Contaminated Cocaine: Docs Puzzled Before Realizing Patient's Habit
Get the world’s most fascinating discoveries delivered straight to your inbox.
You are now subscribed
Your newsletter sign-up was successful
Want to add more newsletters?
Join the club
Get full access to premium articles, exclusive features and a growing list of member rewards.
A woman who developed a rare type of skin lesion mystified doctors, until they realized she was using cocaine that was tainted with a very common contaminant, according to a recent report of her case.
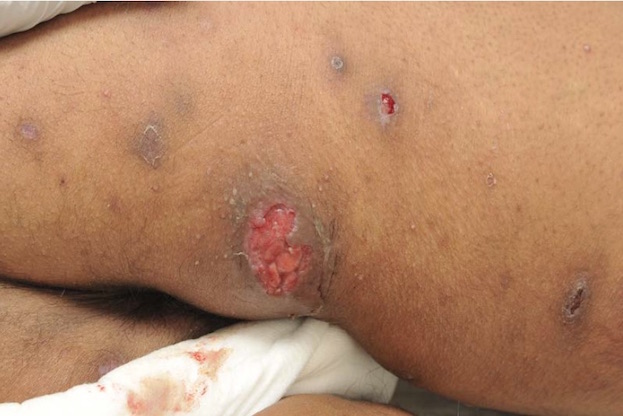
The 42-year-old woman came to the hospital suffering from joint and muscle pain, abdominal pain, and sores on her skin. Although she said she wasn't using drugs, a hair test eventually revealed that she had both cocaine and a drug called levamisole in her system. The skin sores turned out to be due to a condition called vasculitis, which levamisole can cause, according to the report, published Aug. 26 in the journal BMJ Case Reports.
Levamisole is veterinary drug used to treat parasite infections in animals, according to the Drug Enforcement Agency (DEA). A July 2015 report from the DEA found that 83 percent of cocaine seized in the United States is contaminated with the substance, Barbara Carreno, a DEA public affairs officer, told Live Science. [Trippy Tales: The History of 8 Hallucinogens]
Article continues belowThe doctors wrote the report of the woman's case in part to highlight the difficulty of diagnosing people who do not admit to using drugs, the authors said. The case also highlights the usefulness of hair testing for drugs, they said.
When the woman first came to the hospital, in the Netherlands in January 2013, the doctors initially suspected the inflammation in her joints was due to an infection — the woman had a history of urinary tract infections (UTIs), said Dr. Tjeerd van der Veer, a resident physician at Saint Francis Hospital in Rotterdam who treated the woman and co-authored the report of her case.
Sometimes, the bacteria that cause UTIs can lead to an immune response in the joints or eyes (a condition known as reactive arthritis), he told Live Science in an email.
However, as the patient's skin sores became more noticeable, the doctors realized that this was the wrong diagnosis, van der Veer said. A blood test suggested the lesions had a drug-related cause.
Get the world’s most fascinating discoveries delivered straight to your inbox.
However, it wasn't until the woman needed emergency surgery to fix a blockage in her intestine that she admitted to using cocaine.
"Even then, she admitted only to drug use in the past, and not recently," van der Veer said. "It was not until the hair test was positive that we were absolutely certain that recent exposure [to cocaine] had triggered her symptoms," he said.
The woman recovered by abstaining from cocaine; however, two months later, she relapsed and returned to the hospital with more joint pain. It was then, after the doctors ran blood tests and discovered that her kidneys had severe damage, that they were finally able to diagnose her with vasculitis from levamisole-contaminated cocaine, the doctors wrote in their report.
Van der Veer said he was struck "by the severity of the case, as well as the patient's unwillingness to cooperate by admitting to substance abuse," he said. "Maybe she could not overcome her fear for prosecution, or social stigma."
"It must be a sad situation for the patient to be in," he said.
It's "essential for patients to be honest with their health care providers, so they can deliver the right care," he said. Patients "should know that doctors' professional oath prohibits them from sharing patient information with the authorities, or anyone else, without the patient's permission," he added.
Van der Veer said that the patient in this case is currently doing well, but she still needs to take immunosuppressive drugs to treat her inflammation.
Levamisole-contaminated cocaine
Doctors in the United States — in particular, dermatologists and rheumatologists — are seeing more and more people who are affected by levamisole-contaminated cocaine, said Dr. Anthony Rossi, a dermatologist at Memorial Sloan Kettering Cancer Center in New York City, who was not involved with the case report.
Skin lesions like those of the woman in the case report are a classic symptom, Rossi said. They occur when blood vessels near the surface of the skin are severely damaged; without enough blood, the skin dies, he told Live Science.
It's unknown why levamisole is added to cocaine, but one possible explanation is that both drugs are similar in appearance — they're both white powders — so the addition may be intended to increase the weight of cocaine in a way that users won't notice, Rossi said. There's also speculation that levamisole may cause euphoria, he added.
Rossi agreed with van der Veer that it's important for patients to be up-front with doctors about their drug use. If patients keep using levamisole-tainted cocaine, the drug-induced vasculitis won't go away, he said. And some patients have ended up back in the hospital with more-serious problems because they haven't stopped, he said.
Patients shouldn't worry about admitting to drug use in the hospital, Rossi said. Doctors are not going to report them to the police.
"For the most part, people are pretty up-front [about drug use] when you ask them directly," Rossi said.
Rossi said that one of his patients became very proactive about levamisole-contaminated cocaine after she wound up in the hospital from using it. "She went into her community and told people about her story," he said. She even passed out flyers telling people to stop buying cocaine from the drug dealer who sold her the tainted product, he said.
"We're hoping it stops," Rossi added. "But we always try to tell our patients that we don't know what they're cutting cocaine with. If it's not levamisole, it could be something else."
Follow Live Science @livescience, Facebook & Google+. Originally published on Live Science.

 Live Science Plus
Live Science Plus









