First 3-D Images Inside Human Arteries

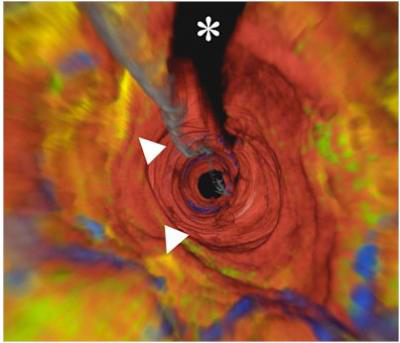
The walls that line human coronary arteries have been imaged for the first time in 3-D, a team of researchers says. Such images will allow cardiologists to see inside patients’ arteries more clearly and check for areas of inflammation or plaque deposits that can cause a heart attack. "This is the first human demonstration of a technique that has the potential to change how cardiologists look at coronary arteries," said researcher Dr. Gary Tearney, associate professor of pathology at Harvard Medical School. "The wealth of information that we can now obtain will undoubtedly improve our ability to understand coronary artery disease and may allow cardiologists to diagnose and treat plaque before it leads to serious problems." A research team at the Wellman Center for Photomedicine at Massachusetts General Hospital (MGH) developed an optical frequency-domain imaging (OFDI) device to get the 3-D views inside a human artery. OFDI can look at more than 1,000 points of artery tissue at a time (the previous imaging device made by the same investigators could only examine tissues one point at a time). As they physically probe through the coronary artery, wavelengths are emitted and reflected back, allowing rapid acquisition of the data required to create the detailed microscopic images. Not only are 3-D images now obtained in seconds, the increased speed also reduces signal interference from blood, which had plagued the MGH researchers’ first-generation technology. The current study, headed up by Tearney, enrolled three patients for whom OFDI provided detailed images along the length of their arteries — visualizing lipid or calcium deposits, and immune cells that could indicate inflammation — and dramatic "fly-through" views looking down the artery's interior. More detailed, cross-sectional images of narrowed vascular segments revealed features associated with the type of atherosclerotic plaques that are likely to rupture and cause a heart attack. Tearney and his colleagues note that these findings need to be duplicated in a larger group of patients, and the time required to process the "fly-through" images — currently several hours —needs to be reduced to provide the real-time information most useful for clinical applications. Combining OFDI with intravascular ultrasound might help with another of the technique's limitations, the inability to penetrate deep into tissues. The next step is to ensure this technique becomes a widely available commercial device to interventional cardiologists within a one- to two-year time frame. The study is detailed in the November 2008 issue of the journal JACC: Cardiovascular Imaging.
- Top 10 Amazing Facts About Your Heart
- Cancer Curing Blood
- How Heart Attacks Strike
Get the world’s most fascinating discoveries delivered straight to your inbox.
