Respiratory system: Facts, function and diseases
Take a deep breath — here's how the respiratory system works.

Get the world’s most fascinating discoveries delivered straight to your inbox.
You are now subscribed
Your newsletter sign-up was successful
Want to add more newsletters?

Delivered Daily
Daily Newsletter
Sign up for the latest discoveries, groundbreaking research and fascinating breakthroughs that impact you and the wider world direct to your inbox.

Once a week
Life's Little Mysteries
Feed your curiosity with an exclusive mystery every week, solved with science and delivered direct to your inbox before it's seen anywhere else.

Once a week
How It Works
Sign up to our free science & technology newsletter for your weekly fix of fascinating articles, quick quizzes, amazing images, and more

Delivered daily
Space.com Newsletter
Breaking space news, the latest updates on rocket launches, skywatching events and more!

Once a month
Watch This Space
Sign up to our monthly entertainment newsletter to keep up with all our coverage of the latest sci-fi and space movies, tv shows, games and books.

Once a week
Night Sky This Week
Discover this week's must-see night sky events, moon phases, and stunning astrophotos. Sign up for our skywatching newsletter and explore the universe with us!
Join the club
Get full access to premium articles, exclusive features and a growing list of member rewards.
The human respiratory system is a network of organs responsible for taking in oxygen and expelling carbon dioxide. Its primary organs are the lungs, which carry out this exchange of gases as we breathe.
The lungs work with the circulatory system to pump oxygen-rich blood to all cells in the body. The blood then collects carbon dioxide and other waste products and transports them back to the lungs, where the waste products are pumped out of the body when we exhale, according to the American Lung Association.
The human body needs oxygen to sustain itself. After only about five minutes without oxygen, brain cells begin dying, according to the National Institute of Neurological Disorders and Stroke, which can lead to brain damage and ultimately death.
Related: Gasp! 11 surprising facts about the respiratory system
In humans, the average breathing, or respiratory rate, mostly depends on age. A newborn's normal breathing rate is about 40 to 60 times each minute and may slow to 30 to 40 times per minute when the baby is sleeping, according to Stanford Children's Health. The average resting respiratory rate for adults is 12 to 16 breaths per minute, and up to 40 to 60 breaths per minute during exercise, according to the European Respiratory Society.
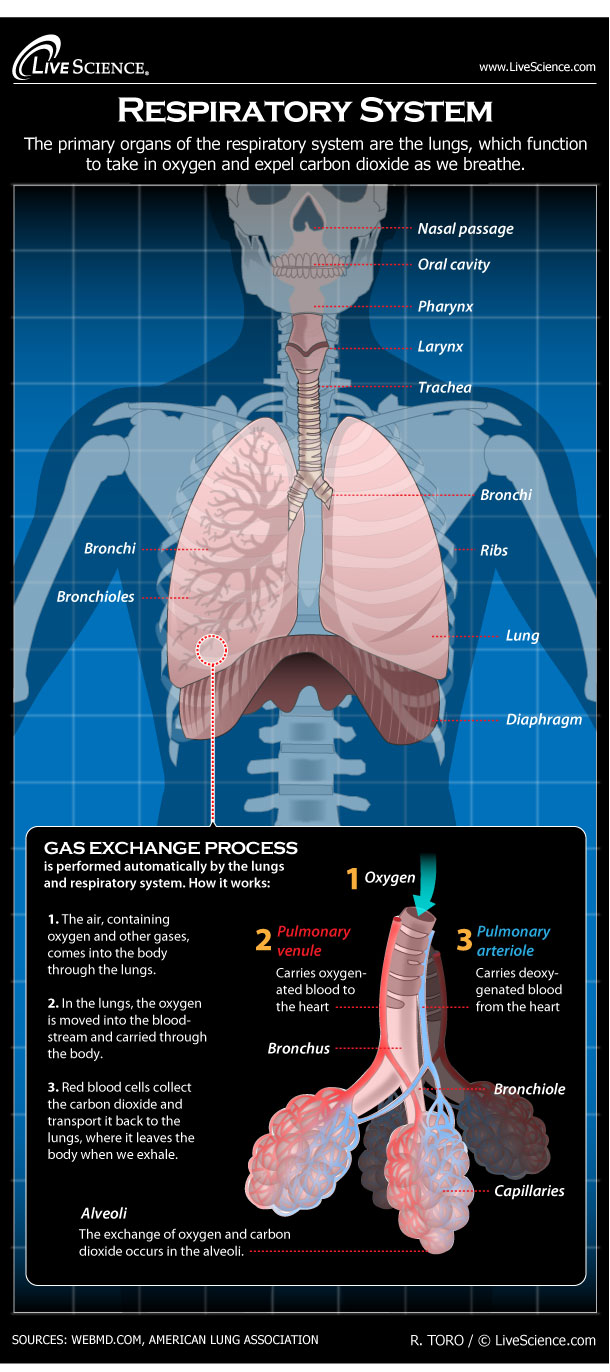
Parts of the respiratory system
There are many components to the respiratory system. They include:
- Nose
- Mouth
- Throat (pharynx)
- Voice box (larynx)
- Windpipe (trachea)
- Large airways (bronchi)
- Small airways (bronchioles)
- Lungs
- Diaphragm
As we breathe, oxygen enters the nose or mouth and passes the sinuses, which are hollow spaces in the skull that help regulate the temperature and humidity of the air we breathe.
Get the world’s most fascinating discoveries delivered straight to your inbox.
From the sinuses, air passes through the trachea, also called the windpipe, and into the bronchial tubes, which are the two tubes that carry air into each lung (each one is called a bronchus). The bronchial tubes are lined with tiny hairs called cilia that move back and forth, carrying mucus up and out. Mucus is a sticky fluid that collects dust, germs and other matter that has invaded the lungs and is what we expel when we sneeze and cough.
Related: Where does all my snot come from?
The bronchial tubes split up again to carry air into the lobes of each lung. The right lung has three lobes while the left lung has only two, to accommodate room for the heart, according to the American Lung Association. The lobes are filled with small, spongy sacs called alveoli, which is where the exchange of oxygen and carbon dioxide occurs.
The alveolar walls are extremely thin (about 0.2 micrometers) and are composed of a single layer of tissues called epithelial cells and tiny blood vessels called pulmonary capillaries. Blood in the capillaries picks up oxygen and drops off carbon dioxide. The oxygenated blood then makes its way to the pulmonary veins. These four veins, two from each lung, carry oxygen-rich blood to the left side of the heart, where it is pumped to all parts of the body. The carbon dioxide the blood left behind moves into the alveoli and gets expelled in our exhaled breath.
The diaphragm, a dome-shaped muscle at the bottom of the lungs, controls breathing and separates the chest cavity from the abdominal cavity. When air gets taken in, the diaphragm tightens and moves downward, making more space for the lungs to fill with air and expand, according to the National Heart, Lung and Blood Institute. During exhalation, the diaphragm expands and compresses the lungs, forcing air out.
Respiratory system diseases
Diseases and conditions of the respiratory system fall into two categories: Infections, such as influenza, bacterial pneumonia and enterovirus respiratory virus, and chronic diseases, such as asthma and chronic obstructive pulmonary disease (COPD).
Viral infections
Not much can be done for viral infections but to let them run their course, according to Dr. Neal Chaisson, who practices pulmonary medicine at the Cleveland Clinic. "Antibiotics are not effective in treating viruses and the best thing to do is just rest," he said.
For most healthy individuals, the most common respiratory ailment they may face is an infection, said Dr. Matthew Exline, a pulmonologist and critical care expert at The Ohio State University Wexner Medical Center. A cough is the first symptom, possibly accompanied by a fever.
Related:The gross science of a cough and a sneeze
"However, a cough can be a sign of chronic respiratory conditions such as asthma, chronic bronchitis or emphysema," he said. "In chronic lung disease, most respiratory diseases present with shortness of breath, initially with exertion, such as walking a significant distance or climbing several flights of stairs."
Asthma
Asthma is a chronic inflammation of the lung airways that causes coughing, wheezing, chest tightness or shortness of breath, according to Tonya Winders, president of the Allergy & Asthma Network. These signs and symptoms may be worse when a person is exposed to their triggers, which can include air pollution, tobacco smoke, factory fumes, cleaning solvents, infections, pollens, foods, cold air, exercise, chemicals and medications. Exercise can also induce asthma. More than 25 million people (or 1 in 13 adults and 1 in 12 children) in the United States have asthma, according to the Centers for Disease Control and Prevention (CDC).
For some people, asthma is a mild irritation, but for others it can be a life-threatening condition, according to the Mayo Clinic. Asthma cannot be cured, but its symptoms can be managed. Early identification and treatment can prevent long-term damage and stop asthma from getting worse over time.
Chronic obstructive pulmonary disease (COPD)
COPD is a chronic and progressive disease in which the air flow in and out of the lungs decreases, making it harder to breathe. COPD is a combination of chronic bronchitis (inflammation of the bronchial tubes) and emphysema (damaged alveoli), according to the Mayo Clinic. Smoking is the leading cause of COPD.
Over time, the airways of people with COPD become inflamed and thicken, making it harder to get rid of waste carbon dioxide, according to the American Lung Association. As the disease progresses, patients experience a shortness of breath, and it can limit activity. More than 16 million Americans are affected by COPD, according to the CDC. COPD has no cure, but it can be treated.
Lung cancer
Lung cancer is often associated with smoking, but the disease can affect nonsmokers as well. It is the second most common cancer for both men and women, outranked by prostate and breast cancers, respectively.
The American Cancer Society (ACS) estimates that in 2021, there will be about 235,760 new cases of lung cancer (119,100 in men and 116,660 in women) and around 131,880 deaths from lung cancer (69,410 in men and 62,470 in women) in the United States. However, the number of lung cancer deaths has been on a downward slope in recent years due to advances in treatment and early detection.Most people diagnosed with lung cancer are older than 65, and the average age of people diagnosed with lung cancer is 70, according to ACS.
There are two different types of lung cancer, which is cancer that originates in the lungs as opposed to cancer that spreads to the lungs –– small cell lung cancer and non-small cell lung cancer, according to the Mayo Clinic. Small cell lung cancer is most commonly found in heavy smokers, and is less common than non-small cell lung cancer.
The main symptoms for lung cancer are shortness of breath, pain, coughing up blood, and fluid in the lungs. A doctor diagnoses lung cancer by performing imaging tests, such as a CT scan; testing coughed-up sputum; and a lung biopsy.
Treatment is based on the extent of the lung cancer, and whether it has spread to other parts of the body. Treatments range from surgery, chemotherapy and radiation therapy, through to palliative care.
Additional resources
- Read more about the anatomy of the respiratory system from the University of Rochester Medical Center.
- Watch "Meet the Lungs," from the Khan Academy.
- Check out this useful diagram of the respiratory system, from The Lung Association.
This article was updated on July 16, 2021 by Live Science Contributor Sarah Wild.
Kim Ann Zimmermann is a contributor to Live Science and sister site Space.com, writing mainly evergreen reference articles that provide background on myriad scientific topics, from astronauts to climate, and from culture to medicine. Her work can also be found in Business News Daily and KM World. She holds a bachelor’s degree in communications from Glassboro State College (now known as Rowan University) in New Jersey.
 Live Science Plus
Live Science Plus