Obesity is linked to 1 in 10 deaths from infection worldwide — and scientists are still learning why
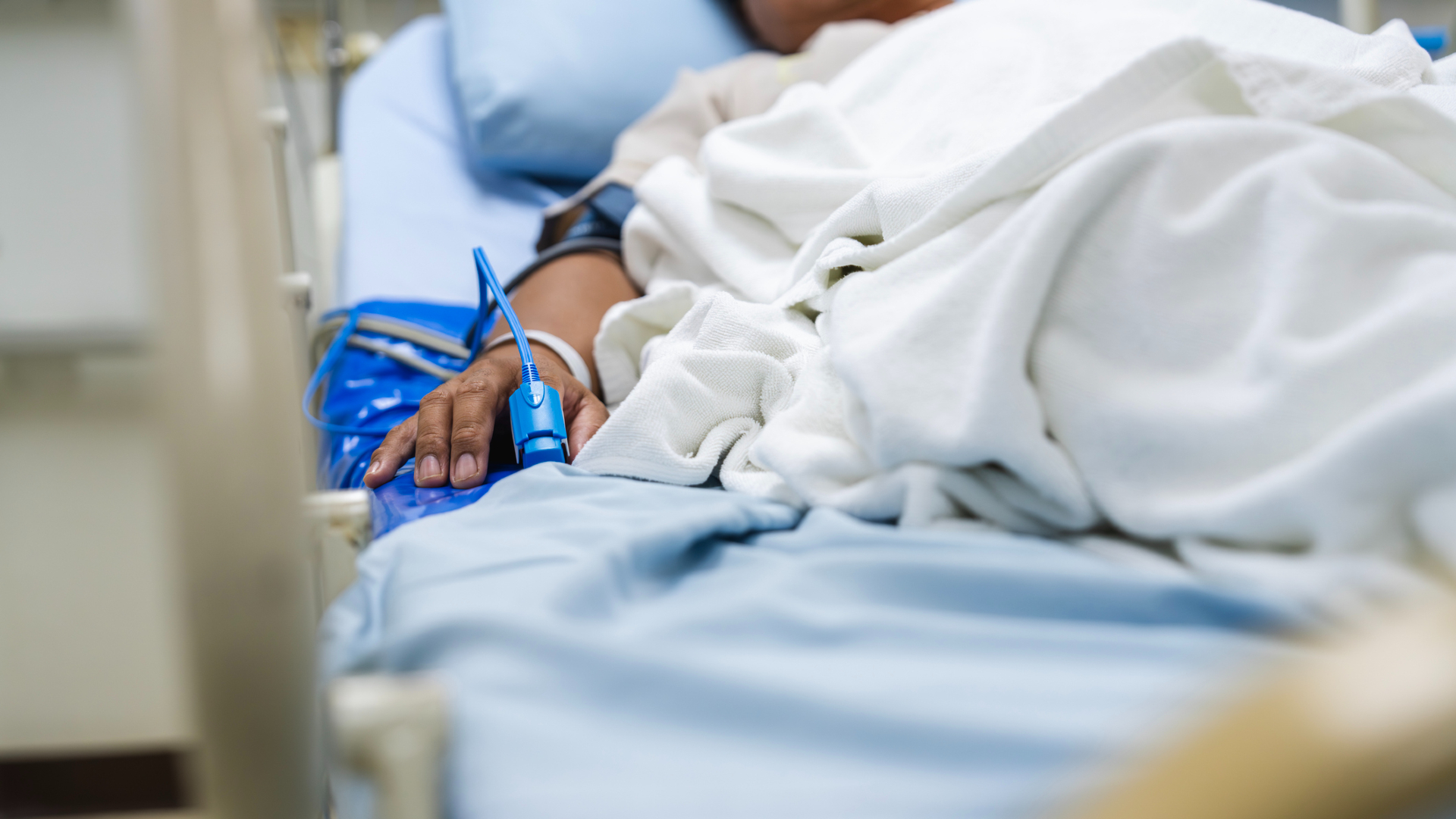
A new study finds that people with obesity are more likely to be hospitalized with or die from severe infections.
Get the world’s most fascinating discoveries delivered straight to your inbox.
You are now subscribed
Your newsletter sign-up was successful
Want to add more newsletters?
Join the club
Get full access to premium articles, exclusive features and a growing list of member rewards.
People with obesity are 70% more likely than those without the condition to be hospitalized with or die from severe infections, according to a new study of over half a million people.
The research found that 1 in 10 deaths attributed to infections worldwide were in people with obesity. This link persisted even in people with obesity who did not have metabolic syndrome or diabetes. And it showed up regardless of socioeconomic status or physical activity levels, researchers reported Feb. 9 in the journal The Lancet.
"People with obesity may find it harder to fight off infections," study senior author Mika Kivimäki, an epidemiologist at University College London, told Live Science. "Extra body fat can affect the immune system in several ways, including impairing lymphatic function, reducing lung function, and increasing long-term low-grade inflammation." The lymphatic system helps to maintain a balance of fluids in the body, as well as to train and ferry immune cells around.
An earlier study by different researchers, published in August 2025, found that using semaglutide — the active ingredient in drugs like Ozempic and Wegovy — reduced users' risk of severe infections by 10%. That finding might also hint that obesity and infection susceptibility are linked and, perhaps, suggest that the risk can be lowered.
The connection between obesity and the dangers of infection were made prominent during the COVID-19 pandemic, the new study found. In 2021, 15% of all infection hospitalizations and deaths were linked to obesity. That connection between obesity and COVID-19 severity motivated Kivimäki and his team to investigate whether the coronavirus was uniquely dangerous for people with obesity or whether the danger extended to all types of infections.
They turned to the UK Biobank, a large database of genetic sequencing and linked medical records from U.K. adults, as well as two similarly large studies from Finland: the Finnish Public Sector study and the Health and Social Support study. Together, these databases included over 540,000 people.
In the Finnish cohorts, participants self-reported their heights and weights, which could be used to calculate a body mass index (BMI). BMI is a rough estimate of body composition often used in large-scale population studies. The UK Biobank participants had more precise measurements done with a body-composition device, and they also had their waist circumferences measured. (Some researchers have argued that these types of metrics should replace BMI, as they're more useful for predicting health outcomes.)
Get the world’s most fascinating discoveries delivered straight to your inbox.
In the study, people with obesity included those with a BMI of 30 or higher; a waist circumference of over 40 inches (102 centimeters) in men or over 35 inches (88 cm) in women; or a waist-to-height ratio of 0.6 or more. Obesity was linked to a 70% greater chance of hospitalization with or death from infection, once adjusted for age and sex. This relationship held across different definitions of obesity and across all bacterial, viral, fungal and parasitic infections.
The results also showed that the greater the degree of obesity, the greater the risk.
People with a BMI of 30 to 34.9 had a 50% higher risk of infection, hospitalization or death, compared with people with BMIs under 30. But people with a BMI of 35 to 39.9 had twice the risk, and people with a BMI of 40 or above had three times the risk. In participants with follow-up measurements of obesity after their first baseline measurement, those who lost or gained weight saw their severe infection risk drop or rise in turn.
The nature of the study did not enable the researchers to prove causation or tease out precisely how obesity might raise these risks, Kivimäki said.
That said, evidence suggests that fat tissue and the immune system are enmeshed; the precursor cells that can turn into fat cells can act like immune cells, and some fat cells also excrete pro-inflammatory substances, said Nikhil Dhurandhar, a professor of nutritional sciences at Texas Tech University who was not involved in the new research.
It's a chronic disease. It's not a matter of willpower; it’s not a matter of discipline.
Nikhil Dhurandhar, Texas Tech University
Previous studies have found not only that weight can influence infection risk but also that certain pathogens are linked to the development of obesity, Dhurandhar told Live Science. The evidence that certain germs drive increases in fat has mostly been gathered in lab animals so far, while the human data is less conclusive.
Obesity can contribute to immune dysfunction that makes it harder for the body to fight infection, Dhurandhar added. Because of this dysfunction, people with obesity may not respond as well to vaccination as do people with weights categorized as overweight or normal, leaving them vulnerable. Obesity is tied to a lack of sensitivity to the hormone leptin, which helps regulate body weight and appetite and also has an immune-protective role, he said.
Dhurandhar said the 1 in 10 infection deaths linked to obesity in the study shouldn't be considered easily preventable by weight loss, because it is very difficult to lose weight and keep it off.
"Obesity is a disease," he said. "It's a chronic disease. It's not a matter of willpower; it’s not a matter of discipline."
However, the emergence of drugs like semaglutide, collectively known as GLP-1 agonists, may make weight loss easier for some people. The effect of these medications on risks from infection remains to be seen, Kivimäki said.
While trials hint that these medications reduce the risk, people taking these drugs also often lose muscle mass along with fat, which could have negative effects on the immune system. Muscle tissue provides an amino acid called glutamine that powers some immune cells, and also produces the anti-inflammatory compound interleukin-6.
"In our future research, we want to better understand why obesity raises the risk of severe infections," Kivimäki said, "and, importantly, what can be done to reduce that risk."
This article is for informational purposes only and is not meant to offer medical advice.
Nyberg, S. T., Frank, P., Ahmadi-Abhari, S., Pentti, J., Vahtera, J., Ervasti, J., Suominen, S. B., Strandberg, T. E., Sipilä, P. N., Meri, S., Sattar, N., & Kivimäki, M. (2026). Adult obesity and risk of severe infections: A multicohort study with Global Burden Estimates. The Lancet. https://doi.org/10.1016/s0140-6736(25)02474-2

Stephanie Pappas is a contributing writer for Live Science, covering topics ranging from geoscience to archaeology to the human brain and behavior. She was previously a senior writer for Live Science but is now a freelancer based in Denver, Colorado, and regularly contributes to Scientific American and The Monitor, the monthly magazine of the American Psychological Association. Stephanie received a bachelor's degree in psychology from the University of South Carolina and a graduate certificate in science communication from the University of California, Santa Cruz.
You must confirm your public display name before commenting
Please logout and then login again, you will then be prompted to enter your display name.

 Live Science Plus
Live Science Plus









