New Device Sees Bacteria Behind the Eardrum

At one time or another, everyone has experienced a doctor sticking an otoscope into their ears. What exactly does the doctor see? Not enough, it turns out. Hiding behind the eardrum, bacteria or other microorganisms can form a thin film, called a biofilm, that can cause chronic ear infections. A new device sees behind the eardrum to detect these problematic biofilms.
"We know that antibiotics don't always work well if you have a biofilm, because the bacteria protect themselves and become resistant," said University of Illinois electrical and computer engineering professor Stephen Boppart. "In the presence of a chronic ear infection that has a biofilm, the bacteria may not respond to the usual antibiotics, and you need to stop them. But without being able to detect the biofilm, we have no idea whether or not it's responding to treatment."
Ear infections are the most common conditions that pediatricians treat. Chronic ear infections can damage hearing and often require surgery to place drainage tubes in the eardrum, and problems can persist into adulthood. Invasive tests can provide evidence of a biofilm, but are unpleasant for the patient and cannot be used routinely.
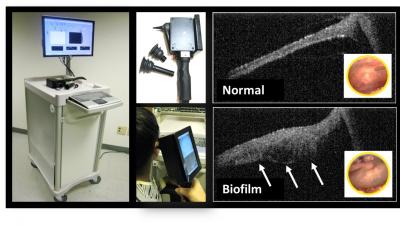
Article continues belowThe new device is an application of a technique called optical coherence tomography (OCT), a non-invasive imaging system devised by Boppart's group. It uses beams of light to collect high-resolution, three-dimensional tissue images, scanning through the eardrum to the biofilm behind it – much like ultrasound imaging, but using light.
"We send the light into the ear canal, and it scatters and reflects from the tympanic membrane and the biofilm behind it," said graduate student Cac Nguyen, the lead author of the paper. "We measure the reflection, and with the reference light we can get the structure in depth."
"I think this is now a technology that allows physicians to monitor chronic ear infection, and examine better ways to treat the disease," Boppart said"We can use different antibiotics and see how the biofilm responds."
Further study will investigate different ear pathology, comparing acute and chronic infections to examine the relationship between biofilms and hearing loss. The researchers hope that improved diagnostics will lead to better treatment and referral practices.
Get the world’s most fascinating discoveries delivered straight to your inbox.
The device is detailed this week in the Proceedings of the National Academy of Sciences.
