Gout: Causes, Symptoms and Treatment
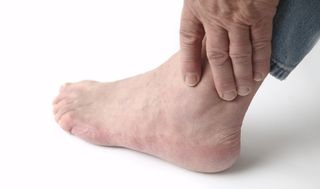
Also called "gouty arthritis," gout is a painful form of arthritis caused by too much uric acid in the body.
The painful flare-ups may be concentrated in the big toe (a symptom known as podagra), as well as swelling and pain in the ankles, knees, feet, wrists or elbows. Flare-ups last days in the beginning, but can become progressively longer. Left untreated, gout can cause permanent damage to joints and kidneys, according to the National Institutes of Health (NIH).
Gout is most commonly seen in men, particularly those between the ages of 40 and 50. It is a very common disease. Six million adults age 20 and older have reported being diagnosed with gout according to the National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS).
"Gout is the most common form of inflammatory arthritis. It is caused by an elevation of serum uric acid levels that cause crystals to accumulate in the joints, which bring on a gout flare," Dr. N. Lawrence Edwards, professor of medicine, rheumatology and clinical immunology at the University of Florida and chairman and CEO of the Gout & Uric Acid Education Society, told Live Science.
Causes
Uric acid is a waste product created during the normal breakdown of purines, naturally occurring substances found in foods such as liver, mushrooms, anchovies, mackerel and dried beans according to the NIAMS.
Uric acid is normally cleaned out of the blood by the kidneys, and passes out of the body along with urine. However, high levels of uric acid can accumulate in the body, either when the kidneys excrete too little uric acid or when the body produces too much uric acid. This condition is known as hyperuricemia, according to the NIH.
The high concentration of uric acid in the blood will eventually convert the acid into urate crystals, which can then accumulate around the joints and soft tissues. Deposits of the needle-like urate crystals are responsible for the inflammation and the painful symptoms of gout.
There are several factors that can make a person more susceptible to gout, according to the NIH. A few are:
- Having a family history of gout
- Being overweight
- Having kidney problems
- Lead exposure
- Drinking too much alcohol
- Taking certain medications like diuretics or niacin
While gout can be painful on its own, it has also been linked other conditions, such as cardiovascular disease, hypertension, diabetes and kidney disease.
For example, gout may be a risk factor in women for incident coronary heart disease, according to the Annuals of Rheumatic Disease. A study published by the online journal Vascular Specialist in 2015 found that gout predicted an increased risk of any vascular event and of coronary heart disease and peripheral vascular disease. The risk was found to be higher in women, though. In many cases, it is unclear if the link is due to excess uric acid in the body or something else.
Symptoms
According to the Mayo Clinic, common symptoms of gout are:
- Intense joint pain that is most severe in the first 12 to 24 hours
- Joint pain that lasts a few days to a few weeks and spreads to more joints over time
- Redness, tenderness and swelling of the joints
Gout vs. rheumatoid arthritis
Gout and rheumatoid arthritis (RA) both cause bumpy, painful joints, but they couldn't be more different. Rheumatoid arthritis is a disease in which the body's immune system attacks itself, causing damage to tissue and organs while gout has nothing to do with the immune system. "Unfortunately, when chronic, it can involve many joints making it difficult to distinguish from rheumatoid arthritis," Dr. Nathan Wei, a rheumatologist and director of the Arthritis Treatment Center in Frederick, Maryland, told Live Science. "Obviously, if the patient has a high level of rheumatoid factor and anti-CCP, that helps. However, a few patients may have concomitant RA and gout."
Gout vs. Pseudogout
Gout and pseudogout closely resemble each other, but they each have very different characteristics. "The amount of pain suffered by a patient with pseudogout is usually less than is experienced by a gout patient," Edwards said. "The main difference between gout and pseudogout are the types of crystals that deposit into the joints and cause inflammation." Edwards went on to point out that monosodium urate (MSU) crystals cause gout, while pseudogout is caused by calcium pyrophosphate crystals.
Test and diagnosis
While gout has painful and distinctive symptoms during flare-ups, its symptoms can be vague during other times. A doctor may extract a sample of joint fluid so it can be examined under a microscope for any presence of urate crystals, according to the NIAMS.
Certain joint infections can produce symptoms similar to gout. If an infection is suspected, the doctor may check joint fluid for bacteria.
Blood tests can reveal the concentration of uric acid in the blood and further confirm the diagnosis. However, according to the Mayo Clinic, blood tests can be misleading, because some gout patients do not have an unusual level of uric acid in their blood, and some people with high levels of uric acid do not go on to develop gout.
Other than a blood test and joint fluid tests, X-rays, ultrasounds and CT scans may be used to confirm a diagnosis.
Treatment and prevention
"A patient’s gout will not get better until they start taking uric-acid-lowering drugs. Patients need to know that their serum uric acid level should be below the target of 6 milligrams per deciliter (mg/dL). While gout cannot be cured, it can be better managed, or even controlled completely, with the right medications and lifestyle choices," Edwards said.
In most cases, long-term medications for lowering uric acid will be used to treat gout and prevent flares gout. "Generally, patients with gout will need to be on these drugs for life. If they stay on them over time, their gout symptoms and risk of deformity or disability will be greatly decreased," Edwards added.
The painful symptoms of gout can be alleviated by nonsteroidal anti-inflammatory drugs (NSAIDs), which can reduce both pain and inflammation around the joints, according to the University of Maryland. Depending on the severity of the flare-ups, patients can be treated with over-the-counter NSAIDs such as ibuprofen (Advil or Motrin), or naproxen (Aleve) or with prescription-strength painkillers such as indomethacin (available under the trade name Indocin).
Corticosteroids, such as prednisone, can be injected directly into the affected joints for relief within a few hours, according to Mayo Clinic. However, despite their effectiveness, corticosteroids must be used sparingly, because they can weaken bones or poor wound healing.
Another pain reliever commonly used to reduce gout pain is colchicine. It is most effective when taken within the first 12 hours of symptoms, according to NIAMS. Once the flare-up subsides, the doctor may prescribe low, daily doses of colchicine to ward off future attacks.
Beyond medications, patients can also control the frequency of flare-ups through exercise and diet adjustments. Because uric acid is created during the digestion and breakdown of purines, patients can reduce the concentration of uric acid in the blood by avoiding high-purine foods such as anchovies, asparagus, dried beans and peas, mushrooms and organ meats (such as livers and kidneys). The Mayo Clinic also suggests that patients should drink more water and less alcohol, because alcohol can raise the level of uric acid in the blood.
This article is for informational purposes only, and is not meant to offer medical advice.
Additional resources
Sign up for the Live Science daily newsletter now
Get the world’s most fascinating discoveries delivered straight to your inbox.

