MRSA Superbug May Get Stronger If You Smoke

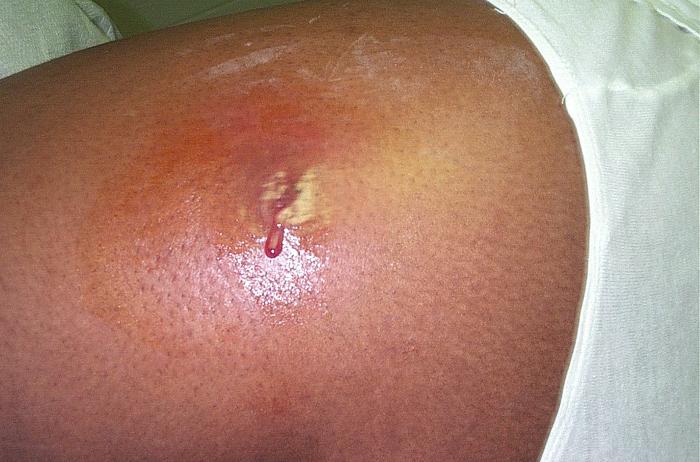
Cigarette smoke apparently isn't deadly for all living creatures. At least one type of bacterium — MRSA, the superbug commonly found in hospitals — apparently thrives on the stuff.
In fact, cigarette smoke makes MRSA stronger and more resistant to antibiotics, which could mean it is worse for human health, according to a new study. The surprise finding appears online this month in the journal Infection and Immunity.
MRSA, short for Methicillin-resistant Staphylococcus aureus, is a type of "staph" bacterium resistant to most antibiotics and is capable of causing life-threatening skin and bloodstream infections as well as pneumonia.
In 2005, MRSA caused nearly 19,000 deaths in the U.S., according to the Centers for Disease Control and Prevention. In recent years, however, the number of infections has decreased by more than 25 percent, and in 2012 there were about 10,000 MRSA deaths, according to CDC data.
The new study began after Dr. Laura Crotty Alexander, a pulmonologist at the VA San Diego Healthcare System, noticed that many of the patients she treated who were smokers had MRSA infections, and wondered whether there was a connection.
Crotty Alexander and her colleagues at the University of California, San Diego, created two batches of MRSA in their lab — one grown normally and the other grown with exposure to cigarette smoke. They then infected human immune cells called macrophages with each of these MRSA samples. Macrophages are a type of white blood cell, and are among the first line of defense to attack MRSA and other sources of infections. [6 Superbugs to Watch Out For]
The macrophages could kill both samples, but they had a much harder time killing the MRSA exposed to cigarette smoke. Digging deeper, the researchers found the reason.
Macrophages kill foreign invaders by engulfing them and then releasing chemicals called reactive oxygen species, such as peroxides, that break apart the invader's cellular walls. These chemicals are highly reactive and thus disrupt chemical bonds holding the bacteria together.
The researchers found that the cigarette-exposed MRSA not only had protection against reactive oxygen species, but also against the antimicrobial proteins that mammals produce, which can poke holes into the bacteria. Although the precise mechanism of how smoke may change bacteria is not fully understood, the researchers wrote that cigarette smoke may alter the chemical charge of MRSA's bacterial cell wall, making it easier for the superbug to repel both antimicrobial proteins and reactive oxygen species.
In mice, the cigarette-exposed MRSA was deadly. Forty percent of mice infected with these bacteria died of pneumonia, compared with 10 percent of the mice infected with regular MRSA, the researchers reported.
"Cigarette smokers are known to be more susceptible to infectious diseases," Crotty Alexander said. "Now we have evidence that cigarette smoke-induced resistance in MRSA may be an additional contributing factor."
The changes induced on MRSA by smoking might be heritable from one generation to the next, the researchers reported.
This means smoking may make MRSA even more deadly for everyone…sort of like exposure to second-hand MRSA.
Follow Christopher Wanjek @wanjek for daily tweets on health and science with a humorous edge. Wanjek is the author of "Food at Work" and "Bad Medicine." His column, Bad Medicine, appears regularly on Live Science.
Get the world’s most fascinating discoveries delivered straight to your inbox.

Christopher Wanjek is a Live Science contributor and a health and science writer. He is the author of three science books: Spacefarers (2020), Food at Work (2005) and Bad Medicine (2003). His "Food at Work" book and project, concerning workers' health, safety and productivity, was commissioned by the U.N.'s International Labor Organization. For Live Science, Christopher covers public health, nutrition and biology, and he has written extensively for The Washington Post and Sky & Telescope among others, as well as for the NASA Goddard Space Flight Center, where he was a senior writer. Christopher holds a Master of Health degree from Harvard School of Public Health and a degree in journalism from Temple University.

 Live Science Plus
Live Science Plus




