Polio Vaccines May Not Always Work
Get the world’s most fascinating discoveries delivered straight to your inbox.
You are now subscribed
Your newsletter sign-up was successful
Want to add more newsletters?
Join the club
Get full access to premium articles, exclusive features and a growing list of member rewards.
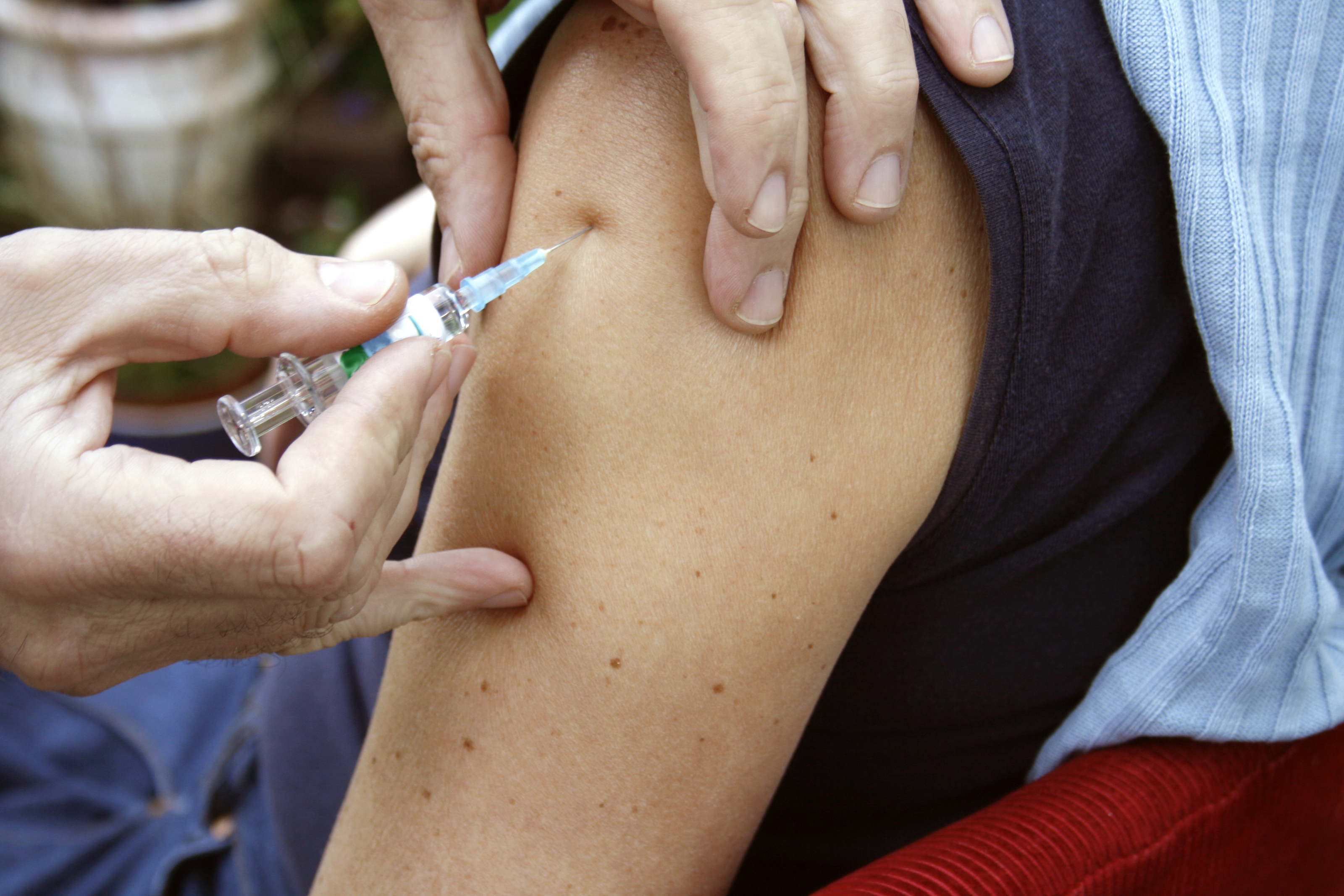
The standard polio vaccine may not always work, as vaccinations didn't prevent polio in people in the Republic of the Congo during an outbreak there in 2010, a new study shows.
The reason the vaccine didn't always work during the outbreak was that the virus had mutated, the researchers said.
In the study, the researchers looked at blood samples taken from 75 people who were vaccinated against polio. Of these people, 24 died from polio in the outbreak, and 51 others live in Bonn, Germany, and did not have polio. The researchers found that about one in five of the participants did not have an antibody response to poliovirus that would have prevented them from getting sick.
Article continues belowThe findings show that researchers need to identify mutant virus strains and generate more potent polio vaccinations, said study leader Dr. Jan Felix Drexler, a virologist at the University of Bonn Medical Centre in Germany. "On one side, we have mutant viruses that are out there, and on the vaccine side, we need to continue generating vaccines and thinking about new ones," Drexler told Live Science.
The 2010 outbreak had a fatality rate of 47 percent, and previous studies have suggested that this unusually high rate of deaths occurred because people were not vaccinated, Drexler said. But the new study suggests that the lack of immune-system response in people who were vaccinated also played a role. [7 Devastating Infectious Diseases]
In the study, the researchers isolated the virus from the blood of a patient who died from polio. They found that the virus that killed the person was a mutant strain, meaning it was genetically different from other polioviruses seen before.
The researchers found that in 15 percent of the blood samples they looked at from medical students and 29 percent of the samples from hospital patients in Bonn, the antibodies normally produced in response to infection were unable to block the mutant virus.
Get the world’s most fascinating discoveries delivered straight to your inbox.
"The response to the mutant virus that caused the Congo virus is much, much weaker than against all other studied viruses," Drexler said. "That's where it got scary, because it means variant [mutant] viruses exist. Viruses can actually escape the human-induced antibodies, so some people may be essentially unprotected from variant viruses."
In addition, people must keep getting vaccinated to prevent future outbreaks, Drexler said. "We proved the mutant viruses are out there, but if we provide a robust population immunity, we can still stop [the viruses] from causing disease," Drexler said.
But researchers also need to create better vaccines, he said. "We are maybe not as close to [polio] eradication as we would like to be."
Raul Andino, a microbiology professor at the University of California, San Francisco, agreed with the new study's conclusions, but he noted that it doesn't provide a complete picture of the 2010 outbreak. "This finding probably represents a very important call to keep high vaccine coverage in all countries, and to keep an eye on the possibility that the virus could evolve away from the vaccine but by no means is a definitive demonstration that is what happened in Republic of Congo in 2010," Andino told Live Science in an email.
Drexler said the study has limitations. For instance, the research team had no access to the clinical histories of the patients who died of polio in the Congo outbreak, making it hard to tell how they had reacted to the vaccine. The findings must also be replicated, he said.
The next steps would be to repeat the experiments with new versions of the virus, and to keep an eye out for patients who might be getting sick with mutant viruses before major outbreaks occur, he said.
The study was published Aug. 18 in the journal PLOS ONE.
Follow Jillian Rose Lim @jillroselim & Google+. Follow us @livescience, Facebook & Google+. Original article on Live Science.
 Live Science Plus
Live Science Plus










