The Pain Truth: How and Why We Hurt

Some 50 million U.S. residents live with chronic pain, experts estimate. Pain forces an estimated 36 million of them to miss work every year and results in roughly 70 million doctor visits.
Yet scientists know very little about how pain works. They can't even agree on a definition.
They do agree it's a huge problem.
"Pain is a silent epidemic in the United States," says Kathryn Weiner, director of the American Academy of Pain Management.
Real numbers are hard to get at. A Gallup Poll done in 2000 found that 80 percent of American believe pain is part of getting old, and 64 percent said they'd see a doctor only if their pain became unbearable. More than a quarter of them figured there is no solution to their pain.
"Pain has significant impact on the pain sufferer and their family," Weiner says. Pain and its treatment "represents a major problem confronting our modern culture."
What is pain?
Get the world’s most fascinating discoveries delivered straight to your inbox.
If you suffer chronic pain, you'll probably find little solace in the fact that doctors and scientists don't understand it very well, and that just popping an aspirin is clearly far form a cure-all.
In fact experts can't even agree on what pain is.
"Pain is complex and defies our ability to establish a clear definition," Weiner says. "Pain is far more than neural transmission and sensory transduction. Pain is a complex mixture of emotions, culture, experience, spirit and sensation."
The American Academy of Pain Medicine isn't much help either. In its online FAQ, under the heading "What is pain?" you'll find this answer: "It is an unpleasant sensation and emotional response to that sensation."
There are several ways to define pain, however, and knowing which you have is important for considering how to treat it.
What we know
One way to divide pain (and perhaps conquer it) is to distinguish between acute and chronic, explains Sally Lawson, a professor of physiology at the University of Bristol in the UK.
Acute pain is what you get when you hit your thumb with a hammer, should you choose to do so. You can also achieve it with a twisted knee or a burn.
Chronic pain is long-term, continuous and far more frustrating. It can result from physical injury, viral infections of the nerve, or arthritic damage to joints and degeneration of bones, Lawson writes.
Scientists also distinguish between evoked pain (use the hammer on your thumb to demonstrate this type) and the spontaneous variety, for which there is no obvious external cause.
One type of chronic pain, called neuropathic, results from damaged nerves rather than the original injury. However, recent research by Lawson and a colleague suggests this pain may sometimes be transmitted by the undamaged nerves.
Not so simple
If it were all that simple, pain probably wouldn't hurt so much. But there's a lot more to it.
"Acute pain is usually evoked, but chronic pain can be evoked or spontaneous," Lawson explains. "Chronic pain often includes spontaneous pain, and spontaneous pain may be ongoing, unpleasant, often burning pain, or it can be an intermittent sharp stabbing or shooting pain, or both."
And that's just the half of it. There are other ways to define and discuss pain.
Meanwhile, scientists are getting closer to understanding the nature of pain by analyzing the types of nerve fibers involved in its transmission, how the signals get to your brain, and how the information is processed.
Nerves in the body serve to warn us when something is acutely dangerous, such as a hot surface, or when our body needs rest or repair. And yes, sometimes those nerves just seem to annoy.
Thousands of pain-sensing nerve endings can be packed into tiny spaces in your fingers, between the vertebrae of your back, and just about everywhere else.
There are several types of nerves that sense cold, warmth pressure, pain and more. The nerves that sense and transmit pain are called nociceptors (pronounced no-sih-SEP-turs). There are more in your fingers and toes, where injury is more likely, than in other parts of your body.
Nociceptors transmit electrical signals to your spinal column. When the cause of pain gets stronger, they fire more rapidly and intensely.
Thinking about it
In the spinal cord, the electrical pain signals trigger release of chemicals called neurotransmitters, which activate other nerve cells that process and transmit the information to the brain.
Important decisions occur in the spinal column: Acute pain like that from touching a hot surface raises a red flag and is routed to the brain immediately. Weaker messages are given less priority, so that you don't overreact to a minor scrape.
They type of pain you feel—acute or chronic—probably depends in part on the type of nociceptive fiber that is sends the initial signal, according to Lawson. "The larger fibers convey electrical impulses very rapidly to the brain, and are thought to cause sharp pricking pain, while the very fine fibers cause ongoing burning, very unpleasant sometimes called ‘unbearable' pain" because of its persistence.
Pain signals are process in the brain's thalamus, a sort of switching station. The thalamus forwards the message to three places:
- Somatosensory cortex (physical sensation)
- Limbic system (emotional feeling)
- Frontal cortex (limbic system)
The brain can do more than just initiate a quick retreat from the source of pain. It might signal nerve cells to release painkillers, such as endorphins.
Chronic pain, for which there is often no obvious source, if often more complex and poorly understood. It's generally defined as pain that lasts more than six months.
Mayo Clinic researchers say chronic pain, which might result from inflammation, can be amplified and distorted like music turned up beyond a speaker's capability, causing pain out of proportion to the source. Beyond that, however, they and other researchers admit many types of chronic pain are poorly understood.
What to do
Only specialists can give proper advice for individual conditions. But all agree that curing chronic pain requires a proactive approach on the part of the sufferer.
Educate yourself, they say, and seek advice of multiple experts. And don't rely on outdated advice.
Many people figure pills are the best way to alleviate chronic pain. But exercise can be an important aspect to treatment.
"Years ago, people who were in pain were told to rest," says Edward Laskowski, a rehabilitation specialist and co-director of the Sports Medicine Center at the Mayo Clinic in Rochester, Minn. "But now we know the exact opposite is true. When you rest, you become deconditioned—which may actually contribute to chronic pain."
Painful Facts
How pain hurts Americans:
- 1 in 6 suffers from arthritis.
- More than 26 million between the ages of 20 and 64 have frequent back pain.
- More than 25 million have migraines.
- Pain costs an estimated $100 billion each year.
SOURCE: American Pain Foundation
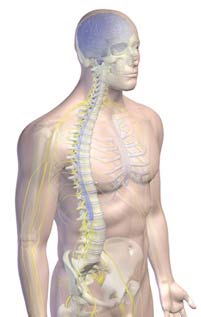
Image courtesty 3DScience.com
Getting Relief
If your family doctor can't solve your pain problem, you might consider a large hospital with a pain center. That can be intimidating. So when working with a specialist, keep your regular doctor informed of treatments and progress. And look for a specialist who:
- Is knowledgeable about chronic pain
- Listens well
- Makes you feel at ease
- Encourages you to ask questions
- Seems honest and trustworthy
- Allows you to disagree
- Is willing to talk with your family or friends
- Has a positive attitude toward life and your condition
SOURCE: Mayo Clinic
Learn More
The path to pain reduction starts with education, experts say. While extraordinary claims and unproven methods can fill a typical Internet search, here are some reliable sources:
- The Mayo Clinic Pain Center
- The American Chronic Pain Association
- Medline, from the National Institutes of Health
- The American Pain Foundation

Robert is an independent health and science journalist and writer based in Phoenix, Arizona. He is a former editor-in-chief of Live Science with over 20 years of experience as a reporter and editor. He has worked on websites such as Space.com and Tom's Guide, and is a contributor on Medium, covering how we age and how to optimize the mind and body through time. He has a journalism degree from Humboldt State University in California.

 Live Science Plus
Live Science Plus





