'Biggest Risk' in Ebola Protection Is Gear Removal

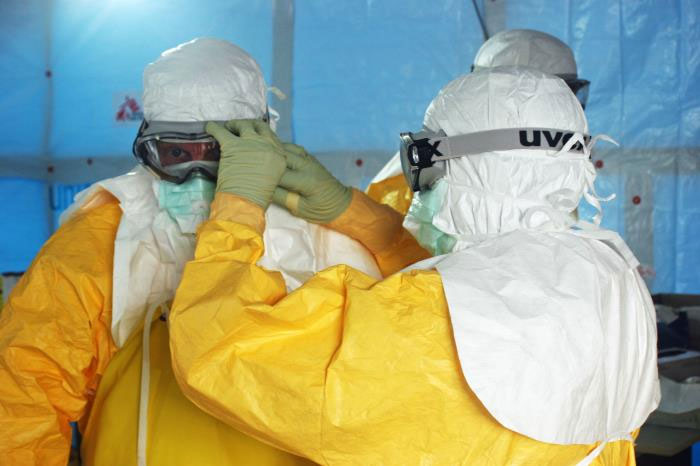
A "breach in protocol" is what led a nurse in Dallas to become the first person infected with Ebola in the United States, according to the Centers for Disease Control and Prevention. The nurse was involved in treating Ebola patient Thomas Eric Duncan, and her case has researchers trying to figure out exactly what went wrong with the safety protocols.
Ebola spreads through contact with an infected person's bodily fluids. Guidelines for health care workers recommend using personal protective equipment, including gloves, a fluid-resistant gown, goggles or a face shield and a face mask. They also recommend certain techniques — such as turning gloves inside out when removing them — that allow workers to safely remove the equipment after contact with an Ebola patient.
How contamination can happen
"The greatest risk overall is probably taking off or 'doffing' the equipment," said Dr. Sandro Cinti, an infectious-disease specialist at the University of Michigan Health System/VA Ann Arbor Healthcare System. [Infographic: Protective Gear For Ebola Patient Care]
In removing the equipment, health care workers should take care not to contaminate themselves or their clothing, Cinti said. Ebola can't get into the body through the skin itself, but having the virus on the skin means it could be transferred to the eyes or other mucous membranes, where it can enter the body, Cinti said. "Even a small breach can lead to an infection," he said.
In some situations, such as when there's a lot of blood or bodily fluids present, additional gear — such as double gloves, disposable shoe covers and leg coverings — may be needed, according to the CDC. Many hospitals are now looking at whether to expand the gear their workers wear to include disposable protective coveralls known as Tyvek suits, Cinti said.
When donning the equipment, "it's important to ensure the hands and wrists are covered completely, and the best way to do that is to have workers watch each other don the equipment," Cinti told Live Science.
Get the world’s most fascinating discoveries delivered straight to your inbox.
Equipment should be discarded after use or, if it's reusable, cleaned and disinfected, according to the CDC. Frequent hand washing is also critical for preventing infection. "This virus is easily killed by soap and the hand washes we use," Cinti said.
How did the Dallas nurse get Ebola?
It's not yet clear exactly how the Dallas nurse — who has been identified as Nina Pham, according to Dallas news station WFAA— acquired the virus. The woman had extensive contact with the infected patient after he was admitted to Texas Health Presbyterian Hospital on Sept. 28, CDC officials said.
She had been monitoring herself for symptoms, and had not been at work for two days before being admitted to the hospital and put into isolation. Officials are now monitoring other health care workers who also treated Duncan, according to the CDC.
The nurse's infection is worrisome, but should not be cause for panic, Cinti said.
People do not need to be concerned about going to a hospital if there's an Ebola patient there, and health care workers can avoid infection if proper precautions are taken, he said.
"Many health care workers have been exposed [to Ebola] in taking care of patients," Cinti said. Although some of them have become infected, it's "quite uncommon," even in Liberia, he said.
A nurse in Spain who recently became infected with Ebola after caring for two Spanish missionaries is showing signs of improvement, NBC News reported today.
The current Ebola outbreak in West Africa is the worst in history, and is responsible for the deaths of more than 4,000 people so far, according to the CDC.
Follow Tanya Lewis on Twitter and Google+. Follow us @livescience, Facebook & Google+. Original article on Live Science.


 Live Science Plus
Live Science Plus





