Are ventilators being overused on COVID-19 patients?
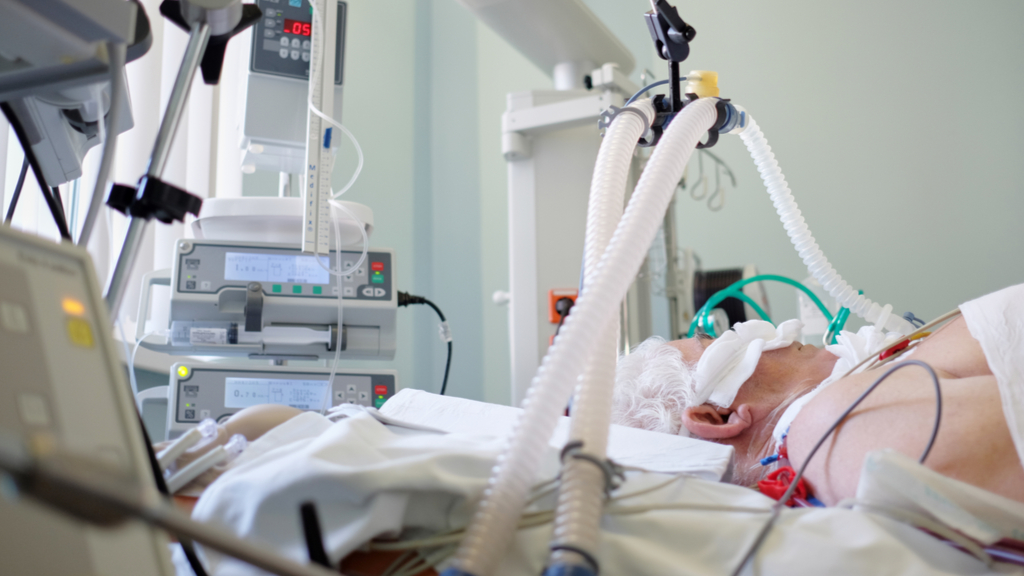
Not all patients with severe COVID-19 infection may benefit from a ventilator.

Coronavirus FAQ
—Coronavirus in the US: Map & cases
—What are the symptoms of COVID-19?
—How deadly is the new coronavirus?
—How long does coronavirus last on surfaces?
—Is there a cure for COVID-19?
—How does COVID-19 compare with seasonal flu?
—How does the coronavirus spread?
—Can people spread the coronavirus after they recover?
Some physicians caring for COVID-19 patients question whether the threshold for placing someone on a ventilator should be raised, given that the breathing machines are in critically short supply nationwide, Stat News reported.
"I think we may indeed be able to support a subset of these patients" with less invasive breathing support, Dr. Sohan Japa, an internal medicine physician at Brigham and Women's Hospital in Boston told Stat News. Ventilators push oxygen into the lungs via a tube placed in the mouth, nose or a hole in the front of the neck; but less invasive devices like the breathing masks for sleep apnea could be used to treat some COVID-19 patients, at least at first.
Indeed, for COVID-19 patients who need breathing assistance, many hospitals are starting them off on sleep apnea devices or nasal cannulas, which deliver air into the nose through a pronged tube, Dr. Greg Martin, a critical care physician at Emory University School of Medicine in Atlanta , told Stat News.
These noninvasive devices offer some advantages compared with ventilators. For example, the process of intubating patients — placing a tube into their airway — to hook them up to a ventilator requires doctors to sedate patients for long periods of time, so the machine can take over the work of breathing, Stat News reported.
In contrast, noninvasive breathing support devices don't "require sedation, and the patient [remains conscious and] can participate in his care," Martin said. If that person's respiratory issues degrade further, then doctors can put them on a mechanical ventilator," he added.
Related: 10 deadly diseases that hopped across species
Physicians typically determine who to put on a ventilator by monitoring their levels of blood-oxygen, or the available oxygen circulating in their bloodstream. Normal amounts — called oxygen saturation rates — range between 95% and 100% blood-oxygen, whereas a rate of 93% signals physicians that a patient may soon suffer organ damage due to a lack of oxygen, according to Stat News. If blood-oxygen levels dip and remain at 80% or below, the damage can be fatal.
Get the world’s most fascinating discoveries delivered straight to your inbox.
At the 93% mark, patients with other forms of severe pneumonia or respiratory distress are first placed on noninvasive devices, but if these simpler measures don't help, they are moved onto a ventilator. Some patients with COVID-19 blow quickly past the 93% percent threshold, as their blood-oxygen levels fall below 70%, Stat News reported. Despite their apparent lack of oxygen, however, a subset of these patients don't develop shortness of breath, cognitive impairment, or heart or organ abnormalities, as would be expected.
"The patients in front of me are unlike any I've ever seen. … They looked a lot more like they had altitude sickness than pneumonia," Dr. Cameron Kyle-Sidell, a Brooklyn, New York-based physician trained in emergency medicine and critical care, told Medscape, a website that provides medical information to health professionals. This odd array of symptoms may emerge because the lungs continue to clear carbon dioxide from the blood without absorbing adequate levels of oxygen, Stat News reported. A build-up of carbon dioxide would trigger the hyperventilation, flushed skin, headaches and dizziness often associated with poor lung function, but if levels remain normal, these symptoms may not arise as expected, according to StatPearls, a database of medical reference articles.
Patients with low blood-oxygen levels but few signs of distress or organ damage may not benefit from ventilation, according to researchers from Italy and Germany who submitted a letter published March 30 in the American Journal of Respiratory and Critical Care Medicine. In the letter, they described patients with these traits in Italy and Germany, noting that their lungs appeared relatively healthy as compared with COVID-19 patients with acute respiratory distress, a condition where the air sacs in the lungs fill with fluid.
Even if patients do develop acute respiratory distress, they may not benefit from ventilation either. The thick fluid clogging up the lungs "limits oxygen transfer from the lungs to the blood, even when a machine pumps in oxygen," Dr. Muriel Gillick, a geriatric and palliative care physician at Harvard Medical School, told Stat News. In this case, placing a patient on a ventilator could damage their lungs by introducing too much pressure into the organ, she said.
Furthermore, reports from Wuhan, Seattle and cities in Italy now suggest that placing patients on ventilators may not significantly improve their chances of recovery or survival. "Contrary to the impression that if extremely ill patients with COVID-19 are treated with ventilators they will live and if they are not, they will die, the reality is far different," Gillick said.
Given the available data and the unfamiliar nature of COVID-19, "I think we have to be more nuanced about who we intubate," Japa said. Noninvasive breathing devices do pose some threat to health care workers, as they can release aerosolized particles of the virus into the air while in use, Live Science previously reported. But the devices may prove to be the best option for patients who would not benefit from a ventilator.
- Going viral: 6 new findings about viruses
- The 12 deadliest viruses on Earth
- Top 10 mysterious diseases
Originally published on Live Science.
OFFER: Save 45% on 'How It Works' 'All About Space' and 'All About History'!
For a limited time, you can take out a digital subscription to any of our best-selling science magazines for just $2.38 per month, or 45% off the standard price for the first three months.

Nicoletta Lanese is the health channel editor at Live Science and was previously a news editor and staff writer at the site. She is a recipient of the 2026 AHCJ International Health Study Fellowship, with a project focused on antibiotic stewardship practices in Japan and the U.S. They hold a graduate certificate in science communication from UC Santa Cruz and degrees in neuroscience and dance from the University of Florida. Beyond Live Science, Lanese's work has appeared in The Scientist, Science News, the Mercury News, Mongabay and Stanford Medicine Magazine, among other outlets. Based in NYC, she also remains involved in dance and performs in local choreographers' work.
