Some patients with brain injuries have life support withdrawn too soon, study suggests
A small modeling study suggests that some patients with severe traumatic brain injury may have recovered had they been kept on life support for longer.

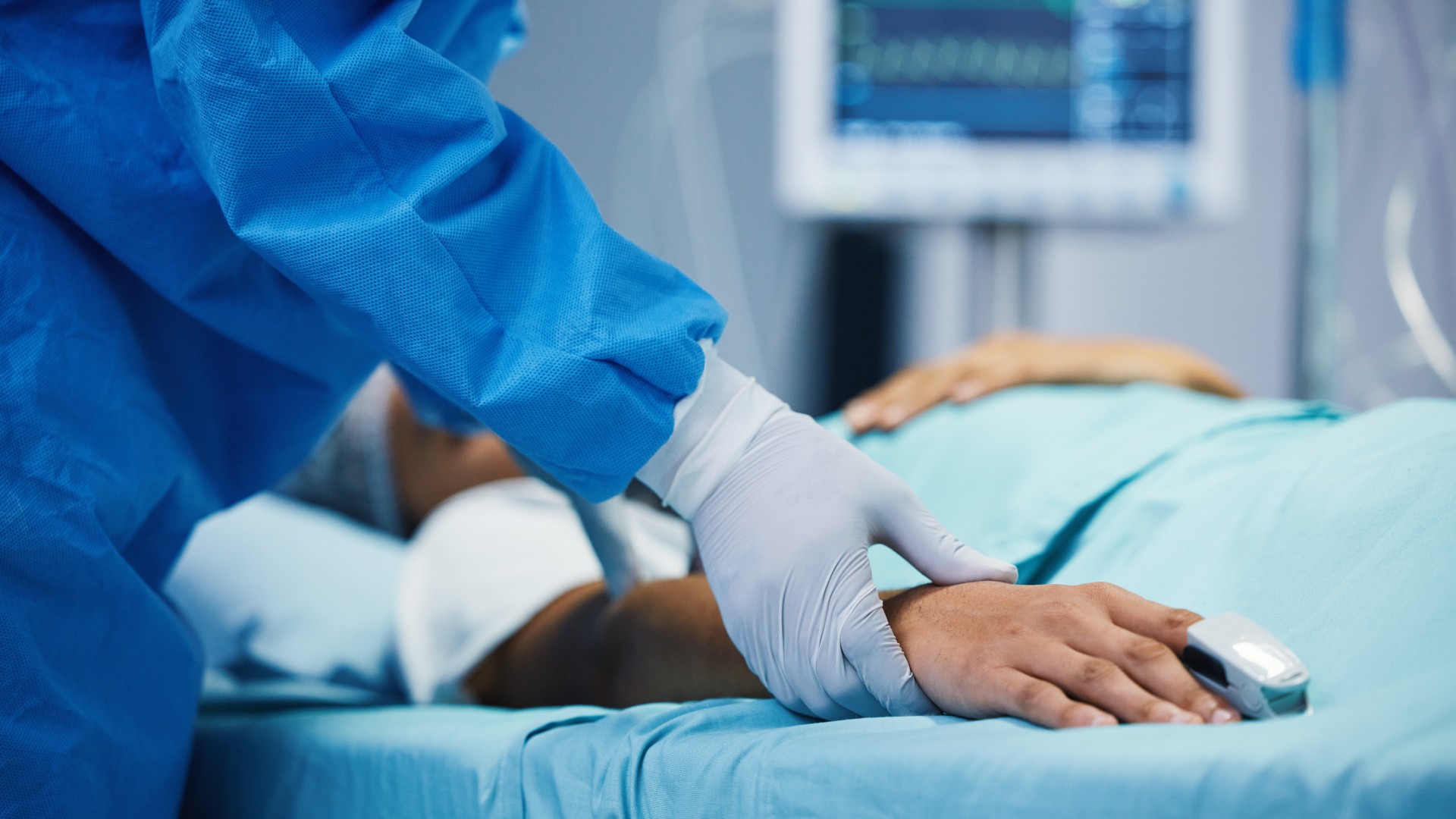
Life support for patients with severe traumatic brain injury (TBI) may sometimes be withdrawn too early, when it's possible that patients could eventually recover, new research suggests.
Every day, just under 200 Americans are estimated to die from a TBI, most commonly caused by fall, firearm-related injury or car crash.
Patients with severe TBI face a high risk of death or long-term disabilities that can affect their physical and cognitive abilities. People with these severe injuries may be given life-support in a hospital's intensive care unit (ICU); this care might include the use of a ventilator to assist breathing and drugs to reduce fluid build-up in the body. However, if doctors think a patient is unlikely to make a meaningful recovery, this support may be withdrawn.
According to the American College of Surgeons, patients with severe TBI in the ICU should receive "full treatment" for at least 72 hours after they sustain an injury. However, in the U.S., there are currently no clinical guidelines as to which patients should then have life support withdrawn or when that should happen.
Related: Lab-grown 'minibrains' help reveal why traumatic brain injury raises dementia risk
"We know that prognosis, or determining how somebody is going to recover after a severe traumatic brain injury, is incredibly imprecise," co-senior study author Yelena Bodien, an assistant professor in neurology at the Massachusetts General Hospital, told Live Science. "We are not able to give families precise information about whether their loved one will recover, to what degree and when," she said.
Clinicians often have to predict within just a few days of a patient's injury whether they are likely to die, develop a long-term disability or make a significant recovery. Doctors typically make these predictions based on clinical factors, such as the severity of a patient's injury — but again, there aren't standardized guidelines for how they should make their final prognosis. The prognosis is then relayed to a patient's caregivers and loved ones, who are often tasked with deciding whether to withdraw life support from the patient or not.
Get the world’s most fascinating discoveries delivered straight to your inbox.
Now, in the new study published May 13 in the Journal of Neurotrauma, researchers suggest that life support may occasionally be withdrawn when patients still have a chance of recovery.
Bodien and her colleagues looked at data from around 3,100 patients with severe TBI who had been seen in the emergency rooms of 18 different trauma centers across the U.S. within 24 hours of their injuries. Among these patients, the team identified 90 people who died around five days after being taken off a ventilator.
These patients were then "matched" to 80 patients who had similar characteristics, in terms of their ages and the severity of their injuries, for example, who were taken off a ventilator but continued to receive other forms of life support, such as a feeding tube. The team did not monitor how long this support continued, but Bodien acknowledged that it may have been for weeks, months or even years. The team compared data from the two groups to predict what the outcome may have looked like for the first group if their life support had not been withdrawn.
Among the 80 patients who were kept on life support, 55% died within six months of their injuries. However, among those who survived, more than 30%, or 24 patients, recovered at least some independence in daily activities within that same time frame.
The researchers argue that these outcomes would have been likely for a similar percentage of the patients whose life support was withdrawn. Because of this, the team argues that delaying the decision to withdraw support could benefit some TBI patients.
Considering these results and the prognostic uncertainty around severe TBI, clinicians should be cautious about early withdrawal of life support and families should feel empowered to request that such a decision be delayed, Bodien said.
The study is "certainly the best data that we have thus far," on this topic, Dr. Zachary Hickman, a neurosurgeon and assistant professor of neurosurgery at Mount Sinai Health System in New York who was not involved in the research, told Live Science.
The findings reinforce what clinicians already know — namely, that it is difficult to predict how someone is going to fare long-term after severe TBI, Hickman said. Sometimes, clinicians can underestimate the potential for recovery at the beginning, he added.
"Decisions to continue or limit life-sustaining measures in patients with severe brain injury are plagued by significant multidimensional uncertainty," said Dr. Christos Lazaridis, a professor in neurocritical care at the University of Chicago who was not involved in the research.
RELATED STORIES
"This study should add further caution when clinicians and families engage in shared-decision making concerning patients with acute brain injury," he told Live Science in an email.
The study does not address, however, how clinicians' predictions about patients' chances of recovery might be improved. Those answers could come with future research and would give patients' families and caregivers better guidance about what to do in these situations.
This article is for informational purposes only and is not meant to offer medical advice.
Ever wonder why some people build muscle more easily than others or why freckles come out in the sun? Send us your questions about how the human body works to community@livescience.com with the subject line "Health Desk Q," and you may see your question answered on the website!

Emily is a health news writer based in London, United Kingdom. She holds a bachelor's degree in biology from Durham University and a master's degree in clinical and therapeutic neuroscience from Oxford University. She has worked in science communication, medical writing and as a local news reporter while undertaking NCTJ journalism training with News Associates. In 2018, she was named one of MHP Communications' 30 journalists to watch under 30.

 Live Science Plus
Live Science Plus




