What is Flesh-Eating Bacteria?

A Georgia college student is in critical condition after getting infected by flesh-eating bacteria during a zip line accident last week. When the zip line broke, Aimee Copeland, 24, fell and cut her leg; she got stitches and went home to recover, but soon returned to the hospital with severe pain deep in her leg. The leg was amputated, but the infection spread to other parts of her body, and she most likely faces additional amputations of her hands and remaining foot.
What is flesh-eating bacteria, and why is it so deadly?
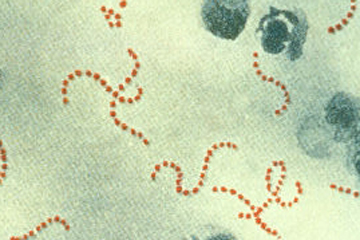
Necrotizing fasciitis, as Copeland's condition is called, is a severe bacterial infection that destroys muscles, skin, and underlying tissue. (The word "necrotizing" refers to something that causes body tissue to die.) Although many types of bacteria can cause the infection, the bacteria Streptococcus pyogenes — the same pathogen that causes Strep throat — brings on a particularly severe and often deadly form of the disease when it infects the fascia, or connective tissue that surrounds muscles, blood vessels and nerves.
Article continues belowAccording to the National Institutes of Health, "Necrotizing soft tissue infection develops when the bacteria enters the body, usually through a minor cut or scrape. The bacteria begins to grow and release harmful substances (toxins) that kill tissue and affect blood flow to the area. As the tissue dies, the bacteria enters the blood and rapidly spreads throughout the body."
In the case of S. pyogenes, the bacteria produces a toxin known as a superantigen, which activates white blood cells called T-cells, causing an overproduction of proteins called cytokines. These wreck havoc on cells.
Immediate treatment of necrotizing fasciitis is needed to prevent death — a dilemma, as the disease can often go overlooked by doctors. The bacteria invades tissue deep inside a wound while the surface through which it entered appears to be healing normally, Dr. William Schaffner of the Vanderbilt University Medical School told Reuters.
"This often is a very subtle infection initially," he said. "These bacteria lodge in the deeper layers of the wound. The organism is deep in the tissues and that's where it's causing its mischief."
Get the world’s most fascinating discoveries delivered straight to your inbox.
Treatment includes powerful, broad-spectrum antibiotics given immediately through a vein, surgery to drain the sore and remove dead tissue, and, in some cases, a dose of antibodies called donor immunoglobulins to help fight the infection.
This story was provided by Life's Little Mysteries, a sister site to LiveScience. Follow Life's Little Mysteries on Twitter @llmysteries, then join us on Facebook.

