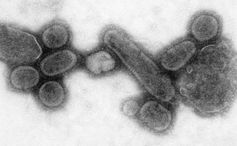
Deadly Airborne Flu Virus Created in Lab – Not as Bad as It Sounds (Op-Ed)
Get the world’s most fascinating discoveries delivered straight to your inbox.
You are now subscribed
Your newsletter sign-up was successful
Want to add more newsletters?
Join the club
Get full access to premium articles, exclusive features and a growing list of member rewards.
This article was originally published at The Conversation. The publication contributed the article to Live Science's Expert Voices: Op-Ed & Insights.
Influenza viruses that exist in nature and affect wild birds shuffle their genes about all the time, creating new viruses with different genetic combinations. In this way a virus was created that in 1918 replicated well and transmitted efficiently in humans. Known as the “Spanish flu”, it was one of the deadliest pandemics in human history, killing up to 50m people worldwide.
Now scientists at the University of Wisconsin-Madison in the US have been criticised for recreating a very similar but distinct influenza virus by mixing together a set of genes taken from viruses of wild birds that are present in the gene pool today. Critics argue that it is hugely dangerous. And it is not the first time scientists have come in for criticism for creating influenza viruses.
Article continues belowIn their paper, published in Cell Host & Microbe, Yoshihiro Kawaoka’s group from Wisconsin found that although the recombinant virus was harmful, it did not transmit. But when they added in some adaptive changes like those selected during virus replication in mammals such as humans or pigs, they created a virus that was transmissible and virulent in ferrets, the best model for human flu. By retracing the evolutionary steps that created the 1918 virus, they re-enacted how the virus can switch from harmless avian virus to a potentially pandemic one.
Could it happen again in nature?
But just because scientists could make this virus does not mean that nature will inevitably do so. What we still lack from this work is a quantification of the risk; how many rolls of the dice would it take for this scenario to arise today and under what conditions would evolution favour those events?The 1918 virus was in fact “resurrected” by scientists a decade ago and it turned out to be one of the most virulent influenza strains ever studied. Some may think that because the virus emerged a century ago it was a one-off historical event that could not happen again today. The new work shows that is not the case. Now that knowledge can be used to justify further research to help combat future influenza outbreaks including stockpiling of drugs and renewing of pandemic plans.
What the work does show is that the 1918 virus was not a “one-off” and that knowledge can be used to justify further research to help combat future influenza outbreaks including stockpiling of drugs and renewing of pandemic plans.
What if the lab virus escaped?
Reassuringly, the particular virus created by Kawaoka and colleagues was recognised by antibodies from people vaccinated against the modern day 2009 pandemic influenza. This suggests that if it were to escape the lab it would not be good at infecting and spreading in people as most of us already have that type of antibody as a result of being vaccinated or naturally infected since 2009.
Get the world’s most fascinating discoveries delivered straight to your inbox.
This type of knowledge forms part of the risk assessment that scientists perform before they begin this type of work and which is updated as the experiment proceeds.
Finding the right vaccines
The data also has implications for vaccine production because the new virus that transmitted in ferrets differed from the starting avian virus in its recognition by antibodies. This suggests that “prepandemic” vaccines generated using original avian viruses before a pandemic virus emerges may not work as well as we would hope. With this new knowledge we might be able to pre-empt the changes and correct that deficit.
It is important with this type of work to make sure we learn as much new information as possible from each experiment and always to ask ourselves as scientists if we could learn these things in a safer way. Sometimes that is possible but it is difficult to envisage how that could be in this particular case.
If we want to understand how to deal with viruses that are both highly virulent and transmissible, we need to have such a virus to work with. This should be done by experts under very highly contained conditions such as those used in Wisconsin in the Kawaoka labs.
Nonetheless, scientists do not have a licence to create at will any virus they dream up – each one needs to be risk assessed individually and the reasons for doing the experiment should be clear. And we should of course continue with an informed debate on where the limits of our scientific endeavours should lie not just for research with flu viruses but with other pathogens and scientific advances as well.
Wendy Barclay's laboratory is funded by the Medical Research Council, the Biotechnology and Biological Sciences Research Council, the Wellcome Trust and commercial bodies.
This article was originally published on The Conversation. Read the original article. Follow all of the Expert Voices issues and debates — and become part of the discussion — on Facebook, Twitter and Google +. The views expressed are those of the author and do not necessarily reflect the views of the publisher. This version of the article was originally published on Live Science.
 Live Science Plus
Live Science Plus