'Brain-eating' amoeba ruled out in 'cluster of illnesses' in Oklahoma. What could the cause be?
Oklahoma's state health department is investigating a cluster of illnesses in people who swam in local lakes and rivers. The cause remains unknown, but a dangerous brain-eating amoeba has been ruled out.

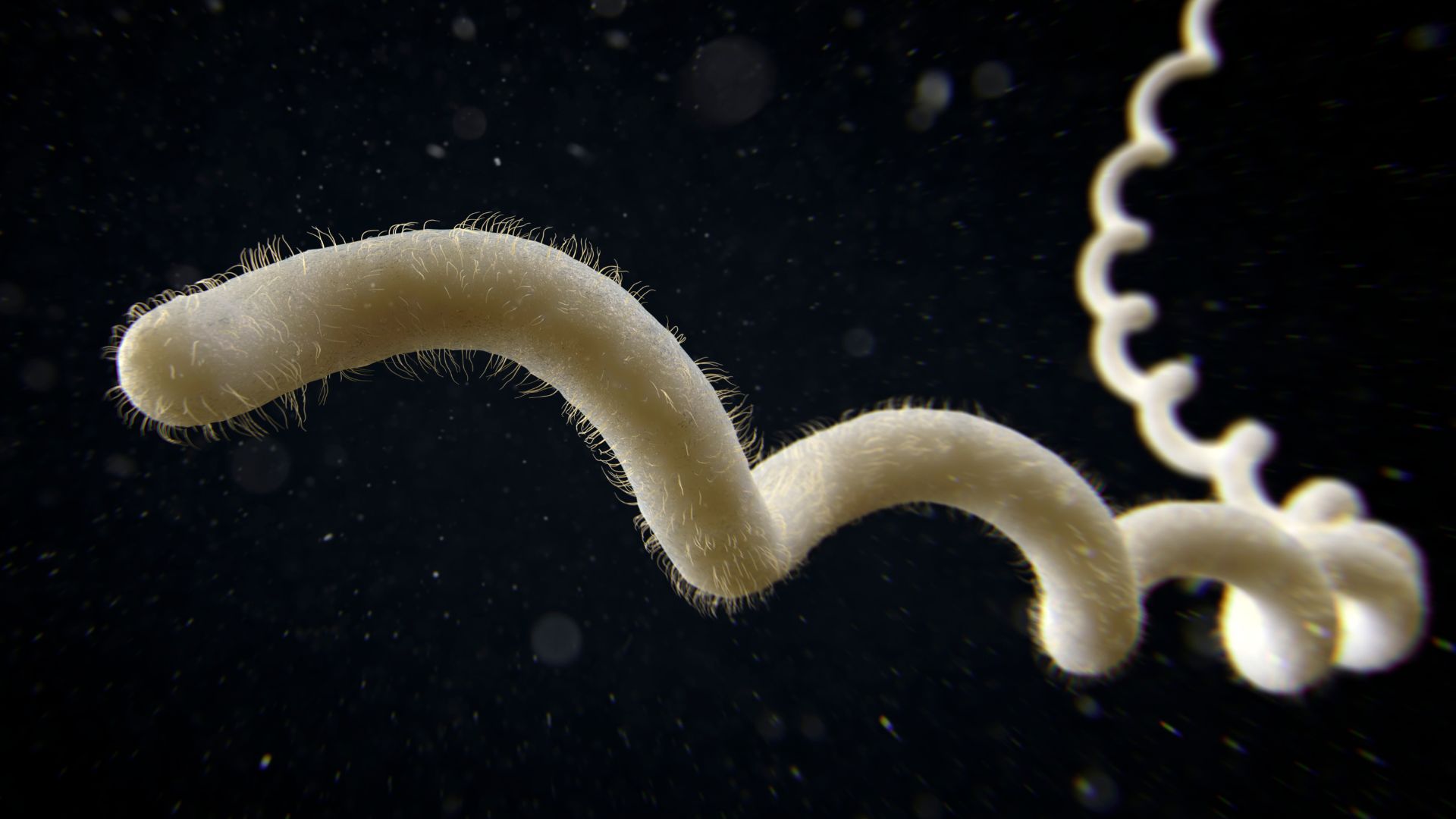
A "cluster of illnesses" in Oklahoma has an unknown cause. An expert told Live Science that Leptospira bacteria (pictured) could be a potential culprit.
State and federal health officials are investigating the cause of a "cluster of illnesses" in Bartlesville, Oklahoma. Early analyses have ruled out the freshwater-residing "brain-eating amoeba" Naegleria fowleri, known for causing a rare but nearly always fatal brain infection called primary amebic meningoencephalitis (PAM), as a potential cause, Oklahoma State Department of Health (OSDH) officials told Live Science in an emailed statement.
"What we know at this time is a few individuals have presented to healthcare providers with varying symptoms," and tests for PAM caused by N. fowleri have been negative, the statement reads. The OSDH is currently investigating the reports and working alongside the Centers for Disease Control and Prevention (CDC) to conduct further tests.
The OSDH statement does not provide more information about the cases, but according to FOX 23, several affected individuals reportedly got sick after swimming in Copan Lake or the Caney River, and at least one child is reportedly being treated in the hospital for suspected bacterial meningitis.
The OSDH has advised residents that public drinking water is safe and that it is tested daily to ensure federal and state quality standards are met.
Related: 'Brain-eating' amoebas are a new concern in northern US states, health officials advise
Meningitis is the inflammation of the layer covering the brain; it leads to symptoms such as headache, stiff neck and light sensitivity, and severe cases can cause seizures, coma and death. Meningitis can be caused by bacteria, viruses or amoebas like N. fowleri infecting the central nervous system; severe cases tend to be caused by bacteria or amoebas rather than by viruses.
It is uncommon to contract meningitis from freshwater. When it does happen, N. fowleri is usually the culprit and, on average, two to three cases of PAM are reported in the U.S. each year. In those cases, patients have usually come into contact with the amoeba after inhaling contaminated water through their noses.
Get the world’s most fascinating discoveries delivered straight to your inbox.
With N. fowleri ruled out as a possible cause of the recent illnesses in Bartlesville, what else could cause meningitis following exposure to freshwater?
According to Dr. Thomas Russo, a professor and chief of infectious diseases in the Jacobs School of Medicine and Biomedical Sciences at the University at Buffalo, the most likely culprit behind the recent cluster of illnesses is bacteria in the genus Leptospira. Exposure to this pathogen can cause an infection called leptospirosis, which can lead to meningitis.
According to the CDC, the urine of infected animals can enter water sources, where the bacteria can then linger for months. Swallowing or bathing with an open wound in water contaminated with Leptospira gives the pathogen an entry point into the body. In the U.S., around 100 to 150 cases of leptospirosis are reported each year, although some of these are caused by contact with infectious urine or consumption of contaminated food.
Enteroviruses present another plausible cause. These are "a group of viruses that cause a number of infectious illnesses, which are usually mild," Russo told Live Science. For example, enteroviruses can cause the common cold and various gastrointestinal symptoms. Enteroviruses can enter freshwater sources via fecal runoff contamination.
"If the water was contaminated with an enterovirus and was ingested, it could potentially cause a meningitis syndrome," Russo said. Infections with enteroviruses are fairly common, but most people who come into contact with an enterovirus don't develop a clinical disease; illnesses that do arise tend to resolve on their own.
Listeria bacteria, a rare but sometimes fatal cause of food poisoning, can also result in meningitis. These bacteria can be found in moist environments, soil, water and animal feces. Certain groups are at a greater risk of illness from exposure to Listeria, including children 6 months old or younger, pregnant people, and people with compromised immune systems.
Balamuthia mandrillaris, an amoeba that is common in freshwater, soil, dust, sewage, swimming pools, water storage, and humidifiers, can cause a rare but serious brain infection called granulomatous amebic encephalitis (GAE). The amoeba can enter the body through broken skin or via inhalation through the nose. Since its discovery in 1896, only 200 cases have been confirmed worldwide, although half of these occurred in the U.S.
RELATED STORIES
Another amoeba, Acanthamoeba, can also cause GAE, although fewer than 50 such cases of GAE have been reported in the literature. The amoeba can be found in swimming pools, lakes, tap water, and heating and air conditioning units. While most people will be exposed to the pathogen at some point in their life, very few will develop an illness — those with a compromised immune system are at most risk of falling ill.
It is also possible for an unknown pathogen to cause meningitis following contact with water, Russo said, and there's a chance that the cases reported in Bartlesville are not related to one another or to the individuals' recent swimming history. So far, limited information has been made publicly available regarding the number of cases and the symptoms or diagnoses of those afflicted. Therefore, it is not possible to conclude the cause of the illnesses, Russo said.
Because of their increased risk of illness when exposed to pathogens, people who are pregnant or have compromised immune systems should consider avoiding swimming in freshwater, according to Russo. Anyone swimming in freshwater should also avoid swallowing the water or allowing it to enter their nose.
Sarah Moore is a freelance science writer. She has an MSc in neuroscience and a BSc in psychology from Goldsmiths College, University of London. Sarah has experience in academic research and has worked in medical communications with top pharmaceutical companies. As a freelancer, she has contributed work to a wide range of publications. Sarah loves to write on all areas of science, from healthcare to nanotechnology but she is especially intrigued by the workings of the human brain.
