An Expanding Alternative to High-Risk Heart Valve Surgery (Op-Ed)
Get the world’s most fascinating discoveries delivered straight to your inbox.
You are now subscribed
Your newsletter sign-up was successful
Want to add more newsletters?
Join the club
Get full access to premium articles, exclusive features and a growing list of member rewards.
Dr. Juan Crestanello is a cardiothoracic surgeon at The Ohio State University Wexner Medical Center. He contributed this article to LiveScience's Expert Voices: Op-Ed & Insights.
When patients hear that they have a problem with their heart, they often think it's a worst case scenario. However, thousands of heart procedures are performed every day in this country, and most patients do not realize some incredible advancements have emerged.
For patients considering one common procedure, traditional heart-valve replacement surgery, there is an emerging alternative for patients at high risk for complications or who are otherwise not candidates for that surgery.
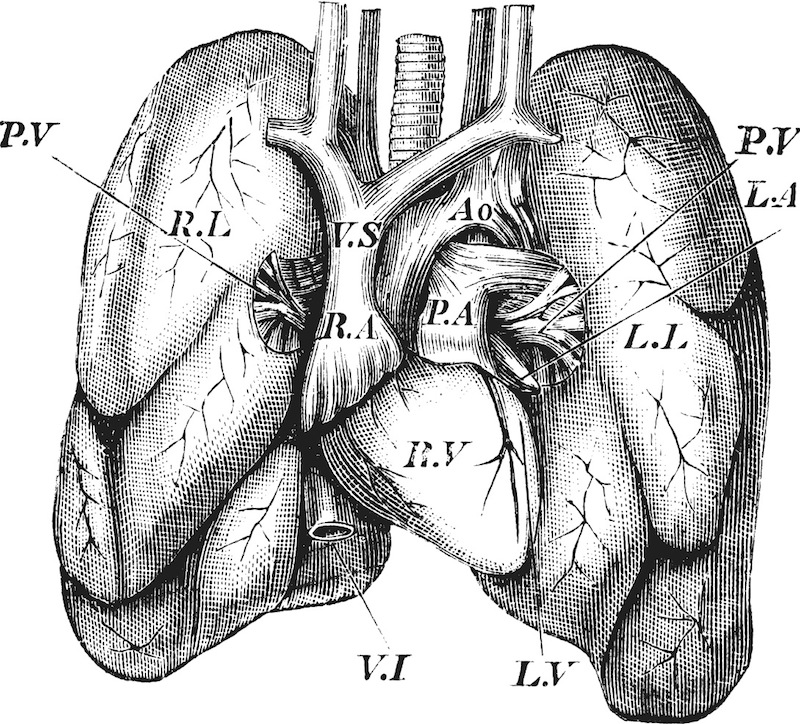
Heart valves generally need replacing when aortic valve disease damages aging hearts. With each heartbeat, the aortic valve opens and closes to allow blood to flow out of the heart. If the valve malfunctions, it can slow blood flow and won't allow blood to come out of the heart. This is called aortic valve stenosis. Those with aortic valve disease may need to have the valve replaced. If you have been diagnosed with severe aortic stenosis, you may be a candidate for that procedure.
Previously, this procedure would have required open-heart surgery, which may not be an option for many patients who are frail or have co-morbidities that make them poor surgical candidates. In the past, these patients were often told there would be nothing left to do in order to treat the problem.
Now, at The Ohio State University's Ross Heart Hospital, we are performing transcatheter aortic valve replacement, a minimally invasive procedure which allows the aortic valve to be replaced through a catheter approach. First, a balloon valvuloplasty is performed. Typically, the surgeon makes a small incision in the groin area and inserts a catheter (a thin, flexible tube) with a small, deflated balloon attached to the tip, threading the catheter through a blood vessel. Once the catheter reaches the damaged heart valve, the surgeon inflates the balloon to stretch the valve opening and allow more blood to flow through it. The balloon is then deflated and removed. [Amazing Images: Heart Shapes in Nature ]
Then, the surgeon inserts a new catheter containing the new heart valve into the blood vessel. The replacement device is threaded through the blood vessels to the heart and into the damaged heart valve where it is released. The new heart valve will take the place of the damaged one, allowing the blood to flow normally out of the heart and through the body.
Get the world’s most fascinating discoveries delivered straight to your inbox.
This procedure benefits patients because it is less invasive, there are smaller incisions and it offers a quicker recovery and a shorter hospital stay than conventional open-heart surgery. The procedural outcomes are comparable to those of conventional surgery — improved quality of life for patients who previously suffered from debilitating shortness of breath, chest pain and/or fatigue.
Since 2011, The Ohio State University Wexner Medical Center has been one of only a few centers in its region that offers this cutting-edge alternative for patients who are considered inoperable or at high risk for conventional surgery. Patients undergoing this procedure at Ohio State may receive one of two devices: In addition to the Edwards SAPIEN transcatheter heart valve, which is U.S. Food and Drug Administration-approved for high-risk cases, patients also have unique access to the Medtronic CoreValve System, which is being studied by clinical trial in the United States. Ohio State had among the highest enrollments in the high-profile Medtronic CoreValve U.S. Pivotal Trial and among the first 20 U.S. centers to participate in the Surgical Replacement and Transcathether Aortic Valve Implantation (SURTAVI) Trial, giving patients opportunities not available in most hospitals.
For most of the patients we treat, it is their only option. They all have co-morbidities — previous surgeries, strokes and many other conditions that would make traditional open-heart surgery too risky. Without this less-invasive option, they would not survive. In the last two years, more than 100 patients have undergone the procedure at Ohio State, and the program is growing as more practitioners become aware of this new treatment option for valve replacement.
The views expressed are those of the author and do not necessarily reflect the views of the publisher. This version of the article was originally published on LiveScience.
 Live Science Plus
Live Science Plus