Do you really need to wear a lead apron to get an X-ray?
Lead aprons were designed to protect reproductive organs from radiation. But are they actually necessary?


Donning a shapeless lead apron may feel like a routine part of getting an X-ray. In theory, this heavy blanket is supposed to protect the body, particularly the reproductive organs, from radiation. But is it really necessary?
Probably not, for two main reasons, experts told Live Science. First, the radiation dose from a typical X-ray is nominal and unlikely to cause harm. Second, because X-ray radiation exposure levels are low, whatever minor reduction the lead apron provides is minimal and has no meaningful impact. For these reasons, several medical organizations now recommend against radiation shielding for most patients, and hospitals are gradually phasing lead aprons out of their radiology departments.
"The use of lead shielding for patients during their imaging procedure, particularly in relation to shielding of reproductive organs, does not appear to be effective for reducing the adverse effects of radiation," said Stephen Graves, an assistant professor of radiology at the University of Iowa Carver College of Medicine. (The University of Iowa stopped using lead aprons in the summer of 2022.)
"For something like a dental X-ray or chest X-ray, the radiation exposure to reproductive organs is similar to what an individual receives through normal background radiation exposure from geological and cosmic sources," Graves told Live Science in an email. (According to Graves, typical medical X-rays deliver radiation doses similar to those you'd experience on a trans-Atlantic flight due to cosmic radiation.)
In fact, in addition to lacking clear benefits, lead aprons could actually have downsides. "The use of lead shielding can occasionally obscure the patient anatomy being examined in diagnostic images, requiring the procedure to be repeated, effectively doubling the radiation exposure," Graves said.
Related: How radioactive is the human body?
What the science says
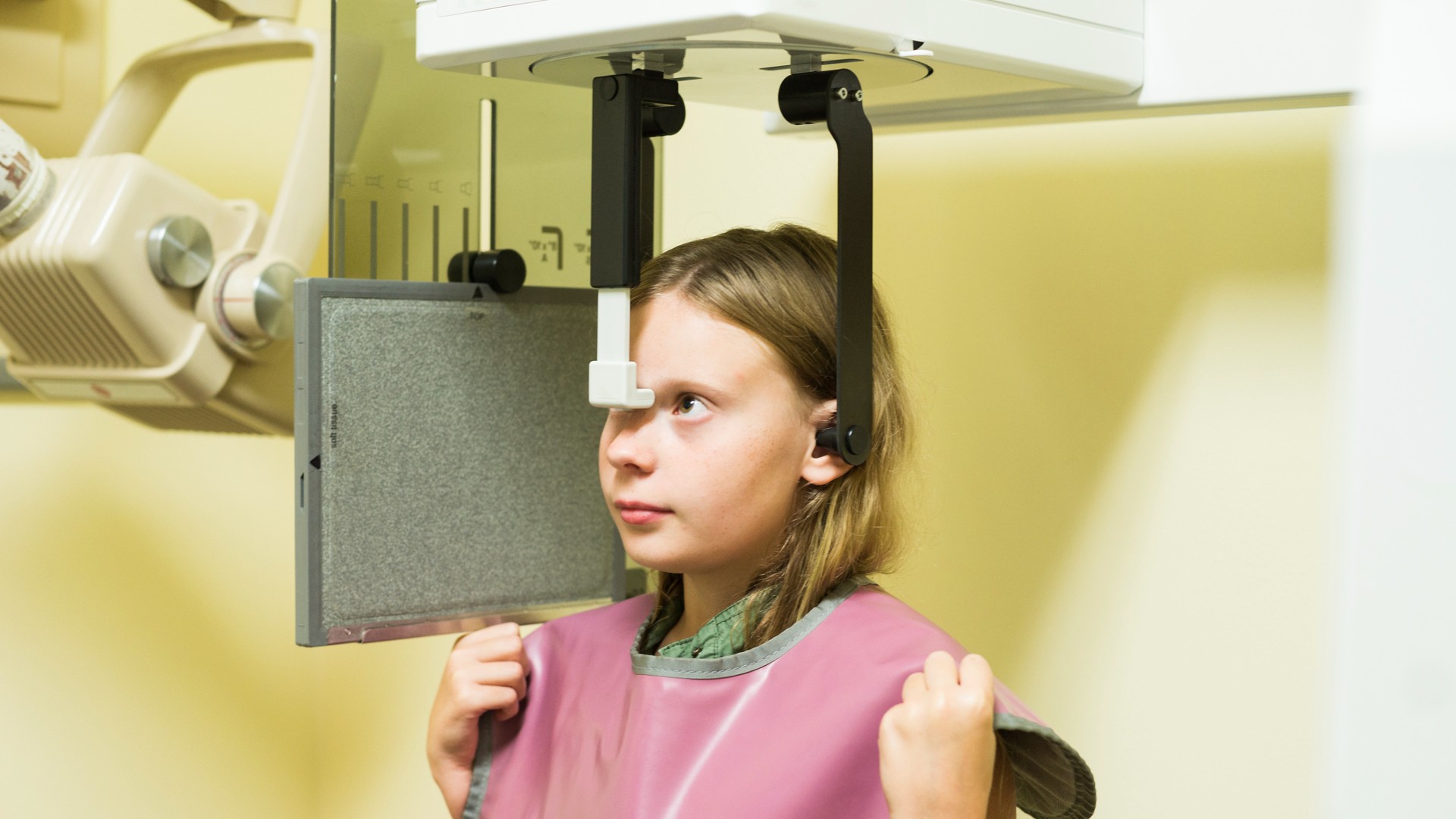
Patient shielding recommendations during X-rays has changed over the years.
Lead has a high density that is very hard for radiation to penetrate. As such, lead aprons were once a staple of radiology, as they were thought to protect sperm, eggs and fetuses from radiation-induced genetic mutations — a concern that led to federal regulations and an increased demand for such radiation shields. However, there's scant scientific evidence to support this practice.
Get the world’s most fascinating discoveries delivered straight to your inbox.
First, no research has demonstrated that radiation exposure can damage reproductive cells in ways that would lead to birth defects or other poor pregnancy outcomes. Even progeny studies of atomic bomb survivors whose reproductive organs were exposed to an atomic bomb explosion came up empty, casting doubt on the claim that gonads require special protection during X-rays.
As for the risk to fetuses, the American College of Obstetricians and Gynecologists' guidelines state: "With few exceptions, radiation exposure through radiography, computed tomography [CT] scan, or nuclear medicine imaging techniques is at a dose much lower than the exposure associated with fetal harm."
And then there were the lead aprons themselves, which studies found to be ineffective at meaningfully reducing X-ray exposure (and, as Graves mentioned, could occasionally obscure the images and necessitate additional X-rays). Still, it wasn't until 2019 that these observations culminated in a landmark position statement from the American Association of Physicists in Medicine (AAPM), a scientific organization focused on ensuring accuracy, safety and quality in the use of radiation in medical procedures, arguing that "shielding during X-ray based diagnostic imaging should be discontinued as routine practice" due to its tendency to obscure the image and "the minimal to nonexistent benefit" of the practice.
AAPM's statement opened the floodgates. "Many professional organizations have developed statements and recommendations about patient shielding, and conversations about how to implement these changes are ongoing," said Rebecca Milman, division chief of radiological sciences at the University of Colorado and author of the study upon which AAPM's statement was based.
A consensus statement on radiation shielding from several European medical organizations, for instance, came out in 2021 and closely reflected the AAPM's conclusions.
But change has come slowly. Milman admitted that it will be difficult to convince patients to ditch the aprons that physicians once claimed would protect them from radiation.
Related mysteries
"An essential aspect of this conversation is the perception of radiation risk, safety, and how this affects the perception and use of patient shielding," Milman told Live Science in an email. "How do we provide meaningful information to patients that will empower them to make informed decisions?"
These questions are made more salient by the nuances of the emerging guidelines. While physician groups no longer recommend that patients wear lead aprons during X-rays, they still suggest that medical providers should wear protective shielding made of lead or exit the room to reduce exposure. Although that makes sense because technicians face repeated exposure, patients may not immediately understand that difference in risk.
"Shielding policies should be based in science but flexible enough to account for individual patient needs," Milman said. "Facilities need to ensure that people are aware of the policy, especially the policy represents a substantial change in practice. This means communicating with radiologic technologists, physicists, radiologists, referring physicians, and patients as well as giving them an opportunity to ask questions about the policy."
This article is for informational purposes only, and is not meant to offer medical advice.

Joshua A. Krisch is a freelance science writer. He is particularly interested in biology and biomedical sciences, but he has covered technology, environmental issues, space, mathematics, and health policy, and he is interested in anything that could plausibly be defined as science. Joshua studied biology at Yeshiva University, and later completed graduate work in health sciences at Cornell University and science journalism at New York University.

 Live Science Plus
Live Science Plus





