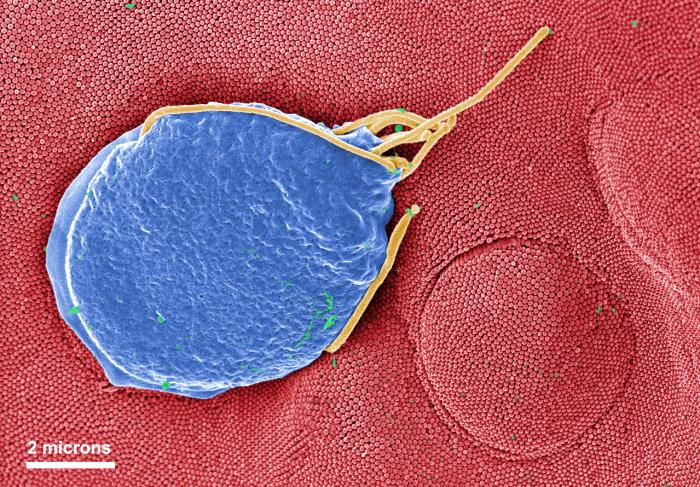
The above image shows a Giardia muris protozoan (in blue and yellow) attached to a single intestinal cell, shown in red.
A word to the wise in the wilderness: don't drink unfiltered water — no matter how clean or clear it may appear. You may swallow more than you bargained for; namely, the microscopic parasite Giardia.
The gastrointestinal symptoms that accompany many an-infection are no walk in the woods (think bloating, abdominal pain and watery diarrhea), but they're not so extreme that a person can't live with them, Barron said. Symptoms can last two to six weeks, but anti-parasitic drugs can decrease the amount of time that the symptoms last, according to the Centers for Disease Control and Prevention (CDC).
And while some parasites are only found in certain regions of the country, for Giardia, it doesn't matter where you are in the United States — according the CDC, itcan be found in every region.
Cryptosporidiosis

Giardia isn't the only parasite lurking in the water — there's also the microscopic parasite Cryptosporidium, which causes cryptosporidiosis (though both the disease and the parasite are referred to as "Crypto").
Unlike Giardia, the tiny protozoan parasite that causes Crypto is protected by an outer shell that allows it to survive for long periods of time without a host, and makes it resistant to certain disinfectants, according to the CDC.
People can become infected when they accidentally swallow water while they're swimming, Barron said. And if Crypto gets into a source of drinking water, entire towns may experience an outbreak, she said.
Barron noted that while the gastrointestinal symptoms are unpleasant — "they're not something you're going to ignore," she said — most people will recover on their own without treatment.
Naegleria fowleri

Naegleria fowleri — also known as the "brain-eating amoeba" — is as bad as its nickname implies. This single-celled microbe, which is found in warm freshwater (such as lakes, rivers and hot springs), causes a rare brain infection called primary amebic meningoencephalitis (PAM) and is almost always deadly. Between 1964 and 2014, there have been only 133 PAM infections in the U.S., and only three people have survived, according to the CDC.
But a person can only become infected if the microbe enters the body through the nose — in what sounds like something out of a sci-fi movie, the amoeba migrates along the olfactory nerve to the brain, where it begins to destroy the brain tissue. Drinking contaminated water, on the other hand, will not lead to an infection.
Histoplasmosis
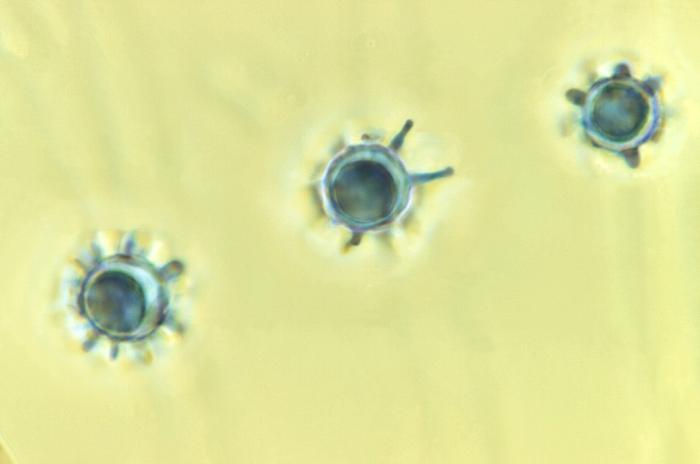
The above image shows three spores of Histoplasma capsulatum, the fungi that cause histoplasmosis.
If you're planning on doing some spelunking this summer, watch out for histoplasmosis, also known as "caver's disease." The fungus that causes this infection is found in bat droppings, which cavers may inhale when exploring.
Most histoplasmosis infections are asymptomatic, Barron said, who has seen patients with signs of past infections who never reported any symptoms (the infection can show up as a white spot on a chest x-ray, she said). For those who do come down with symptoms, the infection is similar to pneumonia, but anti-fungal medications can treat it.
But the great outdoors isn't the only place you can find histoplasmosis — people have also been known to become infected after cleaning their chicken coops, Barron said.
Valley fever

This infection occurs when people inhale fungi that belong to the group Coccidiodes, which are found in the southwestern United States. The tiny spores live in the desert dirt, and on windy days, they can get blown around, Barron said. (This can make valley fever difficult to avoid in certain regions, she added.)
Not everyone gets sick from breathing in the fungus, Barron said. Of those people who do breathe it in, the CDC reports that 40 percent will not develop any symptoms. The people who do get sick may have symptoms similar to the flu, but in severe cases, they can also develop pneumonia, according to the CDC.
The number of reported cases of valley fever has been increasing since 1998 — in 2011, there were over 20,000 cases, according to the CDC. The increase could be due in part to increasing awareness of the disease, but it could also be due to changes in the environment. Changes in temperature and rainfall affect how the fungus grows and how much of it is in the air, according to the CDC.
Blastomycosis

Another inhaled fungal infection, blastomycosis, is caused by the Blastomyces dermatitidis fungus.
Unlike valley fever, which thrives in drier areas, the Blastomyces fungus likes moist soil and is often found where there is rotting wood and leaves, according to the National Institutes of Health (NIH).
A lot of the fungal diseases are found in specific parts of the country, and Blastomyces is no exception — it's mainly found around the Great Lakes and the Mississippi and Ohio River valleys, according to the CDC (think of places with abundant moist soil).
Like other inhaled fungal infections, Blastomyces doesn't always cause symptoms, but when it does, it often resembles pneumonia, Barron said. People with mild infections don't necessarily need medication, but those with more severe infections might be prescribed an anti-fungal medication, according to the NIH.
Babesiosis
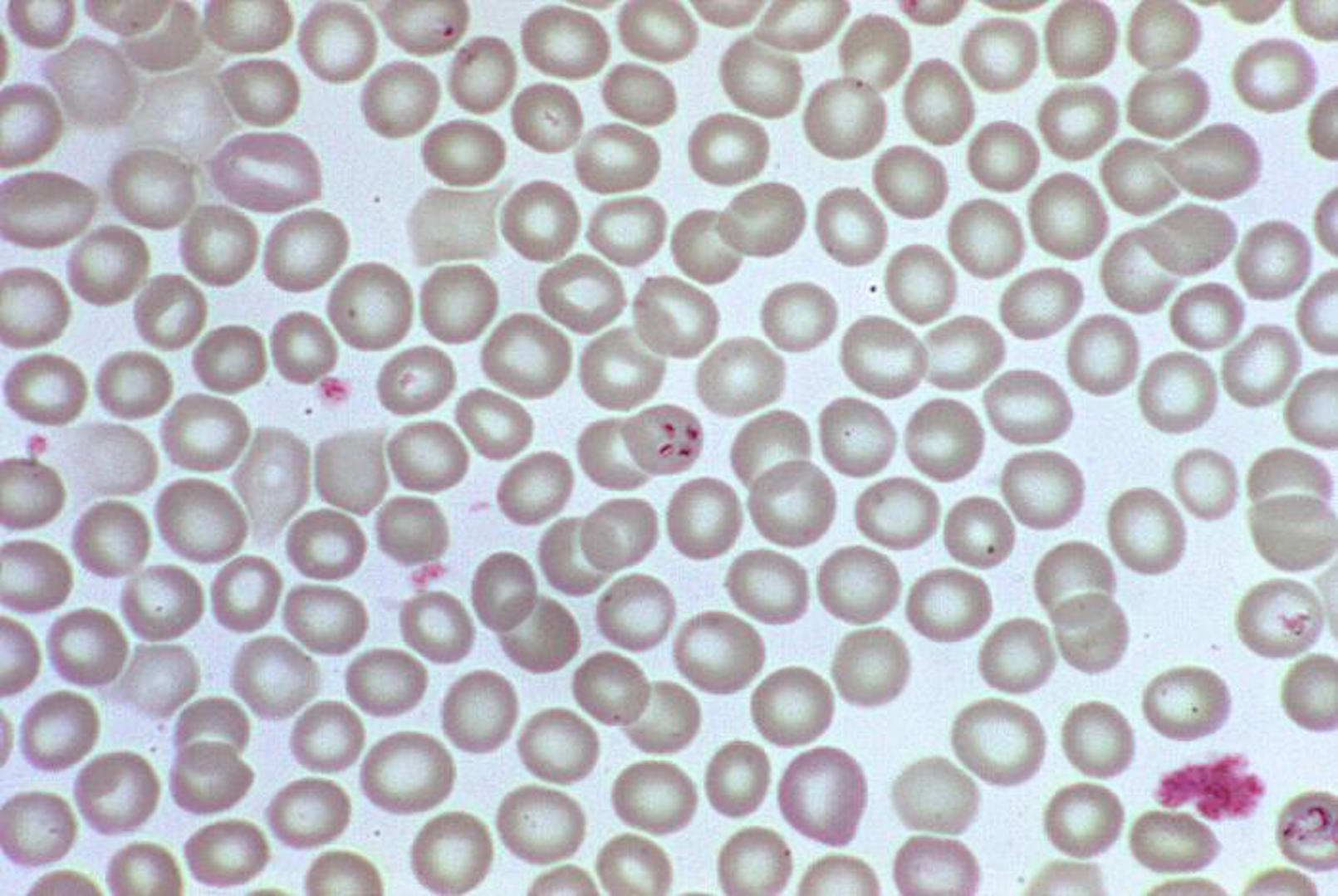
In the above image, the dark spots — here appearing in a "tetrad" configuration — are the babesia parasite in a red blood cell.
This tick-borne disease is most commonly found in the upper Midwest and eastern part of the United States and is transmitted by a bite from a deer tick, according to the CDC. If deer ticks sound familiar, it's because they're also responsible for transmitting Lyme disease. But don't fret if you haven't heard of it, compared with Lyme disease, for which there were over 25,000 confirmed cases in 2013, the CDC only reported 1,762 cases of babesiosis in the same year.
While the symptoms start out non-specific, people can get pretty sick from babesiosis, Barron said. The parasite infects red blood cells, so people with the disease experience symptoms such as fatigue and anemia, she said. However, the infection is easily treated with medications, she said.
Infections are diagnosed by looking at a thin layer of the person's blood under the microscope to see if there are any parasites in the blood. The parasites are actually easy to see, Barron said.
Hantavirus

A 2012 outbreak of this disease in Yosemite National Park sickened 10 people — three of whom died.
The virus is spread by rodents, and is found in their droppings, urine and saliva, according to the CDC. When the virus is stirred up (for example, when someone sweeps up mouse droppings), it can be become airborne, and people can breathe it in.
Hantavirus has a high mortality rate, in part because people may not get treatment until they're really sick, or because they just don't recognize it, Barron said. (In fact, there is no treatment for the virus other than supportive care, she added.) The symptoms can feel like the flu, however, one unique symptom is that the virus decreases the number of platelets a person has in their blood, she said. Platelets help blood clot, so this can put people a high risk for dangerous bleeding, she said.
The virus can be found in places where rodents are common, such as unused buildings. In the case of the Yosemite outbreak, experts believe people contracted the virus while staying in cabins in the park.
If you know you're in an area where the rodents are found, make sure there's lots of ventilation, or where a mask so you don't inhale anything, Barron said.
Rabbit fever

The source of rabbit fever should come as no surprise: You can pick up the bacterium that causes the disease from coming in contact with a sick rabbit. However, rabbits aren't the only source of the infection, which is also known as tularemia. You can also become infected by a tick bite.
Rabbit fever is normally very rare: In the past two decades, there have only been about 125 cases reported each year. However, the CDC reported an uptick in the disease in 2015, when 100 cases were diagnosed in the first nine months of the year.
The symptoms of rabbit fever depend on how a person becomes infected. For example, if a person becomes infected through a cut or a tick bite, they'll develop a wound in that spot. Inhaling the bacteria can lead to pneumonia, which affects the lungs. All of the infections are accompanied by a fever.
Because of the relative rarity of rabbit fever, awareness is important, Barron said. For example, if you live in an area that normally has a lot of rabbits, and then you notice that there aren't any rabbits around, that could be a sign that there's an infection circulating, she said. [10 Deadly Diseases That Hopped Across Species]
Plague
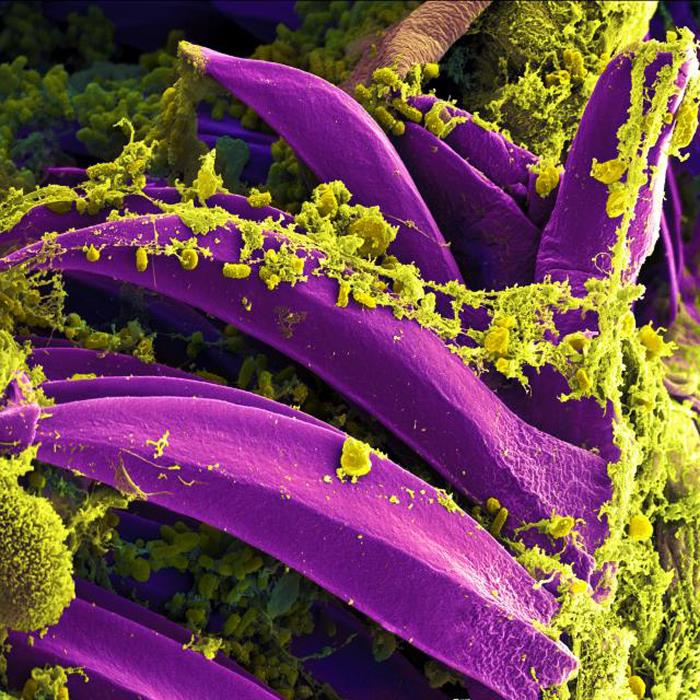
Yes, plague is alive and well in the United States, but thanks to modern medicine, it's highly unlikely we'll see a repeat of the Black Death anytime soon.
Today, the infection, which is caused by the bacterium Yersinia pestis, is easily treated with antibiotics, Barron said. It's only when an infection goes unidentified that it can come deadly, she said.
Plague infections come in two forms. One form is the bubonic plague, which causes the large, dark swollen lymph nodes (known as "bubos") that are commonly associated with the disease, Barron said. These will occur close to the area where a person got bit by a flea and are hard to miss, she said.
The other form is the pneumonic plague, which occurs when the bacteria is inhaled, Barron said. This is type is more deadly, in part because the symptoms can be non-specific and just feel like the flu, she said. Awareness of where you've been and what's been circulating in your area can help a doctor make the diagnosis, she said.
And while rats may have spread the plague through Europe, prairie dogs also harbor the fleas that carry the plague virus — "it lives quite happily" among them, Barron added.
Get the world’s most fascinating discoveries delivered straight to your inbox.

