Should you mix and match COVID-19 vaccines?
Some experts weighed in.

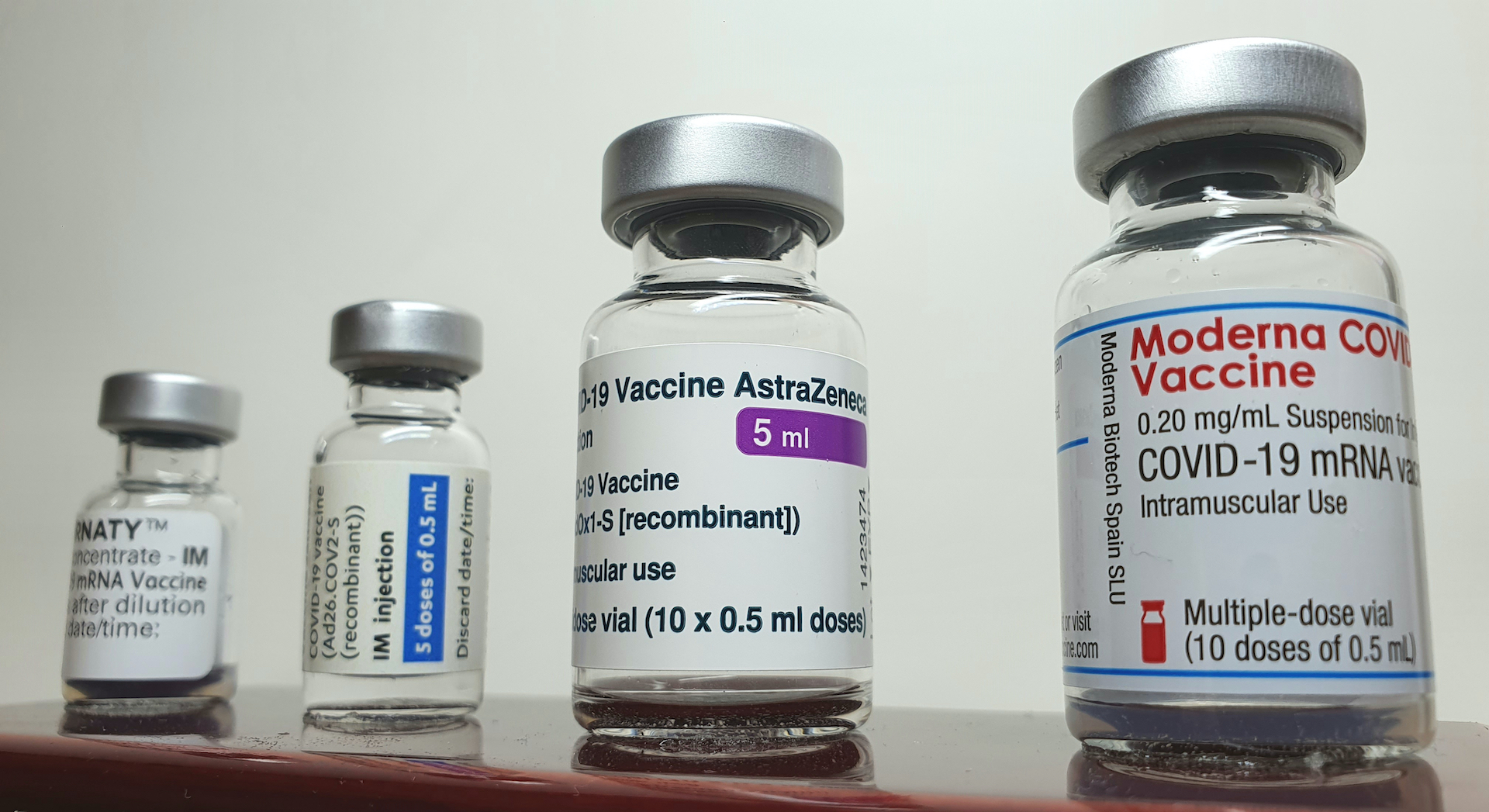
Many people will now be able to "mix and match" COVID-19 booster shots — that is, get a different COVID-19 vaccine for a booster, the Food and Drug Administration (FDA) announced Wednesday (Oct. 20).
Studies and real-world data have shown that this mix-and-match approach is safe and, in some cases, can even be more effective than not mixing. So should you get a booster vaccine that's different from your original dose? Live Science talked with a couple of experts, who agreed that mixing vaccines is perfectly safe, but their recommendations differed slightly.
The FDA has authorized booster doses for adults who are immunocompromised, who are 65 years or older or have underlying conditions, or those who are at high risk of exposure to COVID-19. People who received two shots of the Pfizer-BioNTech or Moderna vaccine are considered fully vaccinated and may be eligible for a booster at least 6 months from their last dose, whereas all adults who got the single-shot Johnson & Johnson vaccine are eligible to get a booster dose two months after their shot.
Article continues belowRelated: 14 coronavirus myths busted by science
Data suggest that in people who received one of the two mRNA vaccines — that is, Pfizer or Moderna — getting a booster of the other mRNA vaccine will likely be equivalent to getting the same one. But in people who originally received the Johnson & Johnson vaccine, getting a Pfizer or Moderna booster may spur a much better immune response than receiving a second Johnson & Johnson shot.
Evidence on mixing
The FDA's announcement to allow mixing and matching follows the early results of an ongoing National Institutes of Health (NIH) study. On Oct. 15, a group of researchers presented the results from the study, which hasn't yet been peer-reviewed and is posted as a preprint to medRxiv, to an FDA panel of experts.
The researchers tested nine different combinations of Johnson & Johnson, Moderna and Pfizer vaccines given to 458 participants and found that mixing was safe and highly effective. Receiving a booster shot greatly increased the circulating number of antibodies including neutralizing antibodies — molecules that bind to the virus and stop it from infecting cells — against SARS-CoV-2, the virus that causes COVID-19.
Get the world’s most fascinating discoveries delivered straight to your inbox.
In people who received a different booster than their original vaccine series, neutralizing-antibody levels increased 6.2- to 76-fold, depending on which vaccine combination they received. Those who received the same vaccine booster as their original vaccine saw their neutralizing-antibody levels increase between 4.2- and 20-fold, again depending on what vaccine they got.
The greatest increase in neutralizing-antibody levels was among those who originally received the single-dose Johnson & Johnson vaccine and then a Moderna booster; this group of participants had, on average, a 76-fold increase in antibodies 15 days after receiving their booster compared to before. The lowest increase — but still an increase — was in those who received the Johnson & Johnson vaccine for both their original dose and their booster. (The Moderna booster in this study was given at the same dosage as the original vaccine, but the FDA has authorized half the dosage for the booster shots that will be given to the public).
Average rise in neutralizing antibody levels
| Row 0 - Cell 0 | Row 0 - Cell 1 | Row 0 - Cell 2 | Row 0 - Cell 3 |
| Row 1 - Cell 0 | Pfizer-BioNTech Booster | Moderna Booster | Johnson & Johnson Booster |
| Two doses Pfizer-BioNTech Initially | 20x | 31.7x | 12.5x |
| Two doses Moderna Initially | 11.5x | 10.2x | 6.2x |
| One dose Johnson & Johnson Initially | 35.1x | 75.9x | 4.2x |
Levels were measured 15 days after booster shots as part of the NIH study.
For those who originally received an mRNA vaccine, there was also a slight advantage — though much less dramatic — in receiving a booster of the other mRNA vaccine.
Those who originally received Pfizer and then boosted with Pfizer had a 20-fold increase, whereas those who boosted with Moderna had a 31.7-fold increase; those who originally received Moderna and then boosted with Moderna had a 10.2-fold increase, whereas those who originally received Moderna and then boosted with Pfizer had an 11.5-fold increase.
"Based on the data that we've seen and everything that we've learned about the experience in other countries, I would probably recommend an mRNA vaccine as a second dose rather than a second J&J vaccine," for those who originally received a J&J vaccine as their first dose, said Dr. Carlos Malvestutto, an infectious-disease physician at The Ohio State University Wexner Medical Center.
But for people who received one of the two mRNA vaccines, it's fine if you get a booster of the same or the opposite one. You'll still "have a good response," Malvestutto told Live Science.
Dr. Eric Cioe-Peña, director of global health at Northwell Health in New York, agreed.
"What is clear from the data is that the best immune response comes from one of the two currently available mRNA vaccines," he told Live Science in an email. So people who received the Johnson & Johnson vaccine (or the AstraZeneca vaccine, which is similar in makeup to the Johnson & Johnson vaccine and has been approved in other countries) will have a stronger immune response if they receive an mRNA booster.
"What is not clear, and probably doesn't make sense, is the switch between the mRNA vaccines," he added. "
There doesn't seem to be a statistically significant difference between how these two vaccines are doing, and they work in remarkably similar fashion."
Still, not everyone is in agreement.
"If we can ensure that there [are] plenty of all three U.S.-approved vaccines, I would personally recommend sticking with your original vaccine," including for those who received the Johnson & Johnson vaccine, Rodney Rohde, a professor at Texas State University and chair of the university's Clinical Laboratory Science program. That's because "they're all looking fine with a boost," and there's more long-term data on the effectiveness of boosting with the same vaccine. Still, "I do think that it's safe to mix and match, and it might come down to what's available," he told Live Science.
Real-world data
This NIH study isn't the only data that point to the safety and possible benefits of mixing and matching vaccines. Countries such as Turkey have been mixing and matching vaccines for some time now, boosting people who received two doses of the China-made Sinovac vaccine with one or two doses of the Pfizer vaccine.
Data from the U.K. and Canada, which have been giving a second dose of Pfizer on top of an original dose of the AstraZeneca COVID-19 vaccine — an adenovirus vaccine that uses the same platform as Johnson & Johnson — have also shown that mixing and matching can be safe and highly effective.
Even before the NIH study results, it was clear from these real-world studies that mixing and matching was safe and prompted a robust immune response. "What we saw was basically the same types of [adverse reactions] that we see with the first and second dose of these vaccines but nothing worse or nothing scary," Malvestutto said. "The evidence shows it is quite safe."
Related: Which COVID-19 vaccine has the lowest rate of breakthrough infections?
What's more, some evidence suggests that mixing and matching these vaccines may lead to a broader immune response that may be better able to respond to a future SARS-CoV-2 variant, Malvestutto said. Still, many questions remain about how effective this approach is for other parts of the immune response.
RELATED CONTENT
"Immunity is not just about the levels of the antibodies; there are other parts to the story," Malvestutto said. The NIH study focused solely on the levels of antibodies. Another extremely important part of the immune response is what are known as memory cells, which circulate in the body long after neutralizing-antibody levels have depleted and prompt the immune system to make more targeted antibodies once exposed to the pathogen.
We still need data on whether the mix-and-match approach has a better, worse or same effect on producing these memory immune cell responses, Malvestutto said.
In any case, the data suggest that mixing and matching is safe and effective. But the most important message is for people to complete their initial vaccinations, and if they're in high-risk groups, to get their boosters, he said.
Originally published on Live Science.
Editor's Note: The article was updated at 2:30 p.m. ET to clarify that all adults who initially got a Johnson & Johnson shot are eligible to get a booster.

Yasemin is a staff writer at Live Science, covering health, neuroscience and biology. Her work has appeared in Scientific American, Science and the San Jose Mercury News. She has a bachelor's degree in biomedical engineering from the University of Connecticut and a graduate certificate in science communication from the University of California, Santa Cruz.