Rheumatoid Arthritis: Symptoms & Treatment

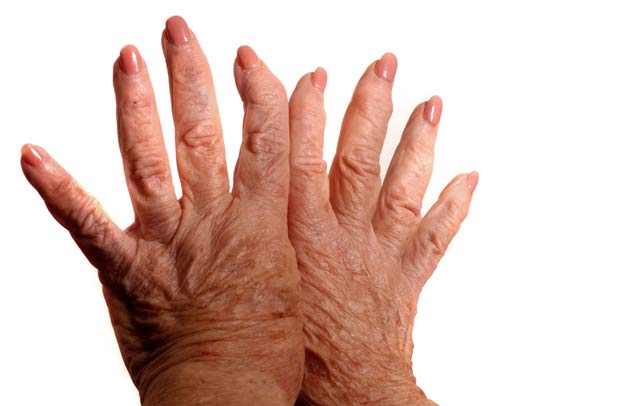
When the immune system goes awry and attacks the joints, it results in rheumatoid arthritis (RA). This disorder can cause significant pain and joint deformity by wearing away joint linings. It is a chronic, debilitating condition that has no cure, and it affects about 1.5 million people in the United States, according to the Arthritis Foundation.
"If the disease goes untreated, it can cause permanent damage to the joints. It can also cause other problems, such as inflammation in the lungs or the eyes," said Dr. Linda Mileti, a rheumatologist at the Cleveland Clinic. The disorder can increase the risk of cardiovascular disease as well, she added.
Joint damage can happen in the first two years in which a person has the disorder, according to the Arthritis Foundation. RA usually affects joints on both sides of the body equally, starting in the small joints of the wrists, hands, ankles and feet. Though this condition is not generally known as a lethal disease, people with RA are two times more likely to die than people of the same age without RA in the general population, according to the Arthritis Foundation.
Article continues belowCauses
Though doctors can characterize aspects of the disease, they do not know a cause. "RA is an autoimmune disorder with genetic susceptibility, but the cause is unknown," Dr. N. Lawrence Edwards, a professor of medicine at the University of Florida, told Live Science. Genetic susceptibility means that environmental factors, such as viral or bacterial infection, may be more likely to lead to RA in a person, due to that individual's inherited traits, according to the Mayo Clinic.
Other known risk factors include gender and age. RA is two to three times more common in women than men, according to the Mayo Clinic. It most commonly begins in middle age and occurs more frequently in older people, according to the National Institutes of Health, but RA can also affect older teenagers and young adults.
Another risk factor is smoking. Heavy, long-term smoking is a "very strong" risk factor for RA, according to the University of Maryland Medical Center.
Symptoms
RA symptoms can be very vague at the onset, resembling those of many other illnesses. They also vary from patient to patient and may come and go. According to the Mayo Clinic, symptoms include:
Get the world’s most fascinating discoveries delivered straight to your inbox.
- Joint pain
- Warm joints
- Swollen joints
- Swollen glands
- Fatigue or weakness
- Red, puffy hands
- Morning stiffness
- Fever
- Loss of appetite or weight loss
- Firm bumps under the skin on the arms
Diagnosis & tests
No single test can confirm RA, so doctors usually rely on a variety of tests to make a diagnosis. These examinations study joint structure or measure the amount of inflammation present in the body.
According to the Arthritis Foundation, tests include:
- Erythrocyte sedimentation rate (known as ESR or sed rate): This blood test measures how quickly red blood cells fall to the bottom of a test tube — the more quickly this happens, the more inflammation is present.
- Rheumatoid factor (RF): About 70 to 80 percent of those individuals whose blood contains RF also have rheumatoid arthritis.
- X-Rays and magnetic resonance imaging (MRI): Sometimes these imaging tests will show the loss of bone density surrounding joints, or will reveal swollen, soft tissue. They also serve as a valuable baseline to compare to future tests.
Medication & treatment
Because RA has no cure, treatments are usually life long and focus on relieving symptoms as well as preventing and slowing joint damage. "Patients need to understand that RA is a multisystem disease that can attack organs such as the lungs, bone marrow, eyes and cardiovascular system," Dr. Nathan Wei, a rheumatologist and director of the Arthritis Treatment Center in Frederick, Maryland, told Live Science. "Hence the need for aggressive treatment."
Many over-the-counter and prescription drugs are available to treat RA, though some have potentially serious side effects that must be carefully monitored. Usually, patients take these medicines in combination. According to the Mayo Clinic, RA medications include:
- NSAIDs: Nonsteroidal anti-inflammatory drugs, such as ibuprofen (commonly known as Advil or Motrin) and naproxen sodium (Aleve), reduce pain and inflammation. Prescription-strength NSAIDs are also available.
- Steroids: Prescription corticosteroids such as prednisone and methylprednisolone (Medrol) help control inflammation and slow joint damage by inhibiting the immune system.
- DMARDs: Disease-modifying anti-rheumatic drugs can save joints and tissues from permanent damage. These medicines include methotrexate (Rheumatrex, Trexall), leflunomide (Arava), hydroxychloroquine (Plaquenil) and others.
- Immunosuppressants: These drugs tame the immune system, and they include azathioprine (Imuran, Azasan), cyclosporine (Neoral, Sandimmune and Gengraf) and cyclophosphamide (Cytoxan).
- Biologics: These drugs inhibit inflammation-producing proteins called cytokines. The medicines include etanercept (Enbrel), infliximab (Remicade) and adalimumab (Humira).
Another major RA treatment is surgery, which is an option when drugs cannot prevent or slow joint damage. According to the NIH, surgical procedures for RA include tendon repair; total joint replacement therapy, which substitutes man-made joints for damaged ones; synovectomy, which removes the inflamed synovial tissue; and joint fusion (arthrodesis), which can stabilize joints, increase mobility and relieve pain.
Self-care can help people manage RA symptoms, the Mayo Clinic said. Light exercise, such as walking, swimming or water aerobics, can help strengthen the muscles around joints. Applying heat may help ease pain and relex muscles, while applying cold may dull the pain. Relaxation techniques, such as deep breathing, hypnosis and guided imagery, can also help control pain.
Additional resources
- Dr. Michael Weisman, a rheumatology expert at UCLA, presents an update on the latest treatments (YouTube video).
- Arthritis Today magazine offers news and information about living with arthritis.
- The American College of Rheumatology provides a downloadable fact sheet on rheumatoid arthritis.
