FDA allows wide use of plasma for COVID-19 with little data that it works

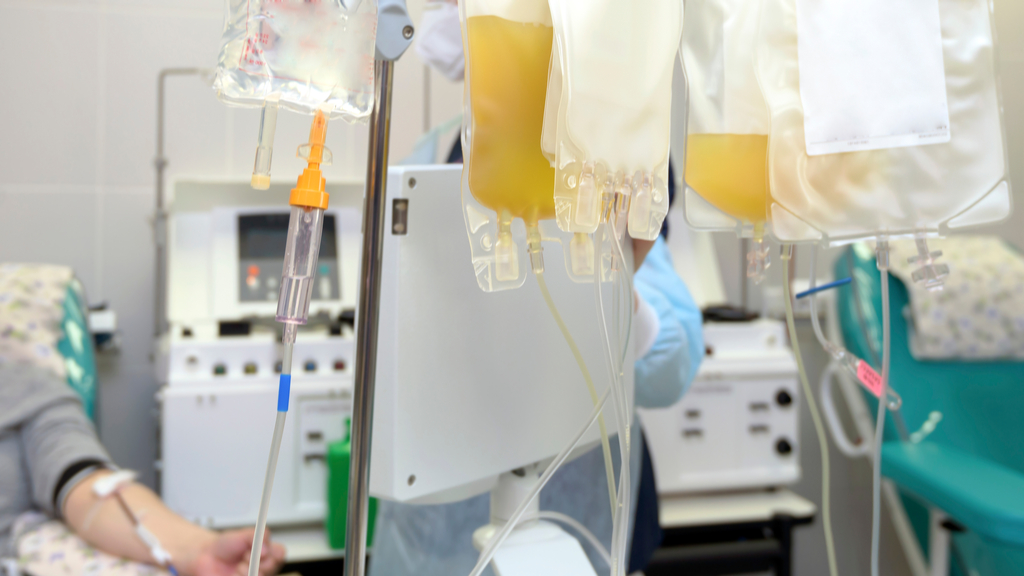
Last week, the U.S. Food and Drug Administration (FDA) announced that it would not allow widespread use of blood plasma to treat COVID-19 patients without more evidence that the therapy works.
Yesterday (Aug. 23), the agency apparently reversed this decision and issued an "emergency use authorization" for the treatment, according to a statement. An emergency use authorization does not require as much clinical evidence as full FDA approval, but does allow doctors to administer an experimental treatment "when there are no adequate, approved and available alternatives," according to the agency's website. That means doctors can use clinical judgment to prescribe plasma without enrolling recipients in a clinical trial to test its effectiveness.
While the authorization may allow more patients access to the therapy, the decision could undermine efforts to enroll patients in randomized controlled trials (RCTs) that would reveal if the treatment actually works, Live Science previously reported. In an RCT, patients are randomly assigned to receive either an experimental treatment or the standard of care, so the two can be compared.
Related: Treatments for COVID-19: Drugs being tested against the coronavirus
Convalescent plasma therapy uses antibody-rich plasma from people who have recovered from a disease and has been studied as a treatment for more than 100 years, but very few RCTs have demonstrated that the intervention works better than other standard treatments, Live Science previously reported. Only a handful of RCTs have been conducted with COVID-19 patients, and most have been too small to reach meaningful conclusions on their own.
The FDA's whiplash decision to authorize plasma therapy, despite needed data, follows remarks made by President Donald Trump that the hold on plasma "could be a political decision because you have a lot of people over there who don’t want to rush things because they want to do it after Nov. 3, and you’ve heard that one before," CNBC reported.
"We are being very strong and we are being very forthright, and we have some incredible answers, and we’re not going to be held up," Trump said in a news conference announcing the emergency authorization on Aug. 23, the eve of the Republican National Convention, Stat News reported.
Get the world’s most fascinating discoveries delivered straight to your inbox.
At the briefing, Trump and Secretary of Health and Human Services Alex Azar also said plasma therapy has been proven to reduce mortality by 35%, The New York Times reported. That's misleading, as no studies have shown that the treatment reduces mortality more effectively than the standard of care.
Neither Trump nor Azar cited exactly where they plucked that statistic from. Most likely, they were referencing a recent study conducted by the Mayo Clinic and National Institutes of Health, according to analyses by Stat News, The Times and various scientists on Twitter.
Outrageous to listen to @realDonaldTrump @secAzar @SteveFDA claiming a 35% improved survival in an observational preprint study compared w/ late-treated patients. There's no evidence to support any survival benefit. 2 days ago FDA's website stated there was no evidence for an EUAAugust 23, 2020
The study, posted Aug. 12 to the preprint database medRxiv, has not been peer-reviewed, was not randomized and did not include a control group, meaning no patients received the standard of care instead of plasma. Instead, the study compared two groups of hospitalized COVID-19 patients who either received plasma within three days of diagnosis, or after four or more days. The mortality rate among patients treated early was 8.7%, as compared with 11.9% in patients treated later. That means that patients treated early had a roughly 26% lower mortality rate than patients treated later.
The study also compared the mortality rates between patients based on the number of antibodies present in the plasma they each received. The mortality rate was 8.9% among patients who received plasma with "high" levels of antibodies, 11.6% in the "medium" group and 13.7% in the "low" group. That means the high-antibody group had a 35% lower mortality rate than the low-antibody group, which may be where Trump and Azar pulled the 35% statistic. However, the researchers obtained these antibody levels from stored plasma samples, so the results may be skewed by a "number of factors related to biospecimen handling and storage," the authors noted.
Related: 20 of the worst epidemics and pandemics in history
In addition to Trump and Azar, FDA Commissioner Dr. Stephen Hahn also made a misleading statement during yesterday's press briefing, seemingly in reference to this preliminary data.
"If the data continue to pan out, [of] 100 people who are sick with COVID-19, 35 would have been saved because of the administration of plasma." But plasma cannot be proven to dramatically improve survival without RCTs, which compare plasma to a different treatment; again, the Mayo trial compared plasma to plasma.
"A 35 percent improvement in survival is a pretty substantial clinical benefit," FDA Commissioner @SteveFDA said in relation to the convalescent plasma emergency use authorization issued today. pic.twitter.com/Dd97vLSZeLAugust 23, 2020
Related Content
RCTs for plasma therapy are difficult to organize. If an area isn't hit hard by COVID-19, there may not be enough people who have recovered who can donate plasma, or enough sick people to enroll in a clinical trial, Live Science previously reported. In addition, randomized trials pose a unique challenge in that some patients will randomly receive a treatment other than plasma, and that fact sometimes deters patients from enrolling, The New York Times reported on Aug. 19. Now that patients can receive plasma without being enrolled in a trial at all, attempts to organize RCTs may be further derailed. The end result is that more and more patients will receive a therapy that may not deliver the promised benefits.
But in any case, both RCTs and the emergency use of plasma rely on a steady supply of plasma donations — will there be enough to go around? Last month, the Trump administration announced the launch of an $8 million advertising campaign to encourage recovered COVID-19 patients to donate plasma, according to Stat News; however, it's unclear whether the campaign and emergency authorization will result in expanded access to the treatment across the U.S., as the president predicts.
To see a list of other potential COVID-19 treatments, see Live Science's coverage here.
Originally published on Live Science.

Nicoletta Lanese is the health channel editor at Live Science and was previously a news editor and staff writer at the site. She is a recipient of the 2026 AHCJ International Health Study Fellowship, with a project focused on antibiotic stewardship practices in Japan and the U.S. They hold a graduate certificate in science communication from UC Santa Cruz and degrees in neuroscience and dance from the University of Florida. Beyond Live Science, Lanese's work has appeared in The Scientist, Science News, the Mercury News, Mongabay and Stanford Medicine Magazine, among other outlets. Based in NYC, she also remains involved in dance and performs in local choreographers' work.

 Live Science Plus
Live Science Plus




