Face Transplants Should Be Offered to More Patients, Doctors Say

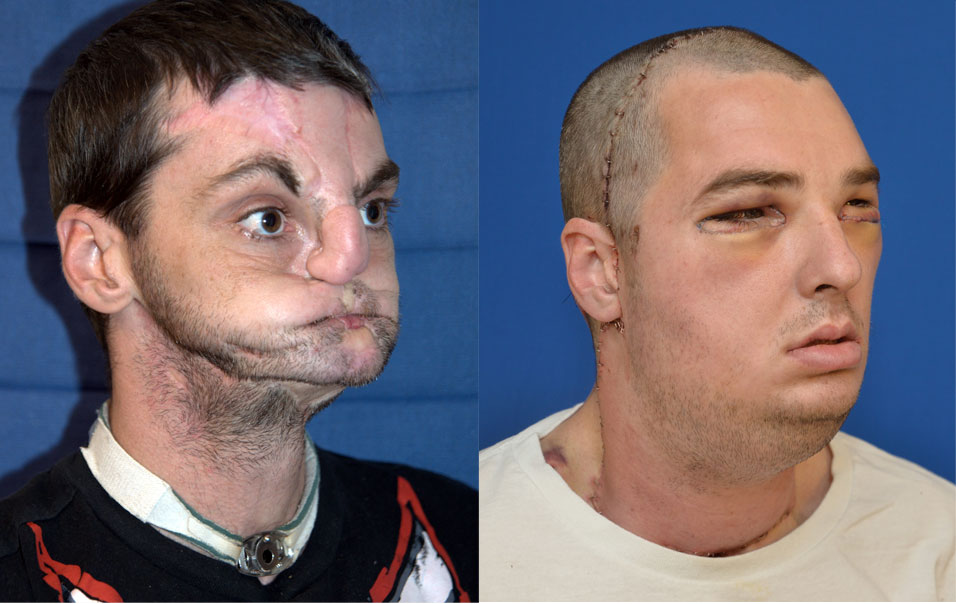
Face transplants promise dramatic results for people left disfigured after animal attacks, fires, shootings and other grisly incidents, researchers say.
But the procedure is still in its infancy. It can cost well over $300,000 and is not covered by insurance companies. The surgery raises ethical dilemmas, too, because it's not life-saving like a liver transplant. Just 28 known full or partial face transplants have been performed worldwide since 2005, when doctors restored a French woman's nose and lips that had been chewed off by her pet Labrador.
In a new review of those 28 cases, a group of plastic and reconstructive surgeons says face transplants should be offered to more patients, as long as they meet certain criteria, because the operation is relatively safe and increasingly feasible. [The 9 Most Interesting Transplants]
For any kind of transplant, one of the greatest risks is rejection. To prevent the immune system from attacking new body parts, transplant patients often have to be put on an intense regimen of immunosuppressive drugs, which in turn leaves them more susceptible to illness and infections.
Of the 22 men and six women whose face transplants were reviewed, all experienced complications with infections, and there was at least one episode of transplant rejection, the doctors said. However, none chronically rejected their new organs or tissues.
Of the three patients who died since their transplants, the cause of death in each case was not directly linked to the surgery, but rather due to an unrelated infection or cancer, the doctors reported in The Lancet on April 27.
Most of the people who received face transplants, especially the seven patients in the United States, are "thriving" — speaking, chewing and rekindling their social lives, the researchers said.
Get the world’s most fascinating discoveries delivered straight to your inbox.
"By far, the overriding factor in the success of face transplantation has been in selecting patients most likely to benefit from and succeed through what can best be described as the most complex of medical-surgical procedures," Dr. Eduardo Rodriguez, chair of the Department of Plastic Surgery at NYU Langone Medical Center, said in a statement. "This is a life-changing treatment that can take years to prepare for, and one that hopefully endures for the rest of the patient's life."
Rodriguez was part of the team that performed an extensive face transplant in 2012 on Richard Lee Norris, a then-37-year-old man from Hillsville, Va., who was mutilated in a gun accident nearly two decades ago. By 18 months after his surgery, Norris reported an improvement in the quality of his life, his body image and symptoms of depression, Rodriguez and colleagues wrote.
"People who volunteer to undergo this procedure do so for very serious health and psychological reasons," Dr. Rodriguez said in a statement. "It goes far deeper than looks. People willing to undergo facial transplantation are highly motivated to do so. Without facial transplantation as an option, many of these people would be at serious risk for severe depression, even potential suicide."
Rodriguez and colleagues noted that because a face transplant isn't a life-saving procedure, the surgery has been criticized for exposing otherwise healthy people to potentially lifelong risks of immunosuppression, which can include infections, cancer, graft loss and death. The doctors said ethical dilemmas can be avoided as long as the right patients are selected for surgery.
The best candidates for a face transplant will be patients who fully understand the consequences of immunosuppression and will be motivated and committed to complying with the intense post-operative rehab, psychological treatment and immunosuppression protocols, the doctors wrote. What's more, these patients should have a strong social support system — friends and family who can help them to address challenges, ranging from media exposure to body image adaptation.
Follow Megan Gannon on Twitter and Google+. Follow us @livescience, Facebook & Google+. Original article on Live Science.


 Live Science Plus
Live Science Plus





