Why is endometriosis so hard to diagnose?
Endometriosis often has vague symptoms that overlap with other conditions, and there are no non-invasive ways to definitively diagnose the condition.

Endometriosis occurs when the lining of the uterus, called the endometrium, grows outside the uterus, often in places such as the fallopian tubes, ovaries or along the pelvis. The condition can cause cysts, heavy periods, severe cramps and even infertility, according to the Office on Women's Health, part of the U.S. Department of Health and Human Services.
Early diagnosis of endometriosis helps reduce the number of emergency visits and inpatient hospitalizations, while minimizing the cost burden on the healthcare system, according to a 2020 review published in the journal Advances in Therapy. However, U.S. residents with endometriosis have the condition for 10 years on average before receiving a proper diagnosis, according to Yale Medicine.
Dr. Adiele Hoffman, a general practitioner and medical advisor at the period-tracking app Flo Health, told Live Science that the problem of delayed endometriosis diagnosis is not limited to the U.S., and that time from symptom onset to diagnosis ranges from 7.4 to 10.4 years in European countries.
So why is endometriosis so hard to diagnose? Here, we discuss a number of possible reasons why many endometriosis cases fall under the radar.
How is endometriosis diagnosed?
No simple blood test, scan or marker can easily diagnose endometriosis, Hoffman told Live Science.
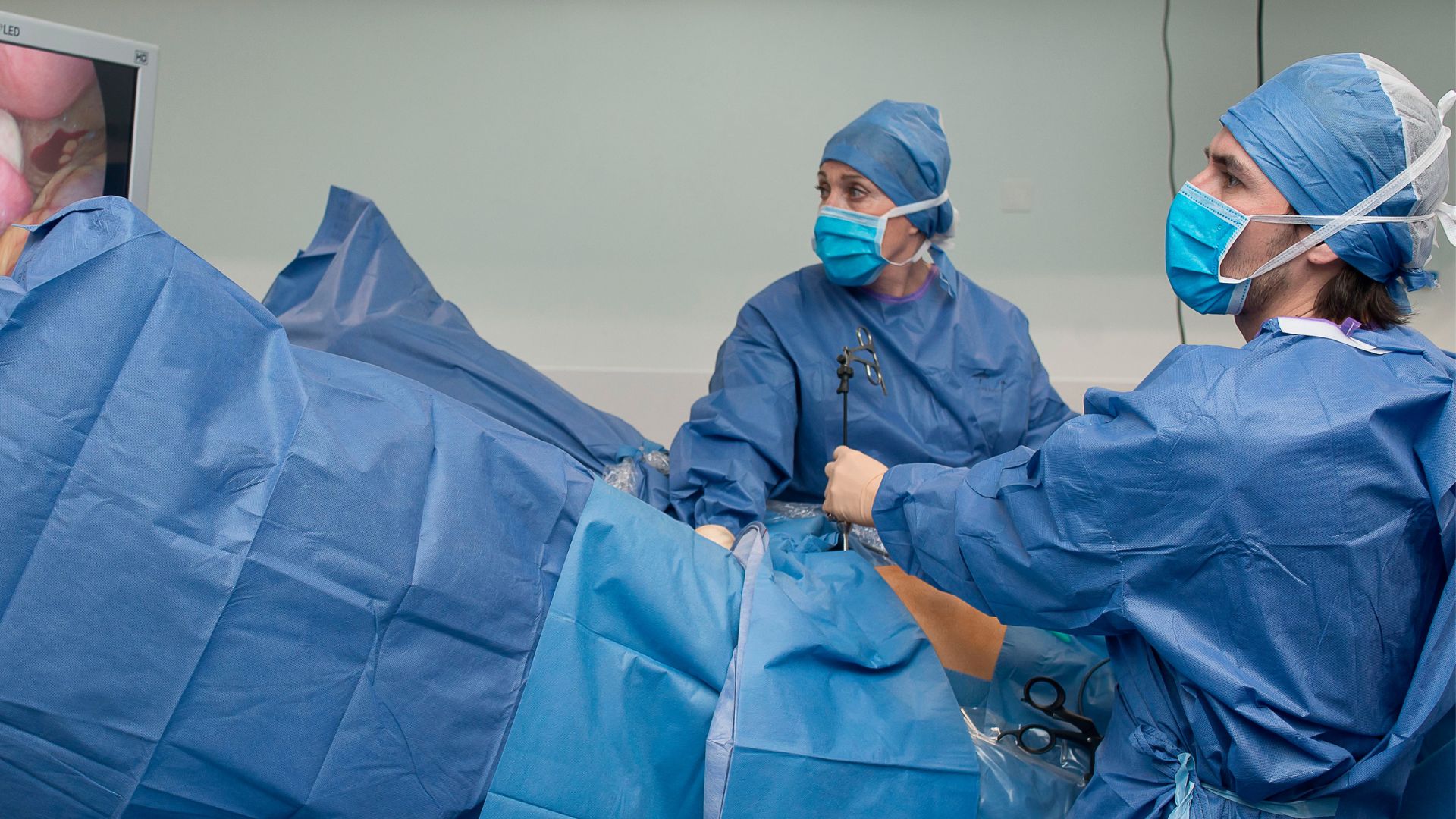
Definitive diagnosis requires laparoscopy, a keyhole surgery that makes a few small incisions in the abdomen to peer inside the pelvis, Hoffman said. Laparoscopy is not practical as a first-line diagnostic tool, according to a 2018 review published in the journal Current Obstetrics and Gynecology Reports. It is relatively invasive and expensive, and it also carries a risk of complications, such as injury to blood vessels or bowel perforation. Moreover, patients can report few symptoms and still have extensive disease, or report extreme pain and have relatively little physical evidence of endometriotic lesions.
"Laparoscopy requires the surgeon to be able to find and visualize the endometriosis which is not always possible for hidden or really deep lesions. Also, a woman can have severe symptoms with only a small amount of endometriosis actually seen during a laparoscopy," Hoffman said.
Get the world’s most fascinating discoveries delivered straight to your inbox.
Therefore, preliminary diagnosis of endometriosis is usually done on the basis of clinical history, physical examination and imaging tests, such as ultrasound or magnetic resonance imaging (MRI). "These are clinical indicators that can point to endometriosis and some specialists have called for it to be diagnosed based on them alone, in the hope this could lead to earlier diagnosis," she said.
However, this strategy of creating a "working diagnosis" also has drawbacks, Hoffman said.
The most common symptom of endometriosis is pain that is often worse around the time of menstruation, Dr. Susanna Unsworth, a women's health specialist in England and in-house gynecologist for INTIMINA, feminine care brand, told Live Science. But women are often told that period pain is normal or that it will naturally improve after pregnancy, Unsworth said. That's not the case.
While "a small amount of pain can be expected with a period, this pain should not impact on daily life," she said. "Lots of women feel they should just 'get on with it' if they do experience more significant pain, with many not even seeking help."
Furthermore, pain is not specific to endometriosis alone, Unsworth said. Symptoms can overlap with other common conditions.
Fibroids, pelvic inflammatory disease and ovarian cysts can cause similar symptoms, as can recurrent urinary tract infections, celiac disease and irritable bowel syndrome, Hoffman said. That can make endometriosis difficult to diagnose on the basis of patient-reported pain.
"Another confusing factor is that endometriosis doesn't cause any symptoms at all in up to 7% of women and is only diagnosed as a part of investigations for infertility," Hoffman said.
Another drawback of creating a working diagnosis is that patients with endometriosis will often have normal findings on a pelvic exam, in which doctors feel for large cysts or scars behind the uterus.
And ultrasounds and MRI can often miss endometriotic lesions, Unsworth said. For example, ultrasound may not detect endometriosis located in the abdominal cavity or within vital organs, according to a 2018 review published in the journal Current Obstetrics and Gynecology Reports.
When imaging tests do not show any ovarian cysts, doctors may prescribe medications as a part of the diagnostic process, according to the Office on Women's Health. These include hormonal birth control to help lessen period pain, or gonadotropin-releasing hormone (GnRH) agonists to block the menstrual cycle and lower the amount of estrogen within the body. Doctors may diagnose endometriosis if the symptoms get better with these medications.
What causes endometriosis?
Doctors still do not fully understand why endometriosis occurs. However, our understanding of this condition is changing, Unsworth told Live Science.
"A commonly accepted view is that of 'retrograde menstruation' — where endometrial tissue flows back from the womb, via the fallopian tubes and into the abdomen. However, it is not clear why this may happen," she said.
It is also possible that the immune system overreacts to this process, leading to endometriosis, she said.
Related: What are the causes of endometriosis?
How is endometriosis treated?
Current treatments for endometriosis include pain medications, hormone therapy (such as birth control pills and GnRH agonists) and laparoscopic surgery to remove endometrial scar tissue, according to the National Institutes of Health. In severe cases, people with endometriosis may undergo a hysterectomy, which is a partial or total surgical removal of the uterus.
But new treatments may be on the horizon.
For instance, a study published Feb. 22, 2023 in the journal Science found that a monoclonal antibody reduced the formation of endometrial scar tissue in monkeys. This research could eventually lead to similar treatments for human patients with endometriosis.
RELATED STORIES
And scientists have identified several genes associated with endometriosis, according to a March 13, 2023 study in the journal Nature Genetics. "Finding genetic reasons why some women develop endometriosis may open up the possibility of gene therapy as future treatments," Unsworth said.
Scientists are researching non-hormonal medical treatments and trying to evaluate how well surgery actually works for endometriosis, Hoffman said. They're also trying to find better diagnostic tools, according to a 2022 review published in the journal Current Opinion in Obstetrics & Gynecology. The most promising potential markers are signaling proteins, byproducts of metabolism, markers of gene activity and certain bacteria in the gut and cervical mucus, according to the review.

Anna Gora is a health writer at Live Science, having previously worked across Coach, Fit&Well, T3, TechRadar and Tom's Guide. She is a certified personal trainer, nutritionist and health coach with nearly 10 years of professional experience. Anna holds a Bachelor's degree in Nutrition from the Warsaw University of Life Sciences, a Master’s degree in Nutrition, Physical Activity & Public Health from the University of Bristol, as well as various health coaching certificates. She is passionate about empowering people to live a healthy lifestyle and promoting the benefits of a plant-based diet.

 Live Science Plus
Live Science Plus





