How Anthrax Kills: Toxins Damage Liver and Heart

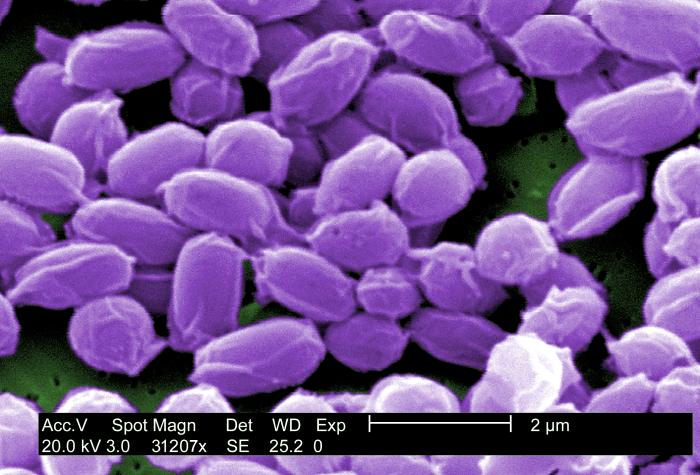
A new study of anthrax reveals why the infection is deadly.
The findings also offer clues that could be used to better treat people who are infected, which could possibly improve survival rates, researchers said in their study published Thursday (Aug. 29) in the journal Nature.
Doctors in developed nations rarely see anthrax cases, but if they do, it's important to treat the disease correctly, and as soon as possible, said Stephen Leppla, of the Laboratory for Infectious Diseases at the National Institutes of Health.
"The problem with clinicians treating anthrax is that nobody has much experience doing it," Leppla said. Understanding exactly how anthrax kills can help clinicians tailor better strategies.
Anthrax is caused by bacteria, and can infect people in one of three ways: people might inhale the spores, eat the spores, or take in spores via the skin. All three types of infection can be deadly, though the skin route of infection is much less so, according to the Centers for Disease Control and Prevention. Inhaled anthrax has a mortality rate of about 75 percent, while the gastrointestinal infection kills about 60 percent of infected people, even with treatment. Among those infected through their skin, anthrax mortality drops to 20 percent. [Tiny & Nasty: Images of Things That Make Us Sick]
In the developing world, people become infected though contact with livestock. In the U.S. and Europe, anthrax is now very rare -- only one or two cases appear yearly on average in the U.S.
Deadly toxins
Get the world’s most fascinating discoveries delivered straight to your inbox.
The bacteria themselves aren't what sickens and kills: it's the toxins the bacteria produce. A doctor can treat a patient with antibiotics and kill all the anthrax bacteria – antibiotics are very effective against the infection. But the toxins the bacteria made remain in the body, and continue damaging cells.
The two toxins produced by anthrax, called lethal toxin and edema toxin, damage many types of cells, but it was thought that their effects on endothelial cells, which line blood and lymph vessels, were what made anthrax so lethal.
In the new study, it was found that wasn't the case; rather, much of the toxins' action seems to be in the cells of the heart muscle and the liver.
To track down which cells anthrax targeted, the researchers looked at mice genetically altered so that a protein called CMG2, to which anthrax toxins bind, was absent from their endothelial cells. They compared these mice with another group that had CMG2.
Results showed that both sets of mice were similarly sensitive to anthrax, which meant that anthrax wasn't killing the mice via damage to endothelial cells.
The researchers next tested mice that were missing the CMG2 protein from their heart cells. Those mice survived the doses of lethal toxin much better than their litter mates that had the protein, which pointed to anthrax's effects on the heart muscle as the way that it kills.
Similarly, mice without CMG2 in their liver cells fared better when exposed to edema toxin than mice that expressed CMG2, showing that the edema toxin affects the liver.
Leppla noted that it is not clear whether the findings are also true of anthrax in people. Future experiments on primates would confirm the results, he said.
Follow LiveScience on Twitter @livescience. We're also on Facebook & Google+.


 Live Science Plus
Live Science Plus





