U.S. woman with COVID-19 receives double-lung transplant in a first
The recipient was an otherwise healthy woman in her 20s.

In a first, a young COVID-19 patient in the U.S. has received a double-lung transplant after the coronavirus ravaged her lungs.
The patient, a Hispanic woman in her 20s, spent six weeks in the intensive care unit at Northwestern Memorial Hospital in Chicago after developing severe COVID-19, according to a statement from Northwestern Medicine. She was hooked up to a ventilator and an extracorporeal membrane oxygenation (ECMO) machine to keep her heart and lungs going.
But by early June, her lungs showed irreversible damage, and she was placed on the waiting list for a double-lung transplant, according to the statement. Double-lung transplants — in which both lungs are replaced with healthy ones from donors who have died — were first performed in the 1960s, but didn't become widespread until the 1990s, according to Harvard Medical School.
Related: 13 coronavirus myths busted by science
Though survival has improved over time, lung transplants remain "very risky" compared with kidney or heart transplants, according to Harvard. This is the first time that the procedure has been performed on a patient with COVID-19, the disease caused by SARS-CoV-2.
Before she could receive the procedure, however, the patient had to test negative for the virus, according to the statement. (Lung transplants aren't usually given to people with active infections, according to The Mayo Clinic. That's because patients must take immune-suppressing drugs after the operation).
"For many days, she was the sickest person in the COVID ICU — and possibly the entire hospital," Dr. Beth Malsin, a pulmonary and critical care specialist at Northwestern Memorial Hospital, said in the statement. "There were so many times, day and night, our team had to react quickly to help her oxygenation and support her other organs to make sure they were healthy enough to support a transplant if and when the opportunity came."
Get the world’s most fascinating discoveries delivered straight to your inbox.
"One of the most exciting times was when the first coronavirus test came back negative and we had the first sign she may have cleared the virus to become eligible for a life-saving transplant," she added.
The surgery took 10 hours, several hours longer than normal because the inflammation caused by COVID-19 had left her lungs "completely plastered" to the tissue around them, the heart, the chest wall and the diaphragm, Dr. Ankit Bharat, the chief of thoracic surgery and surgical director of the lung transplant program at Northwestern Medicine, told The New York Times. Her lung damage was one of the worst he'd ever seen.
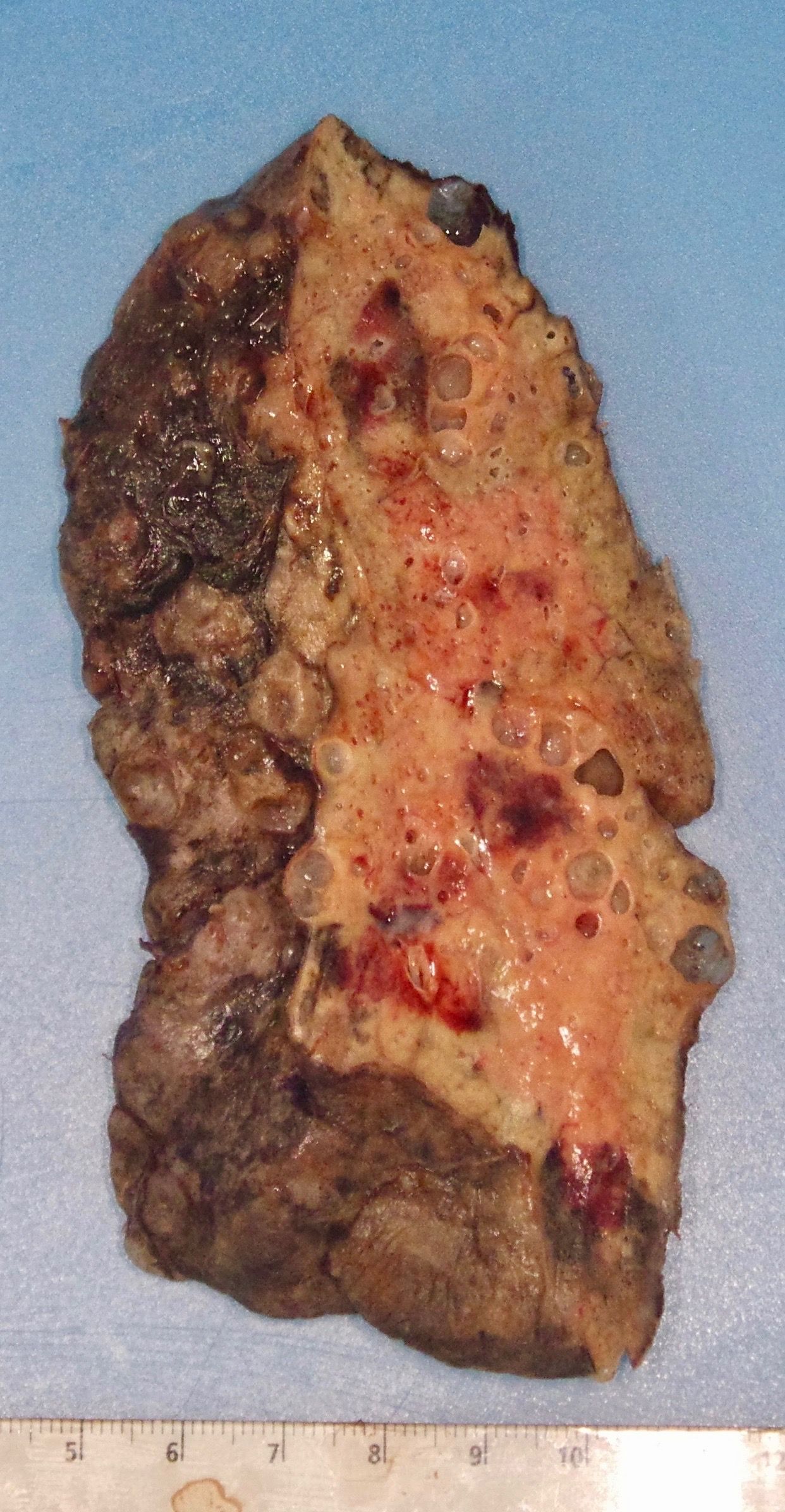
The woman had no serious underlying medical conditions, he told the Times. She was, however, taking an immune-system suppressing medication for a minor illness, he said. But it's unclear whether that drug made her more susceptible to the virus.
She is now recovering well, Bharat told the Times. "She’s awake, she's smiling, she FaceTimed with her family." But she still has a while to recover and is still on a ventilator, he said. She is now taking medication to suppress the immune system to stop the body from rejecting the lungs, which can increase the risk of infection, Bharat told the Times.
But the patient has been tested several times to see if the drugs could have reactivated the coronavirus and those tests have come back negative, according to the Times.
"A lung transplant was her only chance for survival,” Bharat said in the statement. "We want other transplant centers to know that while the transplant procedure in these patients is quite technically challenging, it can be done safely, and it offers the terminally ill COVID-19 patients another option for survival.”
Following lung transplants, more than 85% to 90% of patients survive one year and can function independently in daily life, according to the statement.
"How did a healthy woman in her 20s get to this point? There's still so much we have yet to learn about COVID-19," Dr. Rade Tomic, a pulmonologist and medical director of the Lung Transplant Program at Northwestern Medicine, said in the statement.
- 11 surprising facts about the respiratory system
- The 9 deadliest viruses on Earth
- 28 devastating infectious diseases
Originally published on Live Science.
OFFER: Save 45% on 'How It Works' 'All About Space' and 'All About History'!
For a limited time, you can take out a digital subscription to any of our best-selling science magazines for just $2.38 per month, or 45% off the standard price for the first three months.

Yasemin is a staff writer at Live Science, covering health, neuroscience and biology. Her work has appeared in Scientific American, Science and the San Jose Mercury News. She has a bachelor's degree in biomedical engineering from the University of Connecticut and a graduate certificate in science communication from the University of California, Santa Cruz.

