'Unbelievable Event': Uterus Transplanted in a First for US


A 26-year-old woman who learned at age 16 that she would be unable to have children now has a chance to do so, thanks to the first uterus transplant in the U.S. The transplant provides hope for women who are unable to have babies due to uterus-related issues, said the doctors who completed the transplant.
"This is an unbelievable event" and the patient is doing very well, said Dr. Andreas Tzakis, the program director of the Cleveland Clinic's Transplant Center, who led the surgery.
A condition called uterine factor infertility — in which a woman is unable to get pregnant because she either does not have a uterus, or the uterus does not function properly — affects an estimated 50,000 women in the United States, according to the Cleveland Clinic. [Donated Uterus Transplanted Into Patient | Animation]
A uterus transplant can enable a woman with uterine factor infertility to become pregnant and deliver a baby.
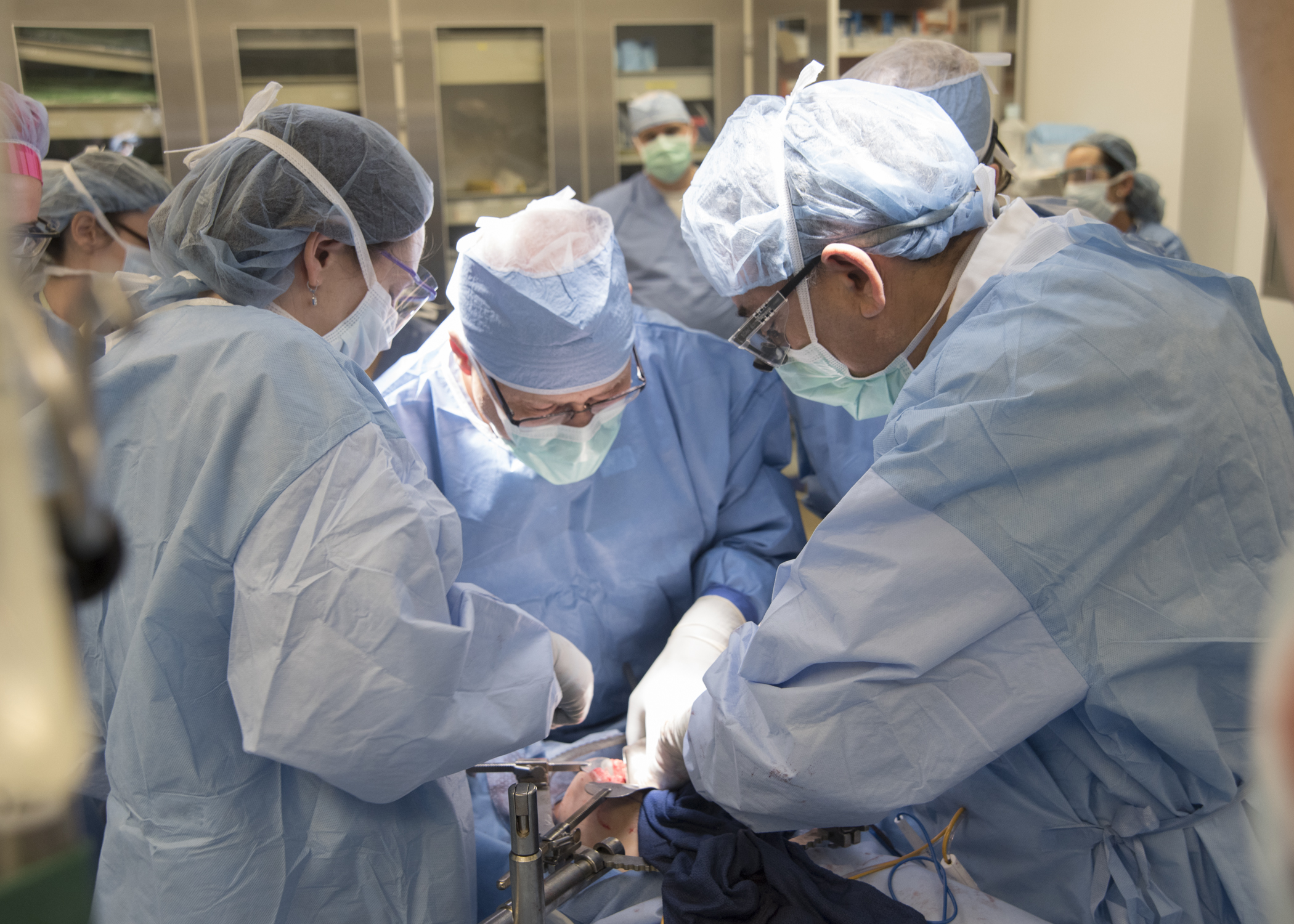
The surgery took place February 2016, and required about 9 hours, said Dr. Toby Cosgrove, the CEO and president of the Cleveland Clinic, speaking at a news conference today (March 7). The team included eight surgeons and about 70 other caregivers, including fertility experts and bioethicists, he said.
The transplant
Tzakis and his team worked very closely with doctors in Sweden, who completed the world's first uterus transplant in 2015.
Get the world’s most fascinating discoveries delivered straight to your inbox.
In the Cleveland transplant, the uterus was taken from a deceased donor, Tzakis said.
The surgeons used transplant techniques that have been well-established for other types of organ transplants. However, the surgery is a little more complex because the transplant site is deep within the pelvis and therefore more difficult to access, Tzakis said.
Dr. Rebecca Flyckt, an OB/GYN surgeon who was part of the team, elaborated upon the surgery.
The the most important of part of the transplant is to connect blood vessels, Flyckt said at the news conference. First, the uterine arteries and veins were connected to the recipient's blood vessels, she said. Once these were connected, the transplanted uterus started to turn pink, which indicated that blood is flowing, she said. [The 9 Most Interesting Transplants]
Next, the surgeons connected the uterus to the vagina, as well as the connective tissue in the pelvis that helps anchor the uterus in place, she said.
The transplanted uterus also included the cervix and the upper part of the vagina.
Preparing for pregnancy
The goal of the surgery is to allow the woman to have a baby, but the woman needs to wait at least a year before trying to get pregnant, Flyckt said.
The team in Cleveland screened more than 250 women, and ultimately selected 10 who will receive transplants.
All of the women were born with normal ovaries that produce healthy eggs, Flyckt said. But without a uterus, the eggs have nowhere to go, she said.
Before the transplant, the women will undergo in vitro fertilization, Flyckt said. They will bank six to 10 embryos before they can be considered for the transplant, she said.
After the transplant is completed, the women need to wait one full year before pregnancy is considered, Flyckt said. This is to make ensure that the woman is taking lower dosages of anti-rejection medications, which suppress the immune system, she said.
Then, the doctors will begin to implant the embryos, Flyckt said. (Because the fallopian tubes were not transplanted, the patient cannot get pregnant through sex.)
Dr. Uma Perni, an OB-GYN specializing in high-risk pregnancies, said the team plans to deliver babies via cesarean section on any women who have undergone uterus transplants, because there are many unknowns about vaginal delivery with a transplanted uterus.
It isn't clear exactly how a transplanted uterus would respond to normal signs of labor, and it's possible that the complex connections that were made during the transplant could be disrupted during labor, Perni said. Ultimately, it isn't clear how the patient's body would tolerate a vaginal delivery, she said.
Perni added that the risk of a preterm delivery is a little higher in women who have undergone a uterus transplant, compared with the average woman. Because of this, the team will be closely monitoring the patient in her third trimester, she said. Ultimately, they hope they can get very close to 37 weeks, which is considered full term, before delivering the baby, she said.
A temporary transplant
Unlike other transplanted organs, which can remain in patients for the rest of their lives, the doctors will likely remove the uterus after one or two pregnancies.
The reason for removing the uterus is to minimize the amount of time that patients must take anti-rejection medications, Falcone said.
Falcone estimated the patient would have the transplanted uterus for about five years, or two pregnancies: There is one year to wait after the transplant surgery, then nine months for the first pregnancy, a year to a year and a half between pregnancies, and then the second pregnancy. [Blossoming Bodies: 8 Odd Changes That Happen During Pregnancy]
It's an "ephemeral transplant," Tzakis said. One option is to remove the uterus, but another option is to wait and see, he said. The team will be careful in deciding how they will proceed — they may do a second surgery, or they may not, he said.
Still, the patient will be monitored for signs that the body is rejecting the uterus, said Dr. Bijan Eghtesad, a transplant surgeon who was part of the team.
In order to monitor the patient, the doctors will have to periodically check the cervix, he said. By looking at the mucosal lining of the cervix, as well as the vagina, they can determine what is going on, he said. Discoloration may suggest rejection, he said.
Follow Sara G. Miller on Twitter @SaraGMiller. Follow Live Science @livescience, Facebook & Google+. Originally published on Live Science.


 Live Science Plus
Live Science Plus




