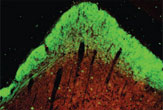
Scientists partially restored the vision in blinded hamsters by plugging gaps in their injured brains with a synthetic substance that allowed brain cells to reconnect with one another, a new study reports.
If it can be applied to humans, the microscopic material could one day help restore sensory and motor function to patients suffering from strokes and injuries of the brain or spinal cord. It could also help mend cuts made in the brain during surgery.
"If we can reconnect parts of the brain that were disconnected by a stroke, then we may be able to restore speech to an individual who is able to understand what is said but has lost the ability to speak," said study team member Rutledge Ellis-Behnke from the Massachusetts Institute of Technology.
The substance contains nano-sized particles that self-assemble into a fibrous mesh that mimics the body's natural connective tissue when placed in contact with living cells.
The mesh allows existing neurons whose axons have been severed by injury or stroke to reconnect. Axons are branch-like projections that link neurons to one other, allowing them to communicate. When many axons are bundled together, they form a nerve.
The study is detailed in this week's online version of the journal for the Proceedings of the National Academy of Sciences.
Nearly good as new
Get the world’s most fascinating discoveries delivered straight to your inbox.
The researchers severed a nerve tract within the visual system of both young and adult hamsters, which resulted in blindness. For some of the animals, the synthetic substance, called SAPNS, was applied immediately after the incision. Other animals were given saline as a control.
Within 24 hours, all of the animals treated with SAPNS showed signs of healing; with time, the gaps in their brain tissues closed up completely.
In the adult group, vision was functionally restored within six weeks. In one animal, the severed nerve tract was restored to more than 80 percent that of a normal animal. In other studies, the researchers found that nerves needed to be only about 40 percent healed for animals to have functional vision.
"This is way above that," Ellis-Behnke said in a telephone interview.
Heals young and old alike
The researchers were surprised to find that the brains of the adult animals responded as well to the treatment as younger animals that were still growing.
"We thought we would need to promote growth to get regeneration in the adults but we found we didn't need that," Ellis-Behnke said.
It's not exactly clear how SAPNS works. The researchers think the substance might somehow promote the migration of brain cells into the wound from other areas. Another possibility is that it closes a wound gap by bringing its two sides together through a contractile process.
The researchers believe SAPNS is better than currently available biomaterials because it works on a level similar in scale to the body's natural support structure, called the "extracellular matrix." It is also biodegradable, disappearing from the wound site after about four weeks; it typically passes through the animals' urine, but it might also be taken up by surrounding tissue for use in protein construction.
SAPNS also doesn't seem to rouse the body's immune system, so tissue rejection isn't a concern. And because it's synthetic, SAPNS is free of biological contaminants that show up in some animal products such as collagen.
Limitations
The findings are intriguing and will be an exciting first step towards the goal of axonal regeneration if they can be confirmed, said Wolfram Tetzlaff, a neuroscientist at the International Collaboration On Repair Discoveries (ICORD) at the University of British Columbia.
It is unclear, however, how well SAPNS will work in real-world situations, said Tetzlaff, who was not involved in the research. For one thing, the wounds in the current study were made using sharp surgical knives.
"This is a very nice, clean transaction. Most injuries do not come that way," Tetzlaff told LiveScience. "Unless you live in Miami and somebody stabs you from the back, you don't get these types of clean lesions."
Also, SAPNS was applied immediately after the cuts were made, which allowed very little time for scar tissue to form.
It's possible that surgeons could create a fresh cut or remove scar tissue around an injury before applying SAPNS, Tetzlaff said, but this might not always be the best course of action.
"Most surgeons are very reluctant to do that because it's so difficult to see what is scar and what is healthy tissue," Tetzlaff said.
Ellis-Behnke said SAPNS will most likely be one part of a group of therapies for axon regeneration and nervous-tissue healing. The team is currently investigating the effect of SAPNS on spinal cord injuries and other types of injuries, as well as its effectiveness when applied some period of time after injury.
"We're very cautiously optimistic, but we also know this is not the Holy Grail," he said.
- Brain Power: Mind Control of External Devices
- Video Games May Help Stroke Victims
- Adult Brain Cells Do Keep Growing
- Partially Paralyzed Mice Walk Again

 Live Science Plus
Live Science Plus





