The Truth About Deadly 'Superbugs'
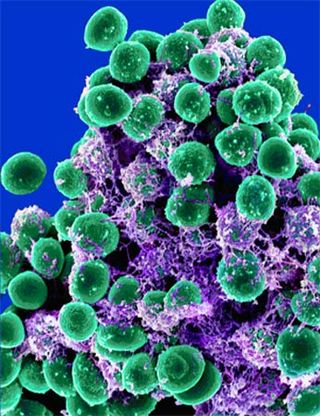
NEW YORK – Armies of invisible creatures are spreading across the planet, infesting local communities and claiming the lives of innocent children in their wake. And the attackers are immune to some of the world's best weaponry. It sounds more like a sci-fi movie plot than reality, but "superbugs"—deadly microbes that can resist drugs designed to wipe them out—are far from imaginary. Schoolchildren in several states recently have died from infections caused by MRSA bacteria, otherwise known as methicillin-resistant Staphylococcus aureus, and medical recordkeeping shows such cases are increasing annually. MSRA spreads via surface-to-surface contact, developing into a staph infection if conditions are right. The first symptoms can include pimple-like sores on the skin where the bacteria launch their attack, while rarer but more advanced infections can enter the bloodstream, attack organs and lead to death. But need the masses live in fear of stubborn yet deadly microbes such as MRSA as their numbers rise worldwide, or are we overreacting? Most medical experts think superbug diseases are here to stay but offer a major caveat: Only a fraction of the population need worry a little, if at all. The numbers An estimated 18,650 Americans died in 2005 from MRSA, a microbe whose defenses have benefited from decades of assault by antibiotics. "The spread of MRSA isn't a flash in the pan. It's been around for about 50 years now," said Dr. Cyrus Hopkins, an infectious diseases specialist at Massachusetts General Hospital. Healthy people are hardly its favorite customers and rarely meet the microbe. About 77 percent of deaths from MRSA in 2005 occurred in people 65 or older, according to a recent study in the Journal of the American Medical Association, an age bracket known for weakened immune systems. For people younger than 65, the chances of dying from a lightning strike (about 1 in 600,000) are greater. "I think people should understand that the chance of being exposed to a superbug is very small," Hopkins said. "Even if they are exposed, the chance they'll get sick from it is very small. And if they do get sick, most healthy people survive." The chances are low, Hopkins explained, because the body's immune system can fight dangerous invasions; in addition, populations of "friendly" microbes living inside of our bodies easily out-compete invaders. Twenty-five to 30 percent of people, in fact, carry harmless S. aureus bacteria inside their nose as "natural flora." The principle of natural flora explains how most Escherichia coli strains live peacefully within our intestines. Eat some spoiled or improperly cooked food, however, and a bigger dose of those or other more foreign bacteria can lead to diarrhea or infection if the microbial visitors to your gut are virulent, as were E. coli strains contaminating spinach earlier this year. Evolution on drugs But where do the harmful, drug-resistant nemeses come from? Experts think the answer lies in how we combat diseases with antibiotics. Antibiotics shut down unruly bacteria directly, police them until the immune system can rid of them or both. And each new antibiotic on the market works well—at least for a few years, said Dr. Martin Blaser, a professor at New York University's School of Medicine and former president of the Infectious Diseases Society of America (IDSA). Medical experts such as Blaser think the forces of evolution start working as soon as patients carrying a dangerous microbe receive antibiotics. "Anyone who doesn't believe in evolution just has to look at MRSA," Blaser said of the microbe's growing arsenal of drug resistance. Kill off millions or billions of harmful bacteria with an antibiotic, and some stragglers with a life-saving genetic change carry on their heritage. If a similar drug is used again, it's much less effective than before; repeat the cycle, and eventually microbes like MRSA make news headlines. Making matters worse, Blaser said, is that drug companies have little incentive to create new antibiotics—they are expensive to test, and the customer turnaround is quick and unprofitable. "Until we develop new antibiotics and change our usage—we use antibiotics like water—these problems will persist," said Blaser, who is lobbying congress with other IDSA members to offer monetary incentives to develop new antibiotics. But recent victims of virulent S. aureus strains that killed schoolchildren have many medical experts on edge, as most victims were healthy. Blaser said the responsible MSRA strains probably did not come out of hospitals, which are well-known breeding grounds for drug-resistant diseases. "It's not just affecting previously ill people," Blaser said. "It's football players, wrestlers and just plain healthy kids." Blaser thinks the microbial attackers somehow evolved to be more invasive than their more bashful in-laws. Sustained attack The growing world population may be the force whacking the evolutionary beehive for virulence, a measure of a microbe's ability to infect something. People used to live in small, spread-out communities, so when super-aggressive diseases did appear, Blaser said they couldn't get very far. "Every time a virulent disease popped up, it was 'end of story.' They had nowhere else to go," he said. But today, populations are immense, tightly connected around the globe and contain growing elderly populations as well as carriers of immune-weakening diseases such as HIV. Blaser said the combination is a recipe for disaster, and his group's new model of that recipe was detailed the Oct. 18 issue of the journal Nature. "We did not make the laws of nature," Blaser said. Even though we may not like them, we need to understand them to better control infectious diseases."
Chamber of wisdom Trying to understand infectious diseases is what engineer Clive Beggs has built his career around—quite literally. The medical technology professor at the University of Bradford in England has helped build one of only a few chambers in the world that can precisely study the hospital environments in which microbes tend to infect people. "If you look at a common laboratory, you'll find microbes in Petri dishes or in a broth, but that tells you little about how they really behave in realistic environments," Beggs said. The 2,825-cubic-foot (80-cubic-meter) climate-controlled room goes online in November and contains a mock-up of a hospital ward. The research team made of doctors, engineers, mathematicians and other specialists hopes to study how microbes "get from A to B and what they do in between," Beggs said. "We want to see how nurses tear down patients' beds, for example, and find out how that might help spread microbes like C. diff," Beggs said, referring to Clostridium difficile—a drug-resistant microbe that is currently ravaging hospitals in Europe. "It's difficult to do the research we'd like to do in a real hospital," he said. "There are bureaucratic issues in gaining access to hospitals, and there's a huge amount of variables we can't control." In addition, Beggs said follow-up clinical studies are long and expensive—so having the most accurate and reliable information possible before taking the plunge is crucial. Before the researchers investigate how best to clean hospital rooms, however, they will first focus on how humidity affects superbugs. "A few studies suggest the drying effects of (air conditioning) could control the spread of some microbes," Beggs said. "But overall, there's little research in this area. We want to change that and possibly help people." Beggs said such environmental countermeasures to prevent bacteria's spread are extremely important, especially if there are fewer new antibiotics in the pipeline. "In general, hospitals are doing everything they can to maintain clean and safe facilities, but we don't fully understand how ward environments affect the spread and development of superbugs," he said. Stopping a superbug While research groups such as Beggs' come up with new ways to thwart dangerous microbes and others seek new antibiotics, some experts think vaccines are as important as ever. Problem is, the disease-preventint injections are as financially unattractive as new antibiotics. "Nobody will invest in a vaccine to fight a disease that isn't very widespread," said Donald Kennedy, a medical professor at St. Louis University's School of Medicine. If vaccine development could get a boost, however, Kennedy thinks microbes like MRSA could get the boot, much like smallpox, or at least be set back as measles, polio and hepatitis B are in the United States. "Vaccination strategies have eliminated or reduced those diseases, not treatment strategies," he said. "It's a challenge, but if we're smart enough we could do it. Most people would rather not catch a disease than take drugs while they have one." Until more advanced solutions come along, people are sticking to tried-and-true advice any doctor would offer: Wash your hands, and wash them often. "That's what our school is recommending our students do," said Tricia Gordon, a public high school teacher in Manassas, Va., where MRSA outbreaks have occurred. "We've sent out public health warnings and information. We're also now requiring kids who play sports to get cleared if they have any sores and we've updated our cleaning supplies to handle (MRSA)." Gordon said most people use the information responsibly, but some seem to be acting a little paranoid. "Some people think the situation is a bit extreme, with kids thinking they have it when with every little pimple that shows up," she said. "Knowledge is power, but you have to keep your head screwed on and act on common sense." To do that, Hopkins said following up on public health warnings is crucial. "Don't react to the 11 o'clock news and get scared. Go to your health department's Web site for detailed information," Hopkins said. "And don't forget to wash your hands."
- Video: Bird Flu Pandemic! Will it Happen?
- 10 Things You Didn't Know About You
- Top 10 Mysterious Diseases
Sign up for the Live Science daily newsletter now
Get the world’s most fascinating discoveries delivered straight to your inbox.
Most Popular



