Get the world’s most fascinating discoveries delivered straight to your inbox.
You are now subscribed
Your newsletter sign-up was successful
Want to add more newsletters?
Join the club
Get full access to premium articles, exclusive features and a growing list of member rewards.
Your response to placebos, or dummy medicine, may depend on your genes, according to a new study.
People with a gene variant that codes for higher levels of the brain chemical dopamine respond better to placebos than those with the low-dopamine version.
The findings, reported online Oct. 23 in the journal PLoS One, could help researchers design medical studies that distinguish the placebo response from the underlying effect of a medicine — the real aim of drug trials.
Article continues below"This is a possible way to discern who is going to be a placebo responder or nonresponder in a clinical trial," said study co-author Kathryn Hall of Beth Israel Deaconess Medical Center in Brookline, Mass.
People report feeling better after receiving a placebo, such as a sugar pill or fake treatment, for conditions ranging from chronic pain to Parkinson's disease. But only some patients respond strongly, and there's no way to predict who will improve on a placebo.
A few studies have provided clues. Differences in versions of the catechol-O-methyltransferase (COMT) gene, which determines levels of dopamine in the brain's prefrontal cortex, are linked to differences in reward-seeking and pain perception. People with the high-dopamine version, or allele, of the COMT gene feel pain more acutely and seek rewards more strongly than those who have the low-dopamine copy.
That led the researchers to wonder whether the gene modulates placebo response.
Get the world’s most fascinating discoveries delivered straight to your inbox.
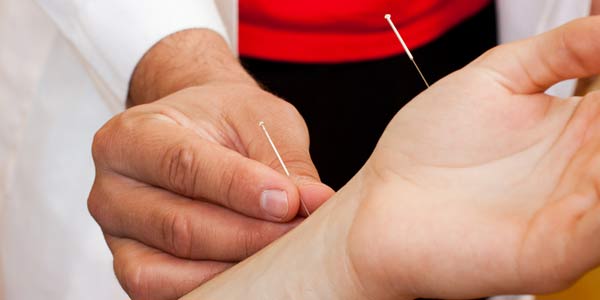
To find out, Hall and her colleagues analyzed DNA from 104 patients with irritable bowel syndrome who were randomized to one of three groups: One was told they were on the waiting list for treatment, another received a placebo in the form of seemingly real, curt acupuncture, and the third group received fake acupuncture from a caring, warm practitioner who looked patients in the eye, asked about their progress, and even touched them lightly, Hall told LiveScience.
Patients with the high-dopamine version of the gene felt slightly better after seeing the curt, all-business health-care provider that gave placebo acupuncture. But they were six times as likely to say their symptoms improved with a caring practitioner as those with the low-dopamine gene, who didn't improve much in any group.
The findings suggest that medical studies called clinical trials could identify treatment versus placebo effect by grouping patients by gene variant, Hall said. Knowing up front the level of placebo effect for a clinical trial could reduce the cost of the trial significantly by using fewer participants, for instance, she said.
People with the high-dopamine allele of the gene may do well on the placebo with the nurturing treatment because they are generally more attuned to their environments, said University of Michigan psychiatrist Jon-Kar Zubieta, who was not involved in the study.
"It speaks about an interaction between the environment and the gene," Zubieta said. "It's very possible that individuals with this allele are more able to process those positive environmental cues."
Follow LiveScience on Twitter @livescience. We're also on Facebook & Google+.

Tia is the editor-in-chief (premium) and was formerly managing editor and senior writer for Live Science. Her work has appeared in Scientific American, Wired.com, Science News and other outlets. She holds a master's degree in bioengineering from the University of Washington, a graduate certificate in science writing from UC Santa Cruz and a bachelor's degree in mechanical engineering from the University of Texas at Austin. Tia was part of a team at the Milwaukee Journal Sentinel that published the Empty Cradles series on preterm births, which won multiple awards, including the 2012 Casey Medal for Meritorious Journalism.

 Live Science Plus
Live Science Plus









