Life Spans May Be Shrinking for Some American Women

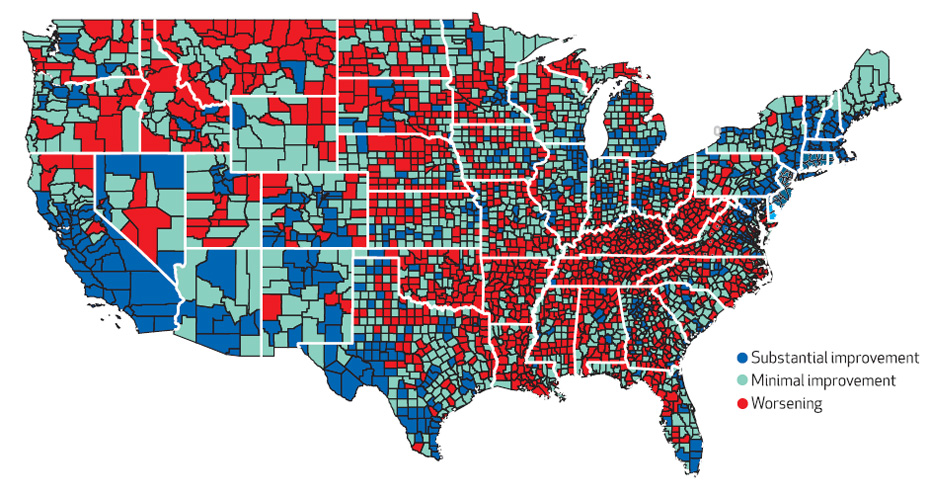
The life expectancy for some American women seems to be on the decline, especially in rural areas in the South and the West, new research suggests.
The mortality rates for women age 75 and younger in 42.8 percent of counties in the United States worsened between 1992 and 2006, while the same was true for men in just 3.4 percent of counties over the same period, the study shows.
"We decided to look at the change in health outcomes over time, and were actually shocked to see that female mortality rates were worsening in more than 42 percent of counties," study researcher David Kindig, professor emeritus of population health sciences at the University of Wisconsin, said in a statement.
American women have generally enjoyed a longer life expectancy than men, but the gap has been narrowing since its peak in 1979. In 2011, the life expectancy for an American female was 81.1 years compared with 76.3 years for men, according to the most recent available data from the Centers for Disease Control and Prevention (CDC).
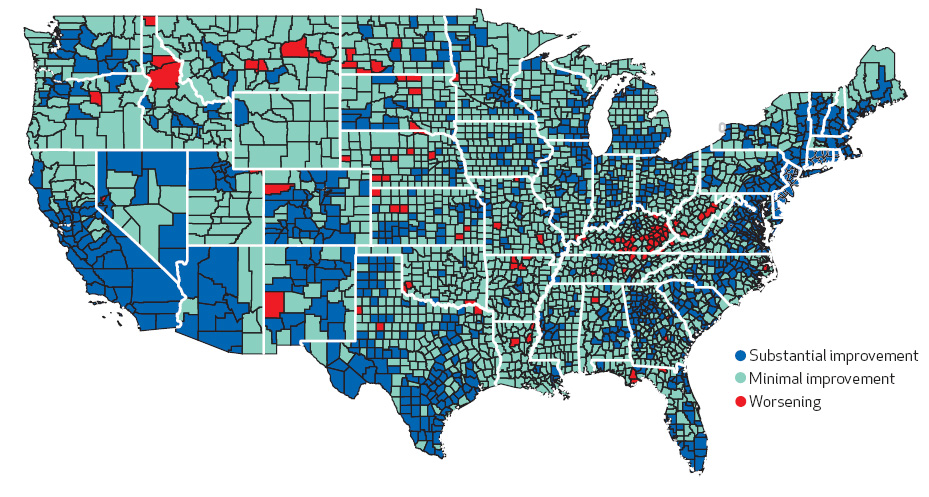
It's not entirely clear why some women might be facing a greater risk of premature death than others. Kindig's team found that mortality rates were not affected by access to primary care physicians. But there were links between higher female mortality and certain regional, behavioral and socioeconomic factors, such as living in the rural South or the West, higher smoking rates and lower education rates.
"Socioeconomic and behavioral factors are underappreciated for their effects on health, but with data like this, we see that those factors are important again and again," Kindig said.
The study is based on averages of the mortality rates in U.S. counties from 1992-1996 and 2002-2006. The researchers said they smoothed out any anomalies that may have been caused by big changes in sparsely populated counties.
Get the world’s most fascinating discoveries delivered straight to your inbox.
Their results were detailed this week in the journal Health Affairs. The findings highlight "the complicated policy reality that there is no single silver bullet for population health improvement," the researchers wrote.
"Investments in all determinants of health — including health care, public health, health behaviors and residents’ social and physical environments — will be required."
Follow LiveScience on Twitter @livescience. We're also on Facebook & Google+.


 Live Science Plus
Live Science Plus





