Discovery Offers Hope to Chronic Pain Sufferers


More than 70 percent of people with chronic pain have lived with it for more than three years, according to the American Chronic Pain Association. A third of those have suffered pain for more than a decade.
Now, scientists have discovered the molecular pathway for chronic pain in rats, offering hope to the nearly one in six Americans who endure aches, burning sensations and throbbing long after their injuries have healed.
The pathway was described previously in the California sea slug, which is an invertebrate, but it has been recently confirmed in rats by Richard Ambron and Ying-Ju Sung of Columbia University Medical Center (CUMC) and a colleague.
Rats have a nervous system that more closely resembles our own and they are often used as model organisms for studies of pain in humans.
"A finding in invertebrates does not necessarily translate into a result that is also true for vertebrates," Ambron told LiveScience. "This is a major advance because we were able to show that the pain pathway was conserved in rats."
Pain research
The worldwide painkiller market was worth $50 billion in 2005, but current medications for chronic pain, meaning pain that lasts weeks, months and even years, leave much to be desired. Companies have shied away from developing new pain drugs in part due to troubles with Vioxx and Celebrex—called COX-2 selective non-steroidal anti-inflammatory drugs. Vioxx and Celebrex were reported a couple years ago to increase the risk of heart disease and stroke as side effects.
Get the world’s most fascinating discoveries delivered straight to your inbox.
Aside from the problems with the COX-2 drugs, acetaminophen is little help, and morphine and other narcotics are addictive and sedate the patient.
The uncertainty around COX-2 drugs has left people in chronic pain with few choices, Ambron said.
"Pain does not receive anywhere near the recognition it should," he said. "Chronic pain is debilitating and greatly diminishes the quality of life, but it has yet to generate the funding that is needed to understand its biological and molecular basis. There is a huge population out there that is suffering, and they can't get relief. A recent survey showed that only 15 percent of those people with chronic, unremittent pain receive treatment. The others seek alternatives, such as acupuncture and cognitive behavioral therapy because the drugs don't work."
Based on the new pathway, Ambron and his CUMC colleagues have applied for a patent to develop a new class of drugs that interfere with the newly reported pathway by "turning off" an enzyme that acts like an on-off switch in the neurons that signal chronic pain.
The chronic pain pathway
In studies with 15 rats, Ambron and his colleagues found that inflammation or injury sets off a cascade of chemical events that causes the activation of an enzyme called protein kinase G (PKG) early on. The PKG causes nerve cells, or neurons, to become hyperexcitable, which means that signals are sent to the pain centers in the brain. As long as the PKG is active, pain persists. Turning off PKG alleviates the pain, making PKG a promising target for drug therapy.
Most prior work on chronic pain has focused on what is called second-order neural processing, which occurs in the central nervous system (the brain and spinal cord). However, drugs that target the neurons involved in this processing must overcome the chemical blood-brain barrier, and this is often difficult.
The finding by Sung, Ambron and David Chiu at New York University Medical Center is important because the PKG pathway is located in the peripheral nervous system (the nerves and neurons in places like the skin that deliver signals to the central nervous system) and is therefore readily accessible to drugs.
Ambron's research was funded in part by aaiPharma, a company that was interested in developing pain drugs but has since been dissolved.
- The Pain Truth: How and Why We Hurt
- Surprising Source of Chronic Pain Discovered
- Yeeowww! Prehistoric Dentists Used Stone Drills
- Chronic Pain Shrinks People's Brains
- Boiling Lobsters Likely Feel No Pain
- Ouch! Why Women Feel More Pain
- New Device Zaps Migraines
Painful Facts
How pain hurts Americans:
- 1 in 6 suffers from arthritis.
- More than 26 million between the ages of 20 and 64 have frequent back pain.
- More than 25 million have migraines.
- Pain costs an estimated $100 billion each year.
SOURCE: American Pain Foundation
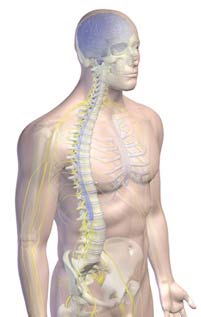
The central nervous system (brain and spinal cord) is colored blue, and the peripheral nervous system (major peripheral nerves) are yellow. Shown are the brain inside the cranium, spinal cord inside the vertebral column, and the spinal nerves coming out of the intervertebral foramen.
Image courtesty 3DScience.com
The Pain Truth

Robin Lloyd was a senior editor at Space.com and Live Science from 2007 to 2009. She holds a B.A. degree in sociology from Smith College and a Ph.D. and M.A. degree in sociology from the University of California at Santa Barbara. She is currently a freelance science writer based in New York City and a contributing editor at Scientific American, as well as an adjunct professor at New York University's Science, Health and Environmental Reporting Program.

 Live Science Plus
Live Science Plus





