
Hospitals Hope to Kick Own Pollution Habits
Get the world’s most fascinating discoveries delivered straight to your inbox.
You are now subscribed
Your newsletter sign-up was successful
Want to add more newsletters?
Join the club
Get full access to premium articles, exclusive features and a growing list of member rewards.
When one thinks of the worst polluting industries — industrial farming, coal mining, toxic sludge manufacturing and the like — hospitals usually don't come to mind. Hospitals are supposed to help heal, not harm.
Yet hospitals are among the greediest consumers of natural resources, burning a sixth of the nation's energy; and they are the most prodigious producers of waste — not just those obscene paper gowns that reveal your tush and need to be trashed, but also mercury-containing solvents and phthalate-laced IV tubing and bags.
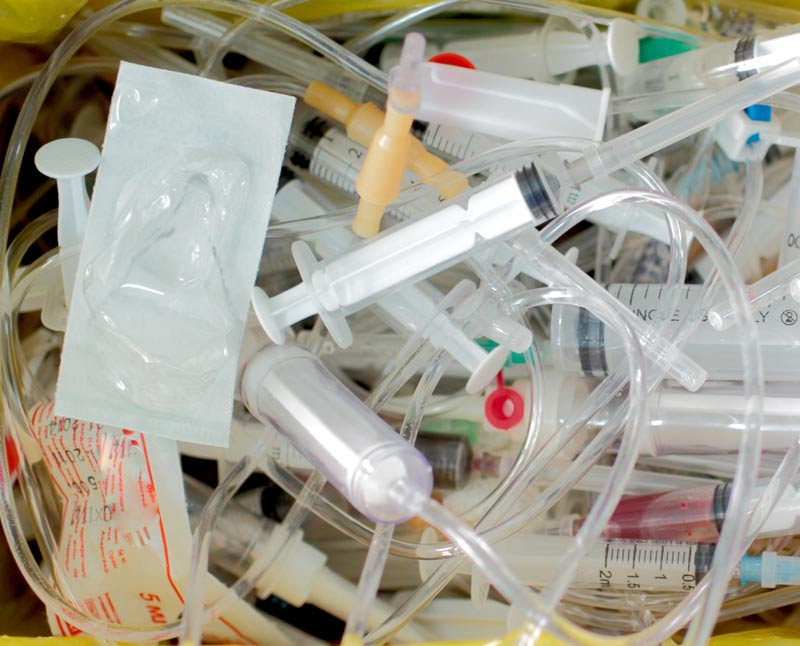
Hospitals generate on average more than 26 pounds of waste per patient bed per day, according to the health-care sector's own statistics, and most of this ultimately is burned or buried. This doesn't include the hundreds of thousands of electronic devices disposed of annually, many with dangerous compounds such as lead and cadmium.
Article continues belowNow the industry wants to green itself. Announced at a press conference on April 3 in Washington, D.C., 11 large U.S. health systems have formed the Healthier Hospitals Initiative (HHI) to dramatically reduce their energy consumption and waste production, as well as to serve more-nutritious food to patients and employees.
"If a hospital's fundamental commitment is to health, then we have a unique obligation to be leaders in making positive environmental change," said John Messervy, chair of the HHI and director of facilities for the Boston-based Partners HealthCare, the parent company of Massachusetts General Hospital and the Brigham and Women's Hospital. "It means that the Hippocratic oath of 'Do no harm' extends beyond the operating room [and] the exam rooms, out to the communities that we are a part of and that we serve." [Infographic: Renewable Energy Consumption in US]
Do no harm
The connection between environment and health is well established. Many birth defects and chronic diseases — cancers, circulatory disease, diabetes, obesity and asthma, together accounting for more than 75 percent of health-care costs — are linked to poor diets and polluted air and water.
Get the world’s most fascinating discoveries delivered straight to your inbox.
The irony of contributing to the very ailments they try to treat and cure has not been lost on hospitals. Each of the health-care systems participating in the initiative has been on its own road to better practices.
Partners HealthCare, for example, has overhauled airflow handlers and implemented programs to buy more energy-efficient products with a goal of reducing energy consumption 25 percent by 2014. Kaiser Permanente has a program to purchase environmentally preferable products, such as IV bags and computers with fewer harmful chemicals. Inova Health System has revamped its cafeterias to serve healthier food to its workers. Dignity Health has increased the number of reusable products it purchases. And so on.
What's new about the Healthier Hospitals Initiative is that, for the first time, these major health-care players are teaming up to share best practices, not only among themselves but freely with any hospital that wants the information. The HHI also is gathering data over the next three years to measure the impact of the program. [American's Best Hospitals, 2012]
Save some money, too
While going green is nice to tout, a major driver of the HHI is to reduce energy and waste-disposal costs.
Knox Singleton, CEO of the Virginia-based Inova Health System, spoke at the April 3 press briefing of a hospital's bottom line of saving money while maintaining quality. Purchasing reusable products, for example, has reduced waste by 4 million pounds and saves millions of dollars annually at Inova. Similarly, Kaiser Permanente's environmentally friendly purchasing program saves $26 million annually, the company representative said.
By combining forces, the members of the HHI — comprising more than 500 hospitals — hope to use their purchasing power to drive market forces and to reduce the costs of healthier and environmentally friendlier products, making it more affordable for any hospital to go green.
For all its potential strength, the HHI represents only about 10 percent of the nearly 5,800 U.S.-based hospitals and doesn't include the very largest systems, such as the Veterans Affairs hospitals. As such, HHI hopes to enlist more hospitals across the United States and Canada.
Christopher Wanjek is the author of the books "Bad Medicine" and "Food At Work." His column, Bad Medicine, appears regularly on LiveScience.

Christopher Wanjek is a Live Science contributor and a health and science writer. He is the author of three science books: Spacefarers (2020), Food at Work (2005) and Bad Medicine (2003). His "Food at Work" book and project, concerning workers' health, safety and productivity, was commissioned by the U.N.'s International Labor Organization. For Live Science, Christopher covers public health, nutrition and biology, and he has written extensively for The Washington Post and Sky & Telescope among others, as well as for the NASA Goddard Space Flight Center, where he was a senior writer. Christopher holds a Master of Health degree from Harvard School of Public Health and a degree in journalism from Temple University.
 Live Science Plus
Live Science Plus










