Women's Genes May Increase Risk of Birth Control Failure, Study Suggests

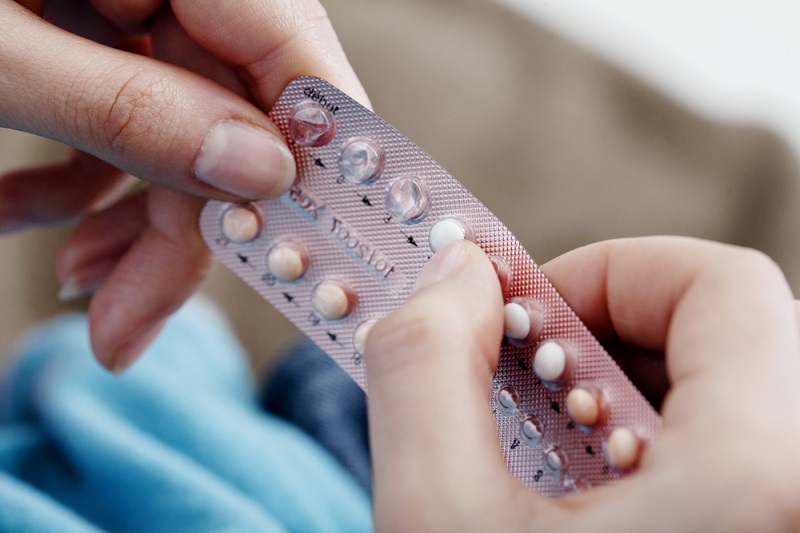
When a woman gets pregnant while on the pill or other hormonal birth control, doctors often assume she didn't use the contraceptive properly. But a new study suggests that, in some cases, a woman's genes may put her at risk for an unplanned pregnancy even while using hormonal birth control properly.
The study found that, while on hormonal birth control, women with a relatively rare version of a gene called CYP3A7 tended to have lower blood levels of the hormones needed for the birth control to work, compared with women who had more common versions of the gene.
The CYP3A7 gene codes for a liver enzyme that's typically active only in fetuses and is switched off before birth, the researchers said. But in some people, the gene stays active, which in turn leads to a faster breakdown of hormones found in contraception, such as estrogen and progestin. The researchers hypothesize that this faster breakdown may increase a woman's pregnancy risk while on birth control, particularly if she is using a low-dose hormonal contraception.
Article continues below"When a woman says she got pregnant while on birth control, the assumption was always that it was somehow her fault," study lead author Dr. Aaron Lazorwitz, an assistant professor of obstetrics and gynecology at the University of Colorado School of Medicine in Denver said in a statement. "But these findings show that we should listen to our patients and consider if there is something in their genes that caused this [unplanned pregnancy]." [5 Myths About Women's Bodies]
Still, more research is needed to confirm the results and find other genes that may also increase the risk of hormonal contraception failure. But if true, doctors might one day consider genetically testing women for these genes if they become pregnant while on birth control, the researchers said.
The study was published online today (March 12) in the journal Obstetrics & Gynecology.
Birth control and genetics
Hormonal contraceptives are one of the most commonly prescribed medications in the U.S. If used exactly as directed, birth control pills are about 99 percent effective at preventing pregnancy, according to Planned Parenthood. However, about 9 out of 100 women who use birth control pills get pregnant each year, which has been thought to be due to factors such as missed pills.
Get the world’s most fascinating discoveries delivered straight to your inbox.
But few studies have looked at whether a woman's genes affect her response to the medications.
In the new study, the researchers looked at data from 350 healthy women, average age of 22 years, who had a contraceptive implant inserted into their arms for at least one year. The device releases a steady dose of the hormone progestin to prevent pregnancy. The researchers chose to study women with the implant to assure that participants were getting a consistent dose of hormones without the need to remember to take a daily pill (as is the case with hormonal birth control pills.)
The authors found that about 5 percent of participants (18 women) had a variant of the CYP3A7 gene known as CYP3A7*1C and had levels of the hormonal medication in their blood that were, on average, 23 percent lower than participants with a more common gene variant.
In addition, among the 18 people with CYP3A7*1C, five (28 percent) had levels of medication in their blood that were below the threshold of the amount doctors deem necessary for the medication to work properly.
Future studies
The researchers hypothesize that the findings will also apply to women on hormonal birth control pills because hormones in the implant and in the pill are similar, and are broken down similarity in the body, Lazorwitz said. But future studies of women on birth control pills are needed to show this, he said.
Another question for future research will be whether CYP3A7*1C carriers who take hormonal birth control have a higher-than-average rate of unplanned pregnancies.
"At this point, it is too early to say that CYP3A7*1C carriers have a certain risk of contraceptive failure, as [more research] is needed to really quantify what that risk may be," Lazorwitz told Live Science.
In addition, most participants in the report identified as Caucasian or Hispanic/Latina; further study of other women is needed to determine if there may be genes more common in these groups that are also tied to contraception failure.
- Beyond Birth Control: 5 Conditions 'The Pill' Can Help Treat
- 7 Facts Women (And Men) Should Know About the Vagina
- Birth Control Quiz: Test Your Contraception Knowledge
Originally published on Live Science.

Rachael is a Live Science contributor, and was a former channel editor and senior writer for Live Science between 2010 and 2022. She has a master's degree in journalism from New York University's Science, Health and Environmental Reporting Program. She also holds a B.S. in molecular biology and an M.S. in biology from the University of California, San Diego. Her work has appeared in Scienceline, The Washington Post and Scientific American.