Breast-Milk Protein May Help Defeat Antibiotic-Resistant Bacteria
Get the world’s most fascinating discoveries delivered straight to your inbox.
You are now subscribed
Your newsletter sign-up was successful
Want to add more newsletters?
Join the club
Get full access to premium articles, exclusive features and a growing list of member rewards.
(ISNS) -- The fight against antibiotic resistance has gained an ally in breast milk. An ingredient found in human milk may make surface infections by the resistant bacteria MRSA more sensitive to attack by antibiotics, a team of researchers from the University at Buffalo, in New York, reports May 1 in the journal PLOS ONE.
The University at Buffalo team added a protein complex -- called HAMLET, after Human Alpha-lactalbumin Made LEthal to Tumor cells – purified from human milk to aggressive strains of antibiotic-resistant bacteria in Petri dishes and along the inside of the noses of mice. The researchers found that the bacteria were more responsive to antibiotics when they were used in combination with HAMLET.
"It sensitizes the bacteria to the antibiotics that they used to be resistant to, so suddenly, you can use the old [antibiotics] again," said Anders Hakansson, one of the study's authors. He is interested in the properties of human milk that protect infants from infections.
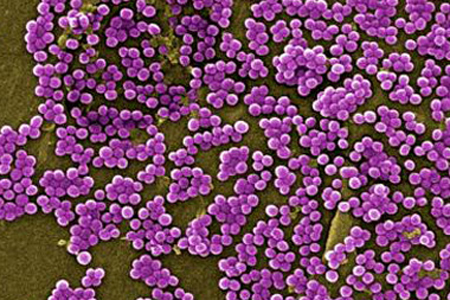
Getting a handle on the stubborn bacteria known as MRSA, methicillin-resistant Staphylococcus aureus, would be a public health relief. MRSA can spur antibiotic-resistant staph infections that are tough to treat.
In 2011, an estimated 11,285 people in the U.S. died from MRSA-related infections, according to the most recent data from the Centers for Disease Control and Prevention. And MRSA has become a common bug that patients pick up in hospitals.
Ironically enough, antibiotic resistance results from the increased use of antibiotics.
When an antibiotic kills bacteria, it can leave behind a small number of bacterial cells that have evolved defenses to the drug. The original antibiotic doesn't work on these mutated strains and the defiant bacteria multiply.
Get the world’s most fascinating discoveries delivered straight to your inbox.
Resistant bacteria can be treated with very high doses of antibiotics but those extreme levels would be toxic to people. Doctors often rely on new antibiotics to kill these superbugs. But eventually bacteria build up resistance to those antibiotics too.
"In the end, we really don't have any good way of treating those infections because they are resistant to essentially all antibiotics that we have," said Hakansson of MRSA. In 2012 the team reported that HAMLET used in tandem with antibiotics could control resistant strains of Streptococcus pneumoniae, a strain of bacteria that can cause pneumonia and other lung infections.
In MRSA, the researchers believe that HAMLET attacks pumps found in a bacteria's cell membrane. These pumps keep the material inside the cell and the solution outside the cell in a vital balance, thereby controlling the flow of nutrients and toxins into or out of the cell.
But HAMLET isn't strong enough to kill the MRSA cells, said Hakansson. He thinks the glitch in the cell's pumps may allow antibiotics to gain a foothold. "It could just be that you make the bacteria not completely happy in the presence of our protein but they're not unhappy enough that they will die," he said.
What's more, the team's results show that some strains of MRSA are more difficult to combat with HAMLET than other strains.
The authors don't yet know for sure how the cooperation between HAMLET and antibiotics actually works but the team is planning more experiments to peek into the cells.
The researchers believe HAMLET can be an important tool for treating bacterial surface infections.
Karen Bush, a biologist at Indiana University in Bloomington, worries that some of these infections will still require high doses of antibiotics even when paired up with HAMLET. Treating infections in the bloodstream with HAMLET could be even more difficult.
"I'm not sure that the protein would survive very long circulating in the bloodstream," said Bush, who was not involved in the study. In the blood, the HAMLET protein complex would simply fall apart, she said, and the large amounts of HAMLET needed to fight some of the most resistant infections might be challenging to deliver.
There is also the potential for resistance to antibiotics from repeated treatments.
"If you're constantly applying and ointment or cream to a wound, you are getting multiple exposures," said Bush.
Although the researchers report that resistance to antibiotics did occur in their experiments, they argue that while using HAMLET, it happens much slower than with the use of antibiotics alone.
Anders Hakansson and his wife, Hazeline Hakansson, also a scientist at the University at Buffalo, have started a company that will begin trials of HAMLET on untested bacteria and different types of infections.
Ryder Diaz is a science writer based in Santa Cruz, Calif.
Inside Science News Service is supported by the American Institute of Physics.
 Live Science Plus
Live Science Plus










