What Is Flesh-Eating Bacteria?

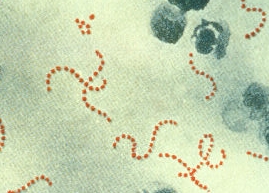
The term "flesh-eating bacteria" refers to several different types of bacteria that can cause necrotizing fasciitis. Necrotizing fasciitis is a severe bacterial infection that destroys muscles, skin and underlying tissue. The word "necrotizing" refers to something that causes body tissue to die.
Necrotizing fasciitis can start as a cut on the leg and end in amputation and, though rare, it has a high mortality rate, according to the Mayo Clinic. While flesh-eating bacteria sounds like the makings of a horror movie, it is actually very preventable.
Causes
Streptococcus pyogenes, the same pathogen that causes strep throat, is usually what is referred to as flesh-eating bacteria, according to the National Institutes of Health. It brings on a particularly severe and often deadly form of the disease when it infects the fascia, or connective tissue that surrounds muscles, blood vessels and nerves. But other bacteria can cause necrotizing fasciitis.
Article continues below"Other bacteria that are known to be flesh-eating are Staphylococcus aureus, E. coli and Klebsiella, members of the genus Clostridium and Aeromonas hydrophila," said Dr. Mary B. Farone, a professor at the biology department of Middle Tennessee State University. "These infections can be monomicrobial (one bacterium) such as with Streptococcus pyogenes (also known as Group A Streptococcus) or polymicrobial (many bacteria)."Group A strep is the most common cause of necrotizing fasciitis, according to the Centers for Disease Control and Prevention (CDC).
Soft tissue infection develops when the bacteria enters the body, usually through an untreated cut or scrape. Once inside the body, the bacteria will grow and release toxins. These toxins kill body tissue and affect blood flow to the area. As the tissue dies, the bacteria are rapidly spread throughout the body by the bloodstream.
In the case of S. pyogenes, the bacteria produce a toxin known as a superantigen, which activates white blood cells called T-cells, causing an overproduction of proteins called cytokines. These wreak havoc on cells.
For most people shouldn't be afraid of flesh-eating bacteria. "If you have a healthy immune system and practice proper wound care, you should not be worried," said Farone. "These types of infections are rare. Being aware of these unfortunate outcomes and recognizing the symptoms are important to realizing when medical attention is required."
Get the world’s most fascinating discoveries delivered straight to your inbox.
Those who are particularly at risk are those who have a lowered immune system or lower ability to heal, such as those with kidney disease, diabetes or cancer.
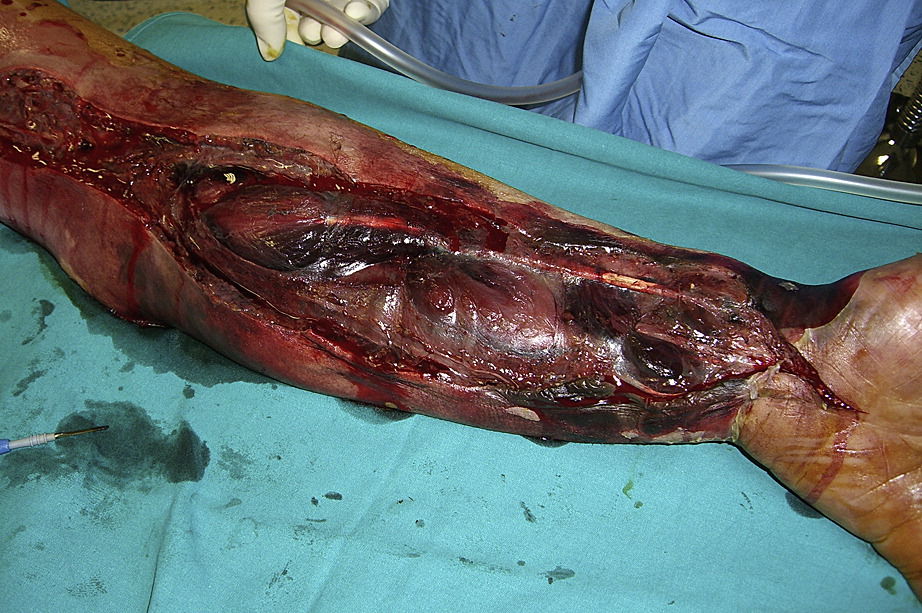
Symptoms
Symptoms of flesh-eating bacteria can come within hours of an injury. According to the CDC they include:
- Soreness that feels like a pulled muscle
- Warm skin
- Red or purplish areas of swelling that spread rapidly
- Ulcers, blisters or black spots on the skin
- Severe pain
- Fever
- Chills
- Fatigue
- Vomiting
Diagnosis & treatment
Immediate treatment of necrotizing fasciitis is needed to prevent death. Sometimes a medical professional will be able to make a diagnosis by looking at the wound. Other times tests such as a CT scan, blood tests or a skin tissue biopsy will be ordered.
Treatment includes powerful, broad-spectrum antibiotics given immediately through a vein, surgery to drain the sore and remove dead tissue, and, in some cases, a dose of antibodies called donor immunoglobulins to help fight the infection. Hyperbaric oxygen therapy and skin grafts may also be needed.
If the infection has caused a severe amount of tissue death, medical professionals may opt to amputate an infected limb, according to the CDC. Amputation may also be required to prevent the disease from spreading.
Prevention
The best way to prevent a flesh-eating bacterial infection is to ensure that wounds are properly cared for. For small wounds, clean the wound and keep it covered with clean, dry bandages until it's healed. Also, avoid using whirlpools, hot tubs and swimming pools until any infection is healed. "Deep wounds need medical attention and antibiotics should be given to prevent the spread of bacteria through the layers of the skin," said Farone.
Additional resources
