Maggots Clean Wounds Faster Than Surgeons
Get the world’s most fascinating discoveries delivered straight to your inbox.
You are now subscribed
Your newsletter sign-up was successful
Want to add more newsletters?
Join the club
Get full access to premium articles, exclusive features and a growing list of member rewards.
The idea of putting maggots into open flesh may sound repulsive, but such a therapy might be a quick way to clean wounds, a new study from France suggests.
Men in the study, all of whom had wounds that wouldn't heal, were randomly assigned to have dead and unhealthy tissue removed from their lacerations by either standard surgical therapy or maggots (that eat dead tissue).
After about a week, men who received the maggot therapy had less dead tissue in their wounds than men who underwent surgery, the researchers said.
Article continues belowHowever, after two weeks, the immature insects had lost their advantage: Both groups had about an equal amount of dead tissue in their wounds. And in the end, the maggots did not help the wounds heal faster.
Although the effects of maggot therapy were not dramatic, it may be useful in certain cases, such as in patients with diabetes, whose wounds need rapid control, the researchers said. But continuing the maggot therapy beyond one week is not of benefit, they said.
Maggot medicine
Medical use of maggots was approved in 2004 by the U.S. Food and Drug Administration. However, only a small minority of patients with unhealing wounds receive the treatment, said Dr. Robert Kirsner, a dermatologist at the University of Miami School of Medicine, who was not involved in the new study.
Get the world’s most fascinating discoveries delivered straight to your inbox.
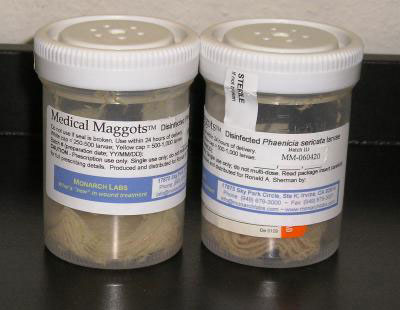
The study included about 100 men with wounds on their lower limbs. About half received maggot therapy and half received surgical treatment. For the maggot therapy, sterile maggots were placed in a small pouch that was placed on top of the wound. The therapy was applied twice a week for two weeks.
Neither the patients nor the doctor evaluating the wounds knew which therapy a patient received (patients wore a blindfold when their bandages were changed.)
After eight days, the percentage of dead tissue in the wounds of patients who received the maggot therapy was 54.5 percent, compared with 66.5 percent in patients who received surgery. But after 15 days and 30 days, the amount of dead tissue in the wounds was about the same for both groups.
The number of patients who reported feeling a crawling sensation in their wound, and the number reporting pain, was also about the same in both groups, according to the study, which was conducted by researchers at the University Hospital Center of Caen, in France.
Gross factor
Maggots secrete an enzyme that dissolves dead tissue but leaves healthy tissue alone, Kirsner said.
Although there are few risks to the treatment, "there is a gross factor to it," Kirsner said. "Patients have to be very psychologically strong," he said.
Another group of patients that may benefit from the therapy are those who cannot undergo surgery, for instance, if they cannot receive anesthesia, Kirsner said.
Future research should determine whether the effects of maggot therapy can be improved using more maggots, and whether an increase in the number of critters would be painful, the researchers said.
The study is published online today (Dec. 19) in the journal Archives of Dermatology.
Pass it on: Maggots can remove dead tissue from wounds more quickly than standard treatments, but the therapy has no superior benefit beyond one week.
This story was provided by MyHealthNewsDaily, a sister site to LiveScience. Follow MyHealthNewsDaily staff writer Rachael Rettner on Twitter @RachaelRettner. Find us on Facebook.

Rachael is a Live Science contributor, and was a former channel editor and senior writer for Live Science between 2010 and 2022. She has a master's degree in journalism from New York University's Science, Health and Environmental Reporting Program. She also holds a B.S. in molecular biology and an M.S. in biology from the University of California, San Diego. Her work has appeared in Scienceline, The Washington Post and Scientific American.
 Live Science Plus
Live Science Plus