'Excessive wrinkling' on young man's hands turned out to be rare condition
The odd symptoms were triggered by contact with water.

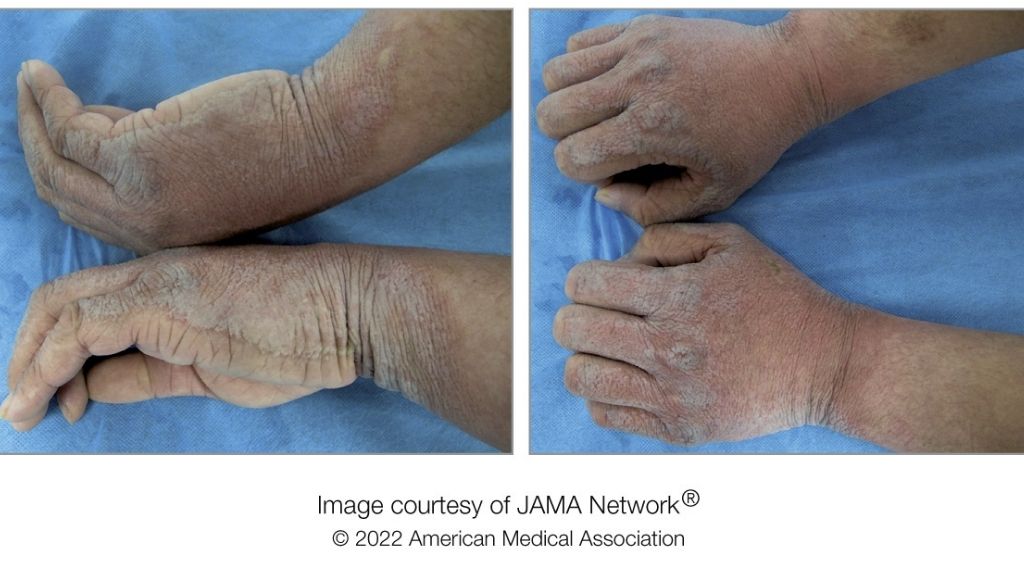
A man in his 20s developed "excessive wrinkling"; bright, white bumps; and patches of thick skin on his hands whenever he immersed them in water. Doctors initially thought the condition might be a symptom of chronic eczema, but they later determined that the wrinkling was caused by a rare skin disease, according to a new report of his case.
The disease, known as aquagenic syringeal acrokeratoderma (ASA), mostly occurs in young women, according to the report, which was published Wednesday (March 23) in the journal JAMA Dermatology. It's also fairly common in people with cystic fibrosis, a genetic disorder that affects hormone-producing glands in the body and causes mucus-producing organs to produce abnormally thick, sticky mucus, according to the Genetic and Rare Diseases Information Center (GARD).
People with cystic fibrosis carry two defective copies of the cystic fibrosis transmembrane conductance regulator (CFTR) gene, but even people who have just one copy of this gene and who don't have cystic fibrosis are prone to the condition, which hints that ASA may be partially caused by a genetic mutation. That said, the exact cause of ASA is unknown, but theories suggest that the condition may have something to do with abnormal sweat glands, according to GARD.
In the case of the young man with wrinkly hands, he reported to the dermatology department at The First Hospital of China Medical University in Shenyang after having experienced this condition for three years. The skin of his hands would become thick, swollen, wrinkly and scaly after being in water, and these changes would be accompanied by an itchy, burning sensation.
Related: 27 oddest medical cases
"It is easy to misdiagnose ASA as eczema when the clinical features first appear," the man's doctors noted in the report. Previously, at a different clinic, the man had been diagnosed with chronic eczema and intermittently treated with topical tretinoin ointment, which is often used to treat fine wrinkles, dark spots and acne; he saw little improvement with this treatment, the report notes.
Although the ASA symptoms initially affected only his hands, the man noted that, in the past year and a half or so, the condition had also spread to his wrists and elbows. "He attributed these changes to the need for washing hands frequently in the period of the COVID-19 epidemic," doctors wrote in the report. Upon closer examination, the doctors determined that the sweat glands and pores on the man's hands would become unusually large and dilated after exposure to water.
Get the world’s most fascinating discoveries delivered straight to your inbox.
"The patient's clinical process was quite interesting," the authors of the new report wrote. "The lesions only appeared after immersion in water, disappeared about 30 minutes after drying, and no lesions occurred with the absence of water contact." These short-lived symptoms are a telltale sign of ASA known as "hand in the bucket sign."
RELATED STORIES
ASA usually affects the palms of the hands, but the man had an unusual case in that his palms were spared, "which, to our knowledge, has previously not been reported," the authors noted.
The patient was treated with topical hydrocortisone urea ointment, which is both a corticosteroid and a moisturizer, and he was told to avoid unnecessary contact with water. "The symptoms had greatly improved after one month, and he is still in follow-up as of this writing," according to the case report.
Other common treatments for ASA include the common acne medications salicylic acid ointment and tazarotene gel, which encourage skin cell turnover, and aluminum chloride, which is used to control excessive sweating, according to the report. And "in most cases, it does not need any treatment and resolves spontaneously," according to GARD.
"The COVID-19 pandemic outbreak has brought changes in lifestyle, including long-term glove wearing and frequent hand washing, causing longer duration of water contact," the case report concluded. "So dermatologists should be more aware of the prevalence of ASA and help to prevent and diagnose this condition during the pandemic period."
Originally published on Live Science.

Nicoletta Lanese is the health channel editor at Live Science and was previously a news editor and staff writer at the site. She is a recipient of the 2026 AHCJ International Health Study Fellowship, with a project focused on antibiotic stewardship practices in Japan and the U.S. They hold a graduate certificate in science communication from UC Santa Cruz and degrees in neuroscience and dance from the University of Florida. Beyond Live Science, Lanese's work has appeared in The Scientist, Science News, the Mercury News, Mongabay and Stanford Medicine Magazine, among other outlets. Based in NYC, she also remains involved in dance and performs in local choreographers' work.