'Poop Transplants' Stall Amid New Rules
Poop transplants, which have become a more common way to treat potentially deadly bacterial infections in the intestines in recent years, have come to a near standstill amid new rules from the Food and Drug Administration regarding the procedure.
The FDA said last month that it considers the procedure, formally known as fecal microbiota transplantation, to be a biological product, and so it falls under the agency's regulation. The new rules require doctors to submit a special application before they are allowed to perform the procedure.
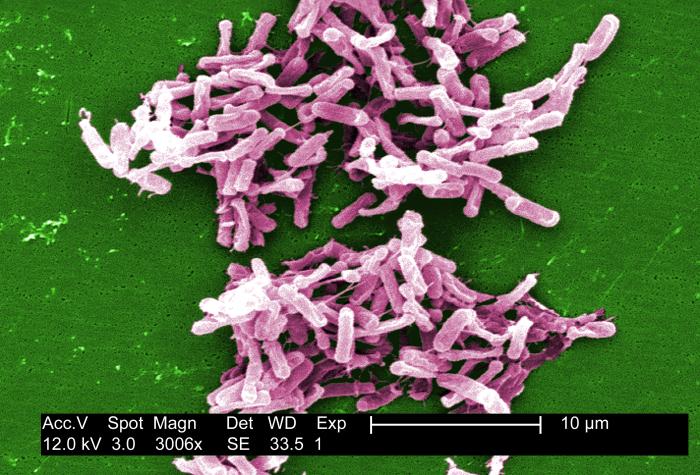
Fecal matter transplants had been essentially unregulated before the FDA statement. The transplants — which involve taking fecal matter from a donor and delivering it to patients' colons through a tube — have been shown in studies to be a very effective therapy for treating the bacterial infection Clostridium difficile. The infection, which causes severe diarrhea, is notoriously difficult to cure.
The new rules are intended to make sure the procedure is safe — to ensure for instance that donors are screened for certain infectious diseases, and that doctors do not perform the procedure unnecessarily.
However, some say the rules are hindering sick patients from getting access to a treatment that they need.
"The regulation by the FDA has created a denial, or an interrupted access, of care for patients," said Dr. Johan Bakken, an infectious disease specialist at the University of Minnesota.
The application process is extensive, and doctors may wait up to 30 to 45 days before they hear back from the FDA, Bakken said. "It becomes a very significant stumbling block, and most clinicians won't take the time to do that," if they aren't already filing paperwork to conduct a research project, he said.
Get the world’s most fascinating discoveries delivered straight to your inbox.
"It's really made a limited-availability procedure basically unavailable for a period of time," said Dr. Trevor Van Schooneveld, an assistant professor of infectious disease at the Nebraska Medical Center's Department of Internal Medicine.
The FDA's goal to make the procedure safe is an excellent one, Van Schooneveld said, but "to just basically stop people from being able to do it, without guidance on where to go from here, is unfortunate."
In an emergency (when the patient's condition is life-threatening) the FDA can give a special approval for the procedure over the telephone without needing the paperwork. But doctors will still have to complete the application eventually, so it doesn't eliminate the extra work, Bakken said.
The spectrum of disease among patients who are candidates for fecal transplantation ranges from recurrent diarrhea that lasts for years, to life-threatening complications that may require the removal of the colon, Bakken said.
C. difficile causes 14,000 American deaths each year, according to the Centers for Disease Control and Prevention.
Many patients already have trouble accessing the procedure because it is not always covered by insurance.
Although more than 700 fecal transplants have been preformed — some going back to the 1950s — the FDA still has questions about the long-term effects of the treatment, Bakken said. More studies are needed that randomly assign patients to receive either fecal transplants or an alternative treatment to better understand the side effects, Bakken said.
Once such studies have been conducted, the FDA could approve fecal transplants as a treatment of C. difficile if there appear to be no adverse effects, he said.
Until then, groups such as the Infectious Disease Society of America, the American Gastroenterological Association and the Centers for Disease Control and Prevention are discussing how they can provide the transplants so that those who need them can get them, Bakken said.
Follow Rachael Rettner @RachaelRettner. Follow MyHealthNewsDaily @MyHealth_MHND, Facebook & Google+. Originally published on LiveScience.

Rachael is a Live Science contributor, and was a former channel editor and senior writer for Live Science between 2010 and 2022. She has a master's degree in journalism from New York University's Science, Health and Environmental Reporting Program. She also holds a B.S. in molecular biology and an M.S. in biology from the University of California, San Diego. Her work has appeared in Scienceline, The Washington Post and Scientific American.


