Preeclampsia: Signs, Symptoms & Treatment
Get the world’s most fascinating discoveries delivered straight to your inbox.
You are now subscribed
Your newsletter sign-up was successful
Want to add more newsletters?
Join the club
Get full access to premium articles, exclusive features and a growing list of member rewards.
Preeclampsia is a serious complication that can develop usually after the 20th week of pregnancy. The condition is diagnosed when a pregnant woman has both high blood pressure as well as a high level of protein in her urine, which is known as proteinuria. (Proteinuria is often a sign that the mother's kidneys are not working properly.)
Preeclampsia can have systemic, or body-wide effects, said Dr. Arun Jeyabalan, a maternal and fetal medicine specialist at Magee-Womens Hospital at the University of Pittsburgh Medical Center, who has done research on preeclampsia.
The disorder can affect other organs in the mother's body. A woman may also have kidney damage, liver failure, neurological symptoms, such as severe headaches, seizures, and fluid on the lungs (known as pulmonary edema), Jeyabalan said.
Article continues belowShe explained that the cause of preeclampsia may be related to substances released from the placenta that can affect maternal blood vessels. When blood flow to the placenta is reduced, the fetus may not get the nourishment and oxygen it needs for growth.
Preeclampsia tends to happen during the second half of pregnancy, and more commonly in the third trimester, Jeyabalan said. It can also occur in the postpartum period, up to six weeks after delivering a baby.
In the past, preeclampsia may have been called "toxemia" or "pregnancy-induced hypertension," Jeyabalan said. But these outdated terms are no longer used. They have been replaced by the terms "gestational hypertension," which is when elevated blood pressure is detected in a woman after the 20th week of pregnancy, but she does not also have protein in her urine, which would be considered "preeclampsia."
In the United States, preeclampsia affects one in every 12 pregnancies or 5 to 8 percent of all births, according to the Preeclampsia Foundation.
Get the world’s most fascinating discoveries delivered straight to your inbox.
Preeclampsia can also be a scary condition because it can kill mothers and babies worldwide, and it may lead to long-term health problems, Jeyabalan said.
Symptoms
Symptoms of preeclampsia may come on gradually or flare up suddenly during pregnancy or within six weeks of giving birth.
"We tell pregnant women to watch out for symptoms in the third trimester and to call their obstetrician or midwife if they have them," Jeyabalan said.
Symptoms may include:
- Visual changes, such as consistently seeing spots or flashing lights in front of the eyes, blurred vision or being oversensitive to light
- Severe headache that won't go away
- Swelling, especially around the ankles and feet, and in the hands and face. "Although swelling is common during pregnancy, seeing it in these areas can raise the suspicion of preeclampsia," Jeyabalan said.
- Pain in the upper right abdomen, which is where the liver is located
- Difficulty breathing
- Sudden nausea or vomiting in the second half of pregnancy
- In its most severe form, seizures can occur in a pregnant woman with preeclampsia, resulting in a condition known as "eclampsia," which is considered a medical emergency and needs immediate treatment because it can be life-threatening.
Risk factors
These following women are more likely to develop preeclampsia:
- Women who have had chronic hypertension (high blood pressure before becoming pregnant), kidney disease, lupus or prediabetes prior to becoming pregnant
- Women who are over age 40 or under age 18
- Women who are experiencing a first pregnancy
- Women who developed high blood pressure or preeclampsia during a previous pregnancy, especially if these complications occurred early in the pregnancy
- Women who are obese before becoming pregnant
- Women who are giving birth to multiples, such as twins or triplets
Causes
Exactly how pregnancy causes preeclampsia is unknown making it a complicated and challenging condition for physicians and women alike, Jeyabalan told Live Science.
Sometimes women who are diagnosed with the condition ask Jeyabalan, "Is there anything I did to cause preeclampsia?" They want to know if eating too much salt, or being under a lot of stress or getting too much exercise may have triggered their symptoms.
Jeyabalan tells women that the cause of preeclampsia is not well understood.
But there are several theories:
Since some women come into pregnancy at higher risk of preeclampsia because of an older age or pre-existing kidney disease or lupus, the disorder may be related to underlying vascular conditions, which means blood vessel problems, Jeyabalan said.
She said another thought is that preeclampsia may have its origins in how the placenta implants to the uterus, which affects its function of delivering nutrients and oxygen to the fetus. These factors may then influence how the placenta reacts in the later stages of pregnancy, which is when the condition is typically diagnosed.
A more recent theory that has garnered lots of attention is the role of angiogenic factors, Jeyabalan said. This theory proposes that factors regulating the formation of new blood vessels in the placenta are overproduced. This might influence blood vessel health in the mother and could lead to high blood pressure and kidney damage, according to the Preeclampsia Foundation.
There may also be a genetic component to preeclampsia, Jeyabalan said. It tends to run in families, so a woman with a mother, sister, aunt or grandmother who has had the condition is at higher risk of developing it.
Diagnosis and tests
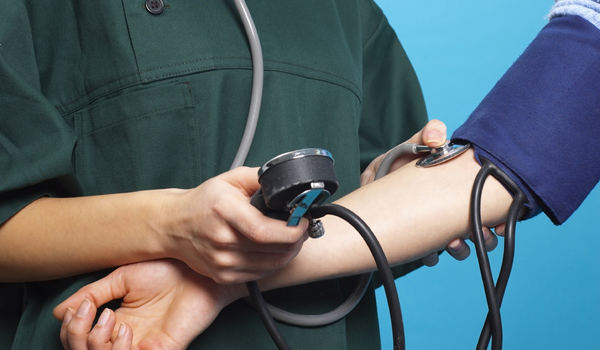
During a woman's prenatal visits, her blood pressure is checked and her urine is tested. This regular monitoring would detect if her blood pressure levels were high, meaning a systolic blood pressure reading (the top number) is 140 or above, and a diastolic (the bottom number) reading is 90 or above, on at least two checks at least 6 weeks apart, Jeyabalan said.
Besides high blood pressure, a pregnant woman would also need to have high levels of protein (above 300 milligrams) detected in her urine.
Once a diagnosis of preeclampsia is made, a mother-to-be's blood pressure and urine tests will be closely monitored because the disorder may progress quickly. She will also be carefully monitored to evaluate whether the disorder might be affecting other organs, such as her kidneys, liver, brain and lungs.
Ultrasounds tests can be used to determine if the fetus is growing well. Fetal well-being can also be evaluated by monitoring fetal heart beat and contraction patterns as well as fetal kick counts, Jeyabalan said.
Risks to mother and baby
In serious cases of preeclampsia, a pregnant woman may need to deliver her baby early before the fetus is fully grown. A mother-to-be with the condition is also at increased risk of serious complications, including seizures, organ damage to the liver and kidneys, and possibly death.
Once a woman has had preeclampsia during pregnancy, she has a 10 to 20 percent chance of developing it again, Jeyabalan said. But her risk is much higher if she had a severe form of preeclampsia, or the condition came on before 34 weeks of pregnancy, she said.
Having preeclampsia during pregnancy could affect a woman's long-term health. Later in life, she faces a greater risk of heart disease, stroke and high blood pressure.
When a mother has preeclampsia, a developing fetus can have growth problems. Others risk to the baby include low birth weight and premature birth along with the potential for lifelong complications from being delivered too early. Some newborns, especially in developing countries, may not survive pre-term deliveries and there is also an increased risk of stillbirth.
Treatment and medication
"Delivery is the beginning of the cure for preeclampsia," Jeyabalan said. That's because a woman's symptoms usually seem to resolve after her baby is born.
But there are treatments available to prevent dangerous spikes in blood pressure or organ damage in a pregnant woman, and to prolong the pregnancy and delay the premature delivery of the fetus.
A woman may be put on high blood pressure medication that is safe to take during pregnancy, Jeyabalan said. In severe cases of preeclampsia, a woman may be given IV magnesium sulfate (an anticonvulsive medication) to prevent seizures.
Steroid injections may be given to help speed up lung development in the fetus in case an early delivery is needed.
Preeclampsia can be a progressive syndrome in which symptoms can quickly get worse, Jeyabalan said. So when treating it, doctors will attempt to strike the right balance between worsening disease in the mother and allowing the fetus to gain some maturity before delivery. "Sometimes we don't always have that luxury," Jeyabalan admitted.
In 2014, the U.S. Preventive Services Task Force, a government panel of medical experts, recommended that women who are at high risk for preeclampsia, such as women who have a history of preeclampsia or have chronic hypertension, should start taking a daily low-dose aspirin (81 milligrams) after 12 weeks of pregnancy. Taking one low-dose aspirin is safe during pregnancy.
Research suggests that high-risk women who took a daily low-aspirin after the first three months, reduced their risk for preeclampsia by 24 percent.
Preeclampsia is not always resolved once the baby is born. Some women will continue to have high blood pressure after childbirth and need to be monitored over a lifetime. These women may need anti-hypertensive medications to control their blood pressure, Jeyabalan said.
Women who had preeclampsia during pregnancy but may no longer be under the care of a maternal and fetal medicine specialist, need to inform their primary care physicians of this pregnancy complication, and they need to be followed more closely by their doctors for long-term cardiovascular disease, Jeyabalan said.
In fact, the American Heart Association recognized preeclampsia as a risk factor for heart attack and stroke in women, and they added it to their list of cardiovascular disease prevention guidelines for women in 2011.
Women with a history of preeclampsia are twice as likely to have a stroke and are four times as likely to have high blood pressure later in life," according to the American Heart Association.
But lifestyle changes, such as not smoking, eating a heart-healthy diet, achieving a healthy weight and exercising regularly, can all help a woman to reduce her chances of developing heart disease in the future.
Additional resources
Cari Nierenberg has been writing about health and wellness topics for online news outlets and print publications for more than two decades. Her work has been published by Live Science, The Washington Post, WebMD, Scientific American, among others. She has a Bachelor of Science degree in nutrition from Cornell University and a Master of Science degree in Nutrition and Communication from Boston University.
 Live Science Plus
Live Science Plus










